In this post, I’m going to do a rapid round-up of what I can find out about the monkeypox outbreak. Fortunately, from our experience with Covid, the relevant conceptual categories for potential pandemic come readily to hand, and will form the rapid-fire post headings: Symptoms and Progression, Spread, Clades, Mortality, R, Community Spread, and Mode(s) of Transmission. After taking a brief detour through Summer Festivals, I will ask “What to Do?” and conclude.
Here, however, is what Biden had to say (which gets slightly misquoted):
BIDEN: But [monkeypox] is a concern in the sense that if it were to spread, it’s consequential. That’s all they have told me.
“That’s all they have told me” doesn’t exactly inspire confidence if Klain, Walensky, and Jha are the “they,” but Biden isn’t exactly the President we want wrapped up in detail, either.
Symptoms and Progression
CDC — sorry, but what can I do? — describes the symptoms and the course of the disease:
You can recognize potential monkeypox infection based on the similarity of its clinical course to that of ordinary discrete smallpox.
After infection, there is an incubation period which lasts on average 7-14 days. The development of initial symptoms (e.g., fever, malaise, headache, weakness, etc.) marks the beginning of the prodromal period.
A feature that distinguishes infection with monkeypox from that of smallpox is the development of swollen lymph nodes (lymphadenopathy). Swelling of the lymph nodes may be generalized (involving many different locations on the body) or localized to several areas (e.g., neck and armpit).
Shortly after the prodrome [initial symptoms[, a rash appears. Lesions typically begin to develop simultaneously and evolve together on any given part of the body. The evolution of lesions progresses through four stages—macular, papular, vesicular, to pustular—before scabbing over and resolving.
This process happens over a period of 2-3 weeks. The severity of illness can depend upon the initial health of the individual, the route of exposure, and the strain of the infecting virus.
Here is an image of some lesions. You’ve probably seen some virtually pornographic sensational images, but here is a medical texbook-ish one that shows their evolution:
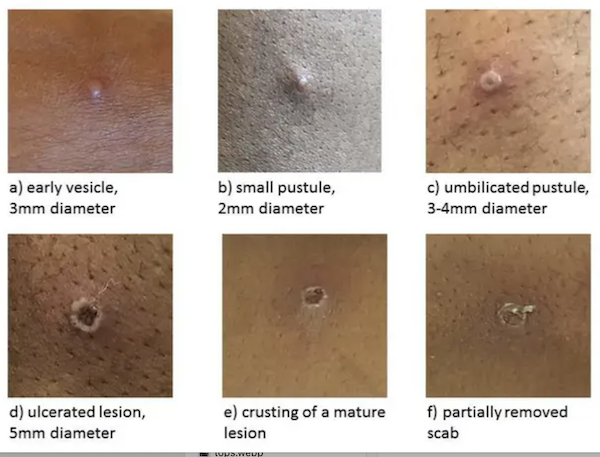
Note that the lesions on their own are not sufficient to diagnose monkeypox:
Nurses and doctors are being advised to stay ‘alert’ to patients who present with a new rash.
Monkeypox is often mistaken for more common rash illnesses like chickenpox, measles, scabies and syphilis, which makes it difficult to diagnose early.
In other words, conclusive diagnosis of monkeypox requires a test, but sadly:
Diagnostic testing for Orthopoxviruses (which includes monkeypox virus) is available at LRN [CDC Laboratory Response Network] laboratories located throughout the United States and abroad. There is no commercial assay to detect monkeypox virus.
Hospitals should contact their local or state health departments to inquire about monkeypox virus testing before contacting CDC.
Well, let’s hope that doesn’t turn out to be a problem. (But won’t this introduce severe time lags into contact tracing, if at any scale at all?)
Spread
Here is the current (and often updated) case count as of this writing:
![]()
Small, but from little acorns…
Clades
What is a clade, you ask. A clade (from Ancient Greek κλάδος (kládos) ‘branch’) is a group of organisms that is composed of a common ancestor and all its lineal descendants; as the name suggests, clades are generally represented as trees. (“SARS-CoV-2 is itself a clade within the family coronaviridae and the genus betacoronavirus.”) Here is WHO on monkeypox clades:
To date, all cases whose samples were confirmed by PCR have been identified as being infected with the West African clade.
Monkeypox is usually self-limiting but may be severe in some individuals, such as children, pregnant women or persons with immune suppression due to other health conditions. Human infections with the West African clade appear to cause less severe disease compared to the Congo Basin clade, with a case fatality rate of 3.6% compared to 10.6% for the Congo Basin clade.
Genomic sequencing of monkeypox samples is taking place, but infinite are the arguments of mages. With time, the genomics will no doubt settle out. When that happens, we’ll have a better handle on the situation:
The current outbreak has raised alarms for several reasons. For one, as countries up their surveillance efforts, more are reporting cases of the virus, which is rarely seen outside Central and West Africa. The pattern of infections indicates that the virus has been spreading undetected. It’s also not clear, for example, if the U.S. case is related to the cases in Europe. Genomic sequencing can help answer that question.
Mortality
From WHO (supported by this meta-study):
Human infections with the West African clade appear to cause less severe disease compared to the Congo Basin clade, with a case fatality rate of 3.6% compared to 10.6% for the Congo Basin clade.
So far, we’ve detected only the West African clade (see above), which is good news. In practice, the death rate could be even lower:
During a 2003 outbreak in the U.S., for example, 26% of cases were hospitalized and 15% had severe disease, but none died. Interestingly, during this outbreak, scientists found previous smallpox vaccination was not associated with severity. Also, children were more likely to be hospitalized in an ICU than adults.
On the other hand, in 2003 the general population hadn’t been weakened by a pandemic. Nor had the health care system attained it’s current level of grotesque inequity.
R
From the Daily Mail (sorry not sorry; their science coverage is generally good):
A World Health Organization report last year suggested the natural R rate of the virus – the number of people each patient would infect if they lived normally while sick – is two.
But the real rate is likely much lower because ‘distinctive symptoms greatly aid in its early detection and containment,’ the team said, meaning it’s easy to spot cases and isolate them.
It would be nice if monkeypox were infectious only when the lesions appeared. I don’t see how we can be sure about that yet, in the absence of the sort of epidemiology we’ve seen for Covid; the monkeypox equivalent of the Skagit Valley choir case, for example. So I’m a tad dubious on the containment argument.
Community Spread
There has most certainly been community spread:
“Now that there’s been community spread, it may be hard to fully snub [sic] this out. I don’t think it’s going to become a major epidemic because this is a virus that’s difficult to spread,” Gottlieb said on “Squawk Box.”
Gottlieb added that there have been numerous disconnected cases, indicating that the spread in the community is ‘pretty wide.’ He said there might be a lot more infection than what health officials have found since it has such a long incubation period and ‘doctors don’t know to look for it yet.’
He noted that the virus is endemic [yay!] in some countries, with the Democratic Republic of the Congo reporting anywhere from five to 10,000 cases a year.
Contact tracing ought to be easy:
A WHO report in 2020 explained that human-to-human transmission of the virus is rare and that the longest chain of cases appears to only have been six people before it ended.
The report said: ‘The epidemic risk for humans is considered to be small.’
But perhaps the geography of “communities” has changed:
Some experts hypothesized that the loosening of international travel restrictions may have contributed to the spread.
“It kind of looks like the virus always had this potential capacity” for human-to-human transmission, McFadden said. ‘It just never had the opportunity in the past — or if it did, it quickly petered out and we never really saw it as an event. Whereas now with people being able to travel all over the world, it’s entirely possible we’re actually seeing it for the first time in a larger context.”
A chain of cases with only six links is certainly “petering out.” But past performance is no guarantee of future results.
Mode(s) of Transmission
Here is CDC on monkeypox’s mode of transmission:
A combination of standard, contact, and droplet precautions should be applied in all healthcare settings when a patient presents with fever and vesicular/pustular rash.
In addition, because of the theoretical risk of airborne transmission of monkeypox virus, airborne precautions should be applied whenever possible.If a patient presenting for care at a hospital or other health care facility is suspected of having monkeypox, infection control personnel should be notified immediately.
I’m going to delve into aerosols just a little because with Covid, CDC butchered droplet v. aerosol tranmission so badly, once bitten, twice shy[1]. For example, UK Health Security Agency (UKHSA) treats monkeypox as airborne:
Yes, it's an airborne HCID according to UKHSAhttps://t.co/25Z8KeQQtc pic.twitter.com/Nbei8ZoYvc
— Tom Andrews💙 (@0bj3ctivity) May 21, 2022
So, at one point, did WHO:
Does the @WHO consider airborne transmission and therefore the use of respirators? In 1980 WHO did recommend respirators for Monkeypox. Why not now?https://t.co/yzXow2EhiX pic.twitter.com/tS3ACwcewP
— Lara 😷 #𝙲𝙾𝚅𝙸𝙳𝚒𝚜𝙰𝚒𝚛𝚋𝚘𝚛𝚗𝚎 (@Iamgoingtosleep) May 21, 2022
However, the aerosol community, so far, thinks not:
Chad Roy, an aerobiologist at Tulane University School of Medicine who led that study, told me that compared to the SARS-CoV-2 coronavirus, monkeypox is “an altogether different virus and the risk of natural transmission by aerosol far less likely.” And the fact remains that past monkeypox outbreaks have been inconsistent with a virus that travels as easily as the coronavirus. “Monkeypox does not scream ‘airborne’ at me; COVID-19 did,” Linsey Marr, an aerosol expert at Virginia Tech, told me.
Then again, Marr is less certain about monkeypox than she was about COVID. And Titanji notes that our knowledge of monkeypox is based on just 1,500 or so recorded cases, as of 2018. “I’ve seen a lot of people writing as if everything we know about monkeypox is definitive and finalized, but the reality is that it is still a rare zoonotic infection,” she said. For that reason, “I’m in Team Cautious,” she said. “We can’t use what happened with previous monkeypox outbreaks to make sweeping statements. If we’ve learned anything from COVID, it’s to have humility.”
Disconcertingly for droplet and close contact advocates, we have one example of tranmission on a plane:
Currently, the CDC is monitoring six people in the United States for possible monkeypox infections after they sat near an infected traveler who had symptoms while on a flight from Nigeria to the United Kingdom in early May.
However, I’m not seeing any epidemiology, like a seat diagram, as we did see for examples of plane tranmission with Covid, and we know nothing about the six people. Team Cautious is a good team to be on, as long as one plays on Team Precaution as well.
Summer Festivals
WHO has expressed concern MR SUBLIMINAL Extroverts are gonna kill us all over mass gatherings in the summer:
“As we enter the summer season in the European region, with mass gatherings, festivals and parties, I am concerned that transmission could accelerate, as the cases currently being detected are among those engaging in sexual activity, and the symptoms are unfamiliar to many,” WHO regional director for Europe Hans Kluge said in a statement.
WHO’s concern is reasonable, given events in Spain, Belgium and Quebec. Let’s take them in order, starting with Spain, the largest. From El Pais (here, but online only here):
A massive party in the town of Maspalomas, on the island of Gran Canaria, Held between May 5 and 15 and attended by nearly 80,000 people, it has become the second focus of the monkeypox outbreak in Spain, have confirmed health sources. The event was attended by several of the positive cases diagnosed in recent days in Madrid, two or three young Italian men whose infection has been confirmed in Rome and at least one case investigated on the island itself, according to these sources.
This is the second major focus of the Moorish smallpox outbreak located in Spain in recent days. The first is a place called Sauna Paraíso, located in the Malasaña neighborhood of Madrid, which was closed yesterday by the Ministry of Health.
Maspalomas Gay Pride is one of the prominent events on the gay community calendar and thousands of people from all over Spain and many European countries attend it every year —except during the forced break caused by the coronavirus pandemic. According to health sources, “among the thirty or so diagnosed in Madrid, there are several who attended the event, although it is not yet possible to know if one of them is patient zero of this outbreak or if they all got infected there.” Research has revealed that the virus began to circulate in the city during the second half of April, although most of the infections known so far occurred around the weekend of May 7 and 8.
Now Belgium:
Oganizers of a fetish festival in Belgium are warning attendees of possible exposure to monkeypox after public health officials linked three cases to the event that recently concluded in Antwerp….
Darklands is a four-day event catered toward gay men that includes a daytime festival, several nighttime parties, as well as education and shopping that features “an extraordinary selection for fetish retailers at the gear market,” according to its website. The festival concluded on May 9.
“There’s reason to assume that the virus has been brought in by visitors from abroad to the festival after recent cases in other countries,” festival organizers said in the post.<./p>
And Quebec, or rather, Montréal:
Dr. Réjean Thomas runs Clinique médicale l’Actuel, a clinic in Montreal’s gay village that specializes in caring for people with HIV and other sexually transmitted diseases.
He says he’s seen up to six patients with symptoms associated with monkeypox, such as lesions on their genitals, within the past two weeks….
“It [likely] started in the gay community in the U.K., and in the gay community people travelled — Portugal, Spain — and Montreal has a large gay community. Gay men like to come to Montreal.”
When asked about stigma on Friday, Dr. Theresa Tam, Canada’s chief public health officer, cautioned against associating the disease with any one group.
“Certainly we will provide support and information … but I think people should understand that [transmission is through] close contact and that could happen in different ways,” she said, pointing to cases in the U.K., two involving people who lived in the same household.
Hence CDC’s advisory:
However, a high index of suspicion for monkeypox is warranted when evaluating people with the characteristic rash, particularly for the following groups: men who report sexual contact with other men and who present with lesions in the genital/perianal area, people reporting a significant travel history in the month before illness onset or people reporting contact with people who have a similar rash or have received a diagnosis of suspected or confirmed monkeypox.
And WHO:
Reported cases thus far have no established travel links to an endemic area. Based on currently available information, cases have mainly but not exclusively been identified amongst men who have sex with men (MSM) seeking care in primary care and sexual health clinics.
However, there are going to be a lot of festivals and mass gatherings during this coming “Hot Pox Summer,” and with no agreed mode of transmission, little information on how prevalent community spread really is, and that really long incubation period, it would be foolish to focus too narrowly on “men who have sex with men” (think again of that example of airplane transmission). It would be super-nice if monkeypox didn’t end up being characterized as a “gay plague,” which would be a bad faith interpretation of what CDC and WHO wrote, but since that’s the stupidest possible outcome, no doubt it will happen.
What to Do?
One thing to do is something you may already have done: Gotten vaccinated for smallpox. From CDC:
Because monkeypox virus is closely related to the virus that causes smallpox, the smallpox vaccine can protect people from getting monkeypox. Past data from Africa suggests that the smallpox vaccine is at least 85% effective in preventing monkeypox.
However, we stopped routine vaccination for smallpox in 1972, so this only applies if you are an old codger like me. Still, you can get vaccinated for smallpox today:
Vaccines: We have a full stock of smallpox vaccines, thanks to bioterrorism preparation. Smallpox vaccines work on monkeypox, especially if the vaccine was recent. In fact, the CDC reports that smallpox vaccination within 3 years is 85% effective at preventing monkeypox disease. The sooner the person received the vaccine, the more effective it will be.
There is also treatment:
Treatment: Effective therapeutics have already been developed but not widely available. The antiviral ST-246 (tercovirimat), for example, was developed specifically for smallpox but works for all orthopoxviruses including monkeypox.
Finally, there are non-pharmaceutical interventions (NPIs):
Other mitigation measures: COVID-19 mitigation measures, like masks and improved ventilation and filtration, will help with reducing spread. In fact, in 2021, a monkeypox case landed in Dallas from Nigeria. It’s largely hypothesized that the mask mandate helped contain the virus.
For myself, I’m going take precautions and assume, for now, that monkeypox is airborne. I’ll continue my current Covid regimen: masking, avoiding crowds, staying in the open air when possible, and in well-ventilated spaces if not. I will also go back to what I did before we all understood aerosol transmission, and work to prevent fomite transmission: Lots of handwashing. Little touching of handles and elevator buttons. And no touching of lesions or scabs! (I don’t know if medicines like Betadine, zinc, IVM, and vitamins have any effect on monkeypox at all, so if they are part of my regimen, it won’t be because of monkeypox.) And for me, the question of festivals and mass gatherings does not arise; I don’t enjoy them. If I did, I would consider sacrificing them. Ditto air travel.
Conclusion
The whole monkeypox outbreak is more than a little unsettling. Bloomberg:
London (AP) — Scientists who have monitored numerous outbreaks of monkeypox in Africa say they are baffled by the disease’s recent spread in Europe and North America.
“I’m stunned by this. Every day I wake up and there are more countries infected,” said Oyewale Tomori, a virologist who formerly headed the Nigerian Academy of Science and who sits on several WHO advisory boards..
“This is not the kind of spread we’ve seen in West Africa, so there may be something new happening in the West,” he said.
One new thing that might be happening: Covid. In addition to Long Covid, vascular damage, and neurological damage, all of which are surely more prevalent than we think, our immune systems are probably out of whack at a population level, and monkeypox may be taking advantage.
Or perhaps the new thing is evolution at work:
The last case of natural smallpox was recorded in October, 1977. It took humanity almost 20 years to achieve that feat after the World Health Organization had approved the global smallpox eradication program. Vaccination against smallpox was abolished, and, during the past 40 years, the human population has managed to lose immunity not only to smallpox, but to other zoonotic orthopoxvirus infections as well. As a result, multiple outbreaks of orthopoxvirus infections in humans in several continents have been reported over the past decades. The threat of smallpox reemergence as a result of evolutionary transformations of these zoonotic orthopoxviruses exists.
Of course, we should be able to contain monkeypox:
Several outbreaks of monkey pox in Africa have been contained during the COVID pandemic while the world’s attention was elsewhere, and outbreaks in Europe and the United States are a concern, Africa’s top public health agency said on Thursday.
“During this pandemic, we have had several outbreaks of monkey pox on the continent … We also expect that other outbreaks will come and we’ll handle it in the usual way,” Ahmed Ogwell Ouma told a weekly news briefing./p>
“We are in close contact with our counterparts at the European CDC to try and understand where that did come from because when you see monkey pox in environments that are far away from a forested area then for sure as far as public health is concerned it raises a lot of questions.”
Then again, another new thing might be the destruction of the public health system under the Trump and Biden administrations. We were never able to do contact tracing with Covid, for example. Or mask mandates. Or quarantines. So it looks like we’re going to confront monkey pox with no settled theory of transmission, and vax + pharma once more. Perhaps doing the same thing will have a different result.
NOTES
[1] Interestingly, the mode of transmission for smallpox could be aerosols as well:


” Human infections with the West African clade appear to cause less severe disease compared to the Congo Basin clade, with a case fatality rate of 3.6% compared to 10.6% for the Congo Basin clade.
So far, we’ve detected only the Congo Basin clade (see above), which is good news. In practice, the death rate could be even lower…”
Did you mean so far only the West African clade has been detected?
Thanks, fixed. Dyslexia…
Sharing of bedding or clothing modes of transmission… I’ve read that before too.
I couldn’t work this in:
“However, there are going to be a lot of festivals and mass gatherings during this coming “Hot Pox Summer,” and with no agreed mode of transmission, little information on how prevalent community spread really is, and that really long incubation period, it would be foolish to focus too narrowly on “men who have sex with men” (think again of that example of airplane transmission). It would be super-nice if monkeypox didn’t end up being characterized as a “gay plague,” which would be a bad faith interpretation of what CDC and WHO wrote, but since that’s the stupidest possible outcome, no doubt it will happen.”
It begs the question why Africa never reported it as such nor do the references to its prevelence in Africa say anything about it being more common there in “men who have sex with men.”
Africa does not have responsibility for the Canary Islands. As a gay man, from my first routine checkup at a sexual health clinic in the 90s, “Spain” was treated as two distinct areas of concern – the mainland (same as rest of EU) and the Canary Islands (meaning predominantly Gran Canaria – Maspalomas Pride being a potential superspreader event).
African responsibility on reporting on various sexually transmitted diseases was poor to non-existent to “not in our jurisdiction” (Canary Islands). I am a hermit these days but I’ve heard nothing to suggest the Canary Islands is not still classed as a MUCH higher risk area than mainland Spain.
I thought about that. I also thought about the homophobia in Africa.
But I’ve also learned this from watching Covid: once these viruses cross over from animal to human and get widespread enough in humans, they can mutate fast.
And this is where the epidemiologists and physicians should walk down the corridor and talk to the health services researchers who look at sexual behaviour etc. They quickly in the 90s got wind of stuff I learnt anecdotally – stuff which I actually got confirmed since the STI consultant who typically checked me out started work part-time in a part-time academic position in my department and we would chat in consultations, with him giving me the “stats and low-down” on everything.
IF monkeypox turns out to be sexually transmitted easily then risk factors for this will show up quickly, if you know how to stratify your data. Separate out areas of almost purely M-M transmission (e.g. Sitges and Ibiza in Spain) from areas where you get a lot of closeted men who attend Pride etc and engage in unsafe sex whilst in a “straight” relationship (Gran Canaria is a hotbed for this, as are various areas of the South of France where naturism is common). Apologies for “lowering the tone” but it is crucial in understanding sexual transmission risk and lack of doing this caused a LOT of the epidemic in Africa of AIDS, as you acknowledge.
These days, with more sexual openness in the developed world, I’m less worried about the potential for this to be characterised as the next gay plague. I just want a possible mode of transmission understood ASAP since, as you acknowledge, it could get out of control in the wider population quickly if we underestimate it.
> Apologies for “lowering the tone” but it is crucial in understanding sexual transmission risk and lack of doing this caused a LOT of the epidemic in Africa of AIDS, as you acknowledge.
> These days, with more sexual openness in the developed world, I’m less worried about the potential for this to be characterised as the next gay plague. I just want a possible mode of transmission understood ASAP since, as you acknowledge, it could get out of control in the wider population quickly if we underestimate it.
Yes to both points, especially “I just want a possible mode of transmission.”
It seems impossible to me that even the horniest of horn dogs would want to, er, copulate with anybody whose lesions were visible. Yech!!!! And after AIDS, I would think you’d have to be pretty addicted to risky behavior to go with anyone who had a rash, particularly at a festival where one is, as it were, spoiled for choice.
IANAE (I Am Not An Epidemiologist), but that raises for me the unpleasant possibility that monkeypox has an asymptomatic mode of transmission. The plane incident raises the same possibility, though of course we don’t know what activities the passengers were engaged in. (On a brighter side, this perspective decouples gay events from “exchange of fluids,” which I think is the hidden assumption in both CDC and WHO’s alerts. That an assumption I want proved, not hidden. Presumably somebody is studying it [hollow laughter].
In Portugal it was reported by 2 practices (in Lisbon) that specialize in following people affected by AIDS HIV, sexual transmissible diseases, etc. So far, all (or almost all, I should check) patients are men below 42 (it probably fits with the vaccination of smallpox). They are very careful to say that maybe this specificity is more connected with the places where it was found than with the contagion route (as, until now, it has never been considered a sexually transmissible disease).
Not only that, but one might imagine that regular testing for disease is a priority for these communities. Their diligence in this regard might explain why many of the reported cases thus far have been from a community that tests for disease regularly.
Exactly.
Both you and IsabelPS make good points, thank you.
Thank you, Lambert.
Perhaps I am wrong to be as sanguine as I am, but this doesn’t ‘feel’ as scary to me as the CV news did, 2 years ago (and as it does — to me — still). Perhaps it’s that there aren’t (yet) reports of recovered and possibly reinfected people dropping dead in the streets, as there was from Wuhan … just 26 months ago (it feels like ‘long ago in a galaxy far, far away’).
Reverting to a. for me, more normal, and snarky outlook: I’m sure US will have no difficulty controlling the spread of Monkeypox, provided that the control/containment measures do not infringe individual liberty to go about life as normal. OTOH, if these early reports are harbingers of really bad news and highly quality respiratory protection is determined to be necessary and is, at last, widely adopted, it might help to control the CV. Perhaps that’s something to hope for.
What would a bunch of monkeypox cases set people’s immune system up for with Covid still out there?
It might work the other way ’round. Last year there were some publications (perhaps more since; haven’t looked) asserting that the CV could exhaust and derange T-cells, impairing immune response to other infections.
This by itself seems to me grounds to remain highly concerned about contracting CV.
(I have the impression that there is reason to think that the vaccines, particularly if received numerous times, also could induce similar effects)
Gee, I wonder, why would a plague (or something very like it) arrive just as the world is on the brink of signing a treaty that would give the WHO emergency powers? Bill G, whaddaya say? Are we forked, or what?
The “Gay Pride” association is often thought to be a result of the higher risk taking behaviours of many gay men. Considering some of the wacky things I saw at Southern Decadence Festival one year, the slur might have some basis in reality.
Anyway, I’m wondering if New Orleans will be experiencing an outbreak of the Monkeypox soon. It caters to just the sort of jet setting, sexually adventureous population that this pathogen would find itself at home in. What is worrying is the fact that it has already exhibited the signs of community spread. Now there is a resivoir of the virus within several large populations of Terran humans. Phyl and I were both vaccinated against small pox when we were children. Almost everyone was. The new generations were not so vaccinated.
Absurdity in action. One pathogen where a vaccine is near useless, and said vaccine is pushed ruthlessly. Another disease where there is already a useful vaccine available, and nothing.
“They” really are trying to kill us.
There is a realtionship between population density and infectuous disease. The higher one goes, the other follows. In this regard, I’m with Mr. Flynn above. It might soon be the “Hermit Life” for us.
Regarding the rate at which monkeypox could be changing: I’m already noting a lot of ‘expert’ bloviation on monkeypox repeats logical errors that made so many expert predictions about Covid evolution literally fallacious.
‘It mutates slowly.’ is back.I know I’ve harped about this before, but:
1) The rate at which researchers detect mutations needn’t be the rate at which mutations occur, and
2) Neither of these necessarily constrains the speed with which the disease’s behavior will change when it enters a new popuation.
Here’s Professor Stefan Rothenburg of UC Davis, who studies orhopoxvirus/host interactions:
The thread I quoted that from:
https://twitter.com/RothenburgLab/status/1528108562894901249
And a relevant article from 2014:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3945082/
Note: The “low frequency SNP’s” Rothenburg refers to are Single-Nucleotide Polymorphisms. I think an article on the topic featured in Links recently. Their relevance here is that a great deal of the functional variation in the monkeypox virus population is likely due to combinations of possibly trivial-seeming and not very common gene variants, which may not even have been observed. Mutation need not occur for them to come into play.
So, people looking at the genomic sequencing results coming in from the current outbreak and drawing inferences about the nature of the bug that’s circulating are knuckleheads.
> So, people looking at the genomic sequencing results coming in from the current outbreak and drawing inferences about the nature of the bug that’s circulating are knuckleheads.
I don’t see why. They’re taking snapshots of a virus that’s evolving and adapting, like everything else.
They’re knuckleheads for not realizing that they don’t necessarily know what to look for, and that the snapshots may not even show what’s important. They’re double-damned and worse than knuckleheads if they’re in a position to know these things and prognosticate anyway.
When I say that Covid predictions were literally fallacious, I don’t mean that they proved incorrect, I mean that their logic was completely unsound.
The current state of understanding of monkeypox is such that virus now circulating outside of Africa could lie comfortably within one or the other of the known clades and have function wildly different from what’s expected from either of them. The fact is, we’re seeing unexpected behavior. In and of itself this means that any observed genetic similarities to ‘known’ monkeypox virus aren’t in and of themsevles predictive of similar behavior.
Until the various references to gay men in the pieces that have been coming out, sexual transmission or a new mutation/adaptation(?) of the disease hadn’t even occurred to me. Instead my first thought was ‘t-cell derangement’ in people with multiple covid infections, people going out and trying to live their life thinking covid was no big deal and their immune systems being unable to resolve something that, maybe prior, would have been no big deal.
I’ve had covid once so far (that I know about) and had a wild reaction afterwards that isn’t supposed to happen (my hair growth since is showing banding of different colors, like a tabby cat) in people but I am convinced is a symptom/side effect of the covid t-cell impact, like my body’s ability to fight melanomas might be compromised right now. How fragile could someone be who has had covid multiple times?
> my hair growth since is showing banding of different colors, like a tabby cat
Holy moley!
yeah, I had a bunch of weird symptoms in the month after covid that seemed like something called VKH and there have been other cases of it after covid. I’ve mentioned the weird hair loss here before and how that is a known covid thing too. But the specific two symptoms that drove me to the doctor were an absolutely terrifying 4 day headache that felt like intracranial pressure and finding a white spot in my hair after my hair dye stopped working in that spot (hair dye needed hair follicles with pigment, no pigment in a big spot). But the doctors thought it was not actually VKH, and so far I’ve been on wait and see protocol. They did find a few minor skin growths and removed them.
A couple of months after that, about an inch an a half of growth has come in. The hair that fell out is all coming in white (I have black hair with a red tint). The spot is white and black with stripes on the hair follicle like agouti in mammals. I’m not a scientist so I quit obsessively reading papers after it seemed like I wasn’t going to die but it made sense to me to keep a close eye on stuff involving melanin production (skin esp) for a while in case my body was adapting to the hit to my immune system by nuking melanocytes.
I’ll keep the commentariat updated on my hair journey, lol
“When asked about stigma on Friday, Dr. Theresa Tam, Canada’s chief public health officer, cautioned against associating the disease with any one group.”
***********
Really? Then why is it OK for the CDN Government and its leader Prime Injector Trudeau to spew bile and hatred, segregate and discriminate against those who do not want to be injected by Criminal Organizations.?
“And through it all, you’ve attracted a level of public scorn that in normal times would typically be reserved only for terrorists and violent criminals. Prime Minister Justin Trudeau called you a “racist” and “misogynist” in a September TV interview. Quebec Premier François Legault called you a “burden” on the health system deserving of punishment. National op-eds are calling for you to be turned away at the hospital’s front doors if you get sick.”
https://nationalpost.com/news/canada/punishing-the-unvaccinated-has-become-one-of-the-most-popular-positions-in-country
Time for those who profess a belief in human rights to step up and show their true colors.
Rodents, not monkeys, are the principal animal reservoir for the disease, and pet importation probably accounted for a previous outbreak in areas where the virus has previously not been present. From the CDC:
“2003 Outbreak from Imported Mammals
In 2003, forty-seven confirmed and probable cases external of monkeypox were reported from six states—Illinois, Indiana, Kansas, Missouri, Ohio, and Wisconsin. All people infected with monkeypox in this outbreak became ill after having contact with pet prairie dogs. The pets were infected after being housed near imported small mammals from Ghana. This was the first time that human monkeypox was reported outside of Africa.
What caused the 2003 U.S. outbreak?
Investigators determined that a shipment of animals from Ghana, imported to Texas in April 2003, introduced monkeypox virus into the United States. The shipment contained approximately 800 small mammals representing nine different species, including six types of rodents…”
Thank you Lee, good link. This looks like a significant vector, where rodent-to-rodent transmission can progress between species when territories overlap, or where humans could also act as transmission agents without necessarily acquiring an infection themselves, as when a tender of rodent stock might use the same tool to clean several cages without sanitizing it in between.
Incubation rates – probably faster in rodents than in humans but still likely a matter of days – impede passive detection more than transmission.
I’ve so far not found data on fomite duration, I think we need to know more about that. Rodents can be / have historically been disease vectors in food storage and preparation contexts. US food preparation standards have increased significantly over my lifetime (64y), spurred by SARS-1 and Ebola experiences, and insurer’s responses. So relatively minor enhancements of standards already in place could produce better prophylactic effect.
If monkeypox had begun broad/international circulation in 2020 around the same time as SARS-CoV-2, it could have been very ugly:
https://www.newsweek.com/rats-rodents-increase-cdc-coronavirus-1506147
Also, if food can be a vector, transmission jumping across further animal species, especially but not only domestic pets, bears examination and vigilance.
Currently poking through the references in this October 2019 article (PLOS = Public Library of Open Science):
A systematic review of the epidemiology of human monkeypox outbreaks and implications for outbreak strategy
https://journals.plos.org/plosntds/article?id=10.1371/journal.pntd.0007791
Who was importing these animals? And was there any good reason for it?
They were for the pet market.
Monkeypox confirmed in imported African rodents CIDRAP (2003)
“Jul 2, 2003 (CIDRAP News) – The Centers for Disease Control and Prevention (CDC) said today it has confirmed monkeypox in six rodents from a shipment of African mammals that is believed to be the source of the current monkeypox outbreak in the United States.
Monkeypox was confirmed in one Gambian giant rat, three dormice, and two rope squirrels, the CDC announced. The animals were part of a shipment of African rodents, previously numbered at about 800, imported into the United States on Apr 9. The CDC did not say whether the six infected rodents were the only ones recovered from the shipment or if any other animals from the shipment were tested and found to be free of monkeypox…”
What Happens To A Rock Climbing Community When Venture Capital Comes Calling?
Another venture capital v private equity saga, BUT! I thoroughly enjoyed the story of Memphis Rocks. That was uplifting, reminding me I’m not a complete cynic.
>>>Time for those who profess a belief in human rights to step up and show their true colors.
Which is hard(er) to do when doing so gets you accusations of being a terrorist or racist or just evil as it not only threatens your well being, it turns off the brains of those around you. It is like when some people become convinced that public health is the evuhl communism in some parts of the United States or is merely something on “a menu of options” to take of yourself according to the PMC people.
It is looking like it will be a double header this summer. Just in time for the Summer semester and then into the Fall. Fun.
When the CDC advice is ‘You can recognize potential monkeypox infection based on the similarity of its clinical course to that of ordinary discrete smallpox’ I can only assume that that is meant for medical staff. But realistically, I suspect that most medical staff would be only familiar with smallpox through reading about the history of medicine as it was eradicated about forty years ago. So how many doctors and nurses would know what to look for then?
Ha, that was my thought too. I think doctors and nurses would have a pretty good idea because I assume they all learn about smallpox at some point, and they would do it with visual aids as I believe they do with a lot of their study? (pictures in textbooks, lecture powerpoint slides etc.), I mean visual documentation of smallpox is pretty extensive, I think? Particularly with the advent of photography. Not to mention the manner in which the disease presented is pretty notorious
Not very practical advice for non-HCWs though, but I guess it wasn’t necessarily meant to be
in my few experiences with rashes and things, and going to regular doctors (as gatekeepers for dermatologists) and then eventually passed on to dermatologists when those doctors reach the limits of their ability, a rash is a rash is a rash to most of these people. yes, they understand things like blisters, pustules, and are definitely keeping their eyeballs open for melanomas or parasites but other than that, there are thousands of things they haven’t seen in person and the particular way they develop on an individual’s skin type can skew diagnosis.
during one of these events, one diagnosed me with impetigo and the next said “impetigo doesn’t happen anywhere except developing nations” and they were both looking at the same rash. thank goodness we have the international agencies alerting health care workers about this, because they may just think it’s a typical domestic “pox” due to bias of “monkeypox doesn’t happen here”. granted, the prescreening session would have already asked about exotic travel, one would guess.
so i’m hoping that we have better ways of detecting this thing than just looking at your booboos, because i’ve been misdiagnosed multiple times that way. luckily for nothing more severe than what was probably some kind of eczema, although they never did figure out what that somewhat disfiguring rash was on either side of my nose before it had gone (8 months suffering with that and various prescribed creams which did nothing).
oh, and doctors are not going to want to inspect these kinds of booboos anyway. my experience when i had chicken pox as an adult and was forced to get a doctor’s note to satisfy my boss that it wasn’t simply a desire for an unpaid 3 week vacation out of the blue (when i could barely afford to live working all of my available and scheduled hours, and she well knew that) was that the doctors don’t want you coming in with something like that, lest you contaminate their facilities or other patients. and some health care workers get very freaked out and try to keep their distance as well. i had one that checked me into an examination room that was keeping a 10 foot distance, and then told me from the doorway “i’m going to leave you here because i get shingles at the drop of a hat!” this was after strategically scheduling me so that there would be almost no one else in the building at the end of the day.
>>>and was forced to get a doctor’s note to satisfy my boss that it wasn’t simply a desire for an unpaid 3 week vacation
Honestly, some employers are morons. Just how is it safe or profitable to have a mass infection of something like chickenpox? But we are seeing the same stupidity with Covid. A disease is a disease. It does not care about politics or anything else. It lets purpose is to spread and reproduce and if you die, it does not matter. Nobody has a magic disease shield.
I know that I keep whining about the stupidity of the people over the pandemic(s) but really just how hard is this to understand? Would you argue about walking up to the hungry grizzly? Or playing with the rattlesnake? Or letting one into your home?
Thank you for this post Lambert.
I am wondering whether the virus was introduced in the Canary Islands by migration, by tourism or both. Then the mass party acted as superspreading event. Now that the community has been alerted I expect that many of the cases will be end-point and R will be lower. Being this a disease that apparently requires close contact behaviour is the most important factor in R. My guess is this will not become endemic but there is the possibility that hidden transmission was much higher than what we know so far and it can have reached a wider geographical distribution and we are yet to discover.
The bad thing, that makes it a little be harder to track, is the relatively long incubation period so I believe that we will see many more cases here and there.
Hey Jankowicz! This is it. This is your moment, your time to shine and heed your true calling!
Get out there and sing us some clever little Monkey Pox song!
Thanks Lambert. I had heard a while ago (years) that monkeypox had a high fatality rate. Something closer to 30%. So this is almost a relief. Don’t know if anyone remembers Fukushima fallout, but in 2011, I talked to a med tech about the follow-on effects of that blowout and he said that there was an apprehension that Fukushima radiation all around the world (it was a mega disaster that simply was not discussed) would “change epidemiology.” I took that to mean that there would be more epidemics, etc. The same thing has been said about a warming planet – that a warmer planet is more virulent, etc. So not only do we have the lasting effects of immune suppression in long Covid, we have a worsening planet-environment – and way too much human interaction. imo.
I get the connection between human interaction and the spread of diseases, but I also see how the lack of human interaction and therefore of human connections can kill us just as much; mental illness, addiction, bad thinking (reasoning ability), violence, and murder including mass shootings are all getting worse as we are steadily atomized; if the current system whatever it is wanted to maintain its ability to exploit the general population, it would be completely, but profitably, incompetent with the current pandemic(s); this would be a good tactic for the strategy of creating opportunities to maintain the current disaster capitalism.
MedCram – Medical Lectures Explained CLEARLY 1.39M subscribers – Monkeypox Explained Clearly
The video give more coverage on both the types of vaccine available and risks / benefits of each, and also a number of support medications and procedures for patients post-innoculation/infection.
Great job Lambert. Everyone should read this in-dpth article by Whitney Webb: https://www.citizensjournal.us/monkeypox-fears-may-rescue-endangered-corporations-aiding-public-in-forgetting-their-past-sins/
In it, she shows the relationship of the company Emergent Biosolutions who have recently purchased the rights to the smallpox vaccine known as ACAM2000, which can also be used to treat monkeypox. The company has a horrible record with their Anthrax vaccine and their production of Covid 19 vaccines and have just announced they will acquire the exclusive worldwide rights to the “first FDA-approved Smallpox Oral Antiviral for all ages” from the company Chimerix. The drug, called TEMBEXA, is only for the treatment of smallpox, which the company refers to as “a high priority public health threat.” The press release on the company’s acquisition of TEMBEXA states that multi-million US government contracts for the product are anticipated.
Emergent Biosolutions now has a monopoly on smallpox and monkeypox vaccines. The Webb article has much more information but it’s starting to sound like a song we’ve heard before.
PS, another interesting article: Monkeypox Was a Table-Top Simulation Only Last Year can be found at: https://brownstone.org/articles/monkeypox-was-a-table-top-simulation-only-last-year/
From the article: Elite media outlets around the world are on red alert over the world’s first-ever global outbreak of Monkeypox — just one year after an international biosecurity conference in Munich held a simulation of a “global pandemic involving an unusual strain of Monkeypox” beginning in mid-May 2022.
So you’re saying the elite biosecurity people were doing their jobs? ffs
Also, please don’t pollute the comments section with toxic waste from those GBD goons at Brownstone. Thank you.