Yves here. The idea that more and more economic activity is likely to be devoted to “care work,” such as services to the young and aged, is typically treated as a negative outcome. The authors of this post beg to differ.
By C.P. Chandrasekhar, Professor of Economics, Jawaharlal Nehru University, New Delhi and Jayati Ghosh, Professor of Economics and Chairperson at the Centre for Economic Studies and Planning, Jawaharlal Nehru University, New Delhi. Originally published at Business Line
Across the world there is much gloom and doom about the impact of technological changes on jobs, as automation and other innovations are seen to threaten not just blue-collar jobs but also many forms of office work. It is true that the way that most of our economies are organised at present, heavily reliant on market mechanisms with less and less public intervention to alleviate the adverse effects, there could well be an increase in technology- driven unemployment.
But even so, some of the extreme pessimism may be misplaced because of the possible emergence of other forms of employment that are more based on human interaction. Particularly, some essential services that enhance the quality of life – which are often broadly clubbed into the composite term “the care economy” – are unlikely to be either as efficient or as socially useful if the element of human interaction is reduced.
Many care services necessarily require face to face relationships, and even if technologies can assist in these and make them more productive, the human element cannot be eliminated. Indeed, better quality care (whether in paid or unpaid forms) typically requires more intensive human input, so standard approaches based on puerile notions of labour productivity are simply irrelevant in such activities.
This in turn means that the care economy broadly defined will continue to be an important source of employment generation in the foreseeable future, and is likely to expand at a faster rate than many other economic activities. This is especially so in the many countries – certainly across the developing world – where care services are currently hugely underprovided by society and therefore forced to be delivered (often in extremely difficult and haphazard ways) by unpaid family labour.
How can we even begin to estimate the likely future global demand for care activities, which include care of the old, the young, the sick, the differently abled, as well as the healthy adults who have different kinds of care needs including all the aspects of quotidian life? This is a huge area of work, made more complicated by the fact that so much care work is performed within homes and communities in often socially unrecognised ways.
But it is possible to provide some initial estimates, based on current employment in care activities in societies where these are more developed and known to be better delivered. Suppose we take Sweden as the benchmark on the basis of which to estimate likely care requirements in the future, since Sweden is known to have a well-functioning (and largely public) health system and is also known to provide reasonable levels of child care and elderly care. Employment in care activities in Sweden relative to the target populations can provide an indicator of the desirable levels of employment. Of course, this is likely to be both optimistic (since most countries currently lag well behind Sweden in such provision) and an underestimate (since much of the employment involved in the provision of such care would not be captured by the occupational classifications alone). So this is clearly an imperfect measure, but nevertheless it provides some broad indications of the potential demand for care.
Here, the Statistical Database of Sweden is used to identify the number of workers in certain care activities in 2014, and compared with the UN population projections for Sweden for 2015. The category of “health workers” includes health care managers, doctors, nurses, physiotherapists, psychologist and psychotherapists, other health care therapists and complementary medicine therapists, dentists and dental nurses and other health care assistants. These occupations together amounted to 762,806 workers in Sweden in 2014, which (given the estimated population of 9,779,426 in 2015) means an average of one such worker for every 12.82 persons.
Now apply this norm to the UN population projections for 2030 for all countries, on the assumption that this is the desirable norm for other countries to try to achieve by 2030 (and is not unreasonable given the Sustainable Development Goals). This gives estimates of the likely requirement of health workers in different regions and in the world as a whole in 2030, which can be compared to the projected working age population (assumed to be 15-59 years) in that year.
A similar exercise can be carried out for dedicated child care and dedicated elderly care. For child care, the following occupations are used for Sweden: pre-school managers, primary and pre-school teachers, and childcare workers and teachers’ aides. When compared with the number of children in the 0-14 age group, this yields a norm of 3.6 children per worker. For the elderly, defined as 60+ years, the occupations taken are elderly care managers and
attendants, personal assistants and related workers. Obviously the elderly are also much more likely to require the assistance of health workers, but this is subsumed under the demand for health workers from the general population. This calculation yields a norm of 16.24 elderly people per worker. This may seem a large number, but it is likely that many people in the 60-70 age range are unlikely to require much assistance. (We do no attempt to measure the care requirements of the differently abled, which would significantly add to the estimates.)
Table 1 provides the results of this exercise in terms of the likely requirement of some categories of care workers using this norm. Several striking features emerge from this. First, if reasonably adequate care services are to be provided to people across the world in 2030, this will require a massive increase in care employment, even in the very limited occupational categories mentioned above. Second, in most countries and regions, this is likely to be a significant proportion of the working age population – and therefore an even larger proportion of the actual employed population. Third, in terms of providing such services to a reasonable level, many more workers will be required in related activities as part of the support and administrative systems to deliver these services.
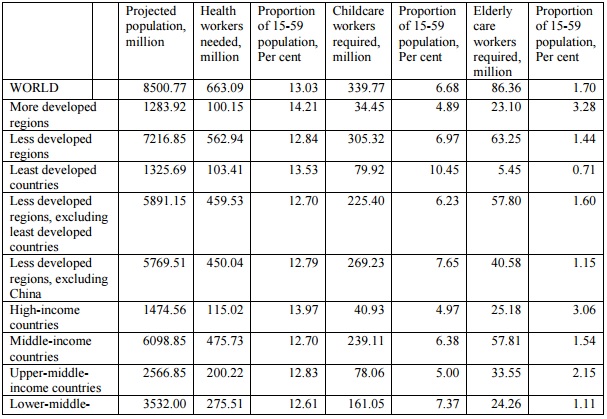
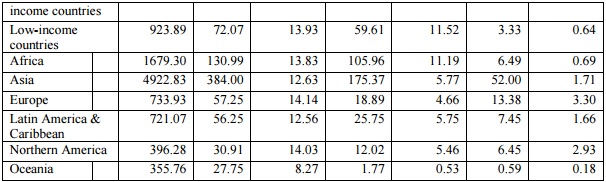
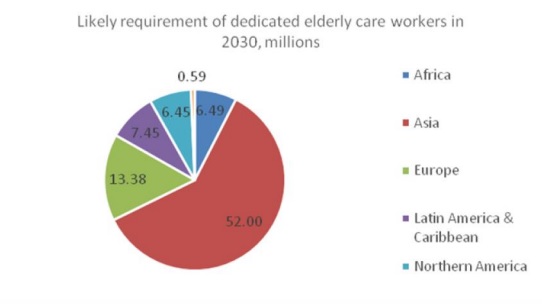
Charts 1, 2 and 3 describe the estimated requirement in terms of the likely regional spread of this type of occupation in 2030. It is evident that Asia dominates in the requirement, simply because of its large population – but what is surprising is that, despite the current perceptions of a younger population than in other regions, the requirement in terms of elderly care is also going to be very large, amounting to well over half the total requirement in 2030.
This basic and even simplistic exercise still provides some idea of the potential of the care economy to generate jobs in the future. But this will NOT be delivered by market forces on their own, and nor will such jobs be “decent work” if the market alone is to determine this. The need for state intervention – and for public provision of these essential care services – is therefore paramount.
Chart 1
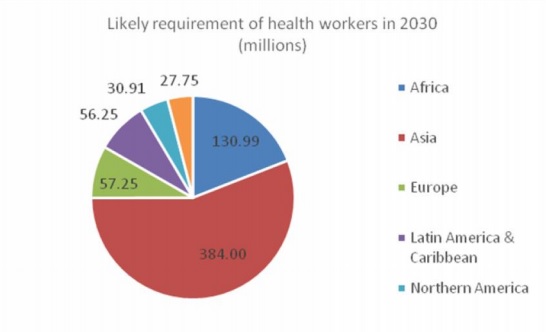
Chart 2
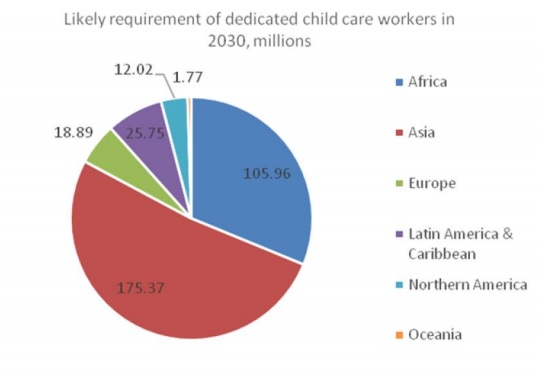
Chart 3


Well, both Hill and Donald seem to anticipate that this is the only place jobs are—they both are advocating big child care programs. Two birds with one stone: taking care of kids for working mothers, and creating new jobs for single mothers, who can then put their kids in the child care. Maybe if they’re lucky their kids will be at the same child care place they’re working at.
What’s wrong with this picture?
i did just that under Bill…started at the bottom (cafeteria) at a Montessori school bc i couldn’t afford the tuition for my daughter. i knew it to be a good school and they underlined that when they paid me the going rate plus accepted my child. the school even forgave my tuition to qualify for teaching assistant…a large expense. unfortunately, after 5yrs the school changed hands and no longer accepted my child without a large fee. the new owners fired All TA’s. i cleaned houses and provided in-home care for cancer patients until i located a montessori school not too watered down. (btw, no training in cancer care…today im caring for 2 people with cancer and still swinging in the wind).
the problem with in-home care is within state structures…some states don’t even recognize (no pay) the care. also, the qualifications are scattered and very costly. i looked into hospice certification here in Ga and the avg cost is over 5000.00. my state is in the process of privatizing this particular industry care. the nurses i speak with are in a flux between no work and semi-work…someone dying and the family involved takes a total commitment on the part of the caretaker. many patients and family’s are cash strapped…caretakers paying expenses out of pocket only last so long.
maybe this is why corporations allowed the privatization of prisons to fall to the wayside…they know where the next BIG fix is. guaranteed windfall bc we will die and some of us expensively thanks to the very toxic environment.
Perhaps no pressure on business to require part-time job options that are as good as full-time job options (except with a corresponding reduction in pay) to enable more parents to work part-time and not make the choice between stay at home parent and full time work? Some countries already do do this. Of course that probably wouldn’t work with employer provided health care of course and of course maternity leave is also needed. And of course that would only work financially for some.
What is your solution to the fact that women have always been caretakers and yet not having continuous work experience in this economy jeopardizes their survival (the man to support a woman theory works up until the day he files divorce). We all know some countries offer 2 years of parental leave.
There seems to be an inherent problem, in American society anyway, that caring for people is often considered a weakness, and thus, if you agree to work at something where you are primarily helping others, that makes you some kind of a loser. Clearly you must be desperate or addled. I’d also add that immigrants are another group, besides women, who often hold these jobs. We’ve got a fundamental problem when money rewards sociopathic values and undermines empathy and kindness.
Yes immigrants but even then they are immigrant women holding those jobs mostly, so it is a woman thing. What do immigrant men do? Gardening, construction, day labor, I don’t know what else.
Male caregivers often work in nursing homes and in hospitals. And I’m sure there’s some gender bias against them for doing this kind of “weak” work. But there they are.
Dr. Neva Goodwin at Tufts has a well developed (working paper) on care work being the foundation for economically viable UBI scheme. She has presented this work with the Democracy Collaborative and Next Systems work. Please see here
Core Support for the New Economy [Draft working paper] June 2016
Thanks for the link. Goodwin has the larger point just right. It is idiotic to force people into crappy paid work in order to pay other people to care for their children and elders. The authors of the post make good points about how much paid care work is created in modern societies, but it still misses the bigger point that there in no intrinsic difference between paid and unpaid care work.
As to Yves’ intro, I think there are a few reasons why having more economic activity dedicated to care work is typically viewed as a negative:
1. Power dynamics. Since the pay in these sectors is generally miserable, what we often have (especially in the case of healthcare and eldery care) is those who have the resources to afford such care paying boatloads of money which gets slurped up by a rentier middleman and those doing the actual dirty work of providing the care getting paid peanuts. Getting paid below a living wage to clean up after a rich(er) person isn’t a good look.
2. Adminisrative bloat. What the article doesn’t address is how many workers who would otherwise be doing something productive in a normal economy are diverted into jawbs in what are billed as the healthcare and education industries, but which are really insurance and administration industries (rentiers). The stats in the article do not include these workers, but I assume this is a huge part of the animosity toward the growth of “care work”.
3. I don’t live in Sweden. It’s great to have models to follow, but it is very inflammatory to argue (as the article does not) that we should be moving to a post-industrial service economy when our infrastructure is falling apart around us and there is a glaring gap in public transportation. And this doesn’t just hold true where I live, but also in “industrialised” countries like the US and UK. Again, this animus is mainly just against what are classified as service jobs in general and not against actual patient/student interface jobs.
4. The pay is the opposite of what it should be. The hardest, most time consuming jobs, like parenting a special needs child, aren’t even paid at all. Interns at third age homes make far below living wage. If the administrator wage vs. dirty work wage was reversed, I’m sure there would be much less resistance to this idea (H/T Diptherio)
I’m not sure all the increased pay in the world is going to make caring for an Alzheimer’s patient good work (caring for children even if not one’s own, while stressful, is probably not comparable and may have some rewards). I suppose minimal hours with an Alzheimer’s patient and good pay might make it more tolerable, that recovery time is probably truly needed from that job. Caretakers themselves die sooner.
reality check.
i run a business of this sort. It can only afford minimum wages.
it pays minimum wages. most of my customers are govt subsidized. The govt has not raised its payments for the last ten years, and the number of compliance items increases monthly. Employee burn is high and quality keeps falling (you get what you pay for). There is no place to even open the conversation about rates with the govt.
the problem with the modern economy is the natural (and no so natural) monopolies and pricing power it creates. Once money is pure fiction, those who can create the money (and its credit equivalents) have an unfair advantage. The FIRE sector does this and circulates the money in itself, and causes inflation for everyone else which leads to decline of other’s standard of living. The defense and healthcare sectors are US specific distortions, but govt employees are now spoiled everywhere.
The problems created by the money system kept getting closer and closer to the heart of the system (equities to debt to GSE debt), and now are are the heart, the negative rates for the govt debt. What happens from here, i don’t know (but good cannot come from evil, this is fundamental) , and it is a thankless job trying to predict the incompetence and dishonesty that govt officials and their handlers like Soros are capable of.
One thing i have seen repeatedly with govt officials and departments is that they are experts are converting their problems into your problems. So beware.
A couple of questions: how would the texture of your business change if as a society we got together and decided to make senior care and child care a greater priority than, say, lighting Syraqistan on fire and subsidising wall street fraud? How would your valid complaints change if exorbitant healthcare costs were brought down to earth? How would your bottom line change if the subsidies to eldercare and childcare were on a par with the subsidies currently paid to Boeing? At that point would you be more willing to be paid on an equal footing with your workers whom you can now only pay minimum wage, with both of you receiving a decent living wage?
Somehow I kept thinking of the “smaller government” we’ve all been voting for these last few decades…..
I have a family member who provides assisted-living to four clients in his home. They much prefer staying with Lee to moving into an institutional facility, and he charges about $2000/mo less than the local corporate options…so about $3000/mo.
I’ve got an idea for an eco-village type set up where (for instance) 1/3 of the residents are old folks who’d otherwise be in assisted living/nursing homes, 1/3 would be caregivers, being paid to take care of their neighbors. The other 1/3 would take care of the greenhouses, goats, children, etc. or work outside the community. The idea would be to finance much of the place off of the care work, by charging those with the means $3,000/mo and those without (i.e. dependent on Medicaid/Medicare) whatever works for them. So, a sliding scale so as not to lock people out on the basis of ability to pay.
Having worked in a nursing home, I can tell everyone here that they are not good places…for anyone involved. We need better options, not because of ideology, because I don’t want to end up in one of those facilities and I don’t want any of you to either. We need to be organizing ourselves, right now, to provide for ourselves. Waiting around for the gov’t to figure it out is always a losing proposition.
That’s the truth. Nursing homes are last resort, in my book. I used to deliver specialty beds,( KCI), to quite a few for decubitus patients. The alzheimer’s wings of the facilities are pretty rough.
We need to bring back to the forefront the argument of end of life choices.
If the above is true, then it will also be fought tooth and nail by the owners.
Loss of consumer’s/patients by their own choice cannot be tolerated, bottom line and all that.
To me, that part of Soylent Green they got right. I’d rather check in to an end of life facility, not a nursing home.
what the Koch Brothers go state by state and Veterans are the key: https://www.yahoo.com/news/afge-inside-koch-brothers-plot-sell-veterans-health-220800490.html
This is where the argument breaks down for me. It assumes that the world economic growth will continue so that we will live in a rich enough of a world. It also assumes that the elderly are somehow able to extract large amounts of real resources from the young, who are already burdened with debt and terrible career and economic prospects. They are unlikely to welcome this extraction.
Meanwhile the 0.01% have no difficulty extracting large amounts of real resources from everyone else, which is why everyone else is burdened with debt and terrible career and economic prospects.
Where does this kind of work paradigm leave the antisocial assholes among us? Not everyone is an extrovert who loves people. This seems a rather bad thing…
funnee…i don’t like raving family members and constantly lookout for wayward siblings stealing drugs, money or legal papers to BLAME ME later. i can take the ‘thankless’ part of the job but landing in prison is a very serious FEAR of mine. i recently read about a local bonded caregiver losing everything to one family member accusations…kill me.
last week my own brother accused me of stealing his truck…he’d left it in a parking lot at the drugstore. he shouldn’t be driving but he sneaked out and caught a ride from the pharmacist daughter (gawd). the safety nets for cancer care are deteriorating fast. his new trial treatments are done in a doctors office and he’s immediately released…sometimes family members can’t get to him fast enough (spread thin with many ailing at the same time).
your going to have to think outside the box like the rest of us…this article reads like its an opening field to better lives. Health is mandatory and without money flow its bootstrapping time. it won’t be pretty…
don’t think that are that many un-social jobs to begin with, those jobs there truly were for introverts have been replaced by H1Bs and the like. Really it’s not a good economy to find an introverted job in as is. Maybe a few might still exist in government work?
So a “caring economy”, by apparently seeking to commodify care, does exactly what for whom outside of the number parasite class?
Well, we’d better make some meaningful work for people who f’ing hate people, lest they go kicking over the “in” kids’ sand castles. If it weren’t for the Western civilizational tenet that the imaginary is more real than what’s in front of you ever will be, we wouldn’t have the problem in the first place.
if a caring economy means people already doing paid caretaking work get better paid it does a lot for them. If it means nursing homes and so on are better staffed it means a lot in terms of patient care. If a caring economy means those doing unpaid care taking work getting as income (at least for a set period of time) then it enables people who are currently risking their own financial survival to care for others to have better lives (whether they risk their own financial survival of course depends, we all know well-off stay at home parents, but many who take on the caretaking role are none so fortunate).
Sounds like the resemblance between “the caring economy” and the “sharing economy” isn’t just that they rhyme.
Regarding care work today, it’s something in which only the rich can indulge.
Many times private duty nursing becomes confused with being in service at Downton Abbey.
http://www.nytimes.com/2011/03/29/nyregion/29butler.html?_r=0
Funny you should say that… just found out that a friend – who used to have a successful computer-making business in the 1990s, a good IT guy – just found work as a cook to the whole-foods-ceo-wife’s-parents… at decent pay …. so dig up that millionaire in your rolodex
Care jobs are okay but they don’t bring much value to the economy.
People need to get back to work and help build the country bottom up.
We need infrastructure, the roads, the tracks, the buildings, the pipes, the power and water networks that were constructed by our grandparents need dire refurbishing or more.
It’s not going to be a makeup job.
And it requires real people with hands to get the job done.
The future is not pussy footing around making tea for some elderly, but rather picking up a wrench, sledgehammer, … and getting down to work.
Ah the patriarchy. Caretaking jobs are necessary for the survival of the entire society (whether they are paid or not) but “they don’t bring value” they aren’t done by “real people” (they are usually done by women afterall not actually real people kwim) and they “consist of making tea for the elderly”. I don’t think anyone is saying caretaking jobs should be the ONLY jobs. But basically absolutely socially essential jobs are unpaid or poorly paid and women who often take these jobs earn pennies on the dollar and often end up eating cat food in their old age (single women are quite likely to end up poor when they are elderly).
Care jobs are okay but they don’t bring much value to the economy.
That is exactly the problem. They bring huge value to the society but not to the “economy.” I would argue that is the fault of the economy, not the work.
It’s henotheistic neoliberalism: thou shalt have no other economies before me.
Household, social, etc. economies exist, with their own forms of (often abstract, uncountable) currency. To symbol manipulators and bleeding-heart Randians, that’s a Problem. The only reason to monetize these other economies is to rhetorically trade off the common interest (which commoners don’t deserve) in favor of the elite interest (which elites do, because they’ll hurt you if you don’t).
They bring enormous value to the collective, non-commodified economy of the household, of which the capitalist economy is a subset, and a dependent one at that.
Thanks for posting this Yves! In fact, Chandrasekhar and Ghosh hit the nail squarely on the head.
“This basic and even simplistic exercise still provides some idea of the potential of the care economy to generate jobs in the future. But this will NOT be delivered by market forces on their own, and nor will such jobs be “decent work” if the market alone is to determine this. The need for state intervention – and for public provision of these essential care services – is therefore paramount.”
The expansion of care work should be one of the main draws (i.e. the thing to politicize) of a job-guarantee program or any other major fiscal expansion in the United States. Not only would it provide meaningful employment, put upward pressure on wages, and add a heavy dose of socialization to an increasingly isolated society, the bigger draw for me is that it is great for the environment!
Other than driving, care work has an incredibly small carbon footprint. And there is so much need. Speaking from personal experience (father and father-in-law had strokes in the same year), consider all the annual stroke victims who have horrible insurance plans that cover only 5-7 days of physical and occupational therapy. That’s it and then they are cut off, alone to fend for themselves, now disabled. These American citizens deserve more. Soaking up all the slack in labor markets and assigning them work duties to improve the lives of stroke victims would be a major boost to the economy and to society.
This is the type of creative thinking and vision that was sorely needed when Obama took office in 2008. I heard Christina Romer speak once and she did not strike me as all that imaginative in this way. However, I’m optimistic there will be opportunities in the future to advance the type of labor program that Chandrasekhar and Ghosh endorse in this article.
sounds like the downton abbey economy to me…hey we could be house staff and butlers, too!
I can see the ad now “non smoking, non drinking, mild personality required for live in care for aging mother. Flexible availability necessary as you will be working 8am-5pm and on call 5pm to 8am. Must be willing to perform household chores when mother is sleeping. Must have own car with insurance to drive mother to doctor. Proven ability to deal with difficult personalities required. Salaried position.”
tegnost looks up from bottom of hole, mutters “Damn, I though it was deep enough…”
gets back to digging
Funny you should say that. I read that very ad today while looking around at rn jobs to see what’s out there. It was posted by a corporation. So there it is.
I remember when child care, nursing, and teaching were considered careers; nowadays they’re jawbs, having been thoroughly corporatized and crapified.
To those responders who think care work adds little value to an economy, consider that a healthy, educated population is pretty essential to the health of an economy. Think of it as “social infrastructure,” if you will.
In general, to date, this care work has been provided via the unpaid labor of females. I’m betting that’s the easier neoliberal solution than more and larger government programs. Even now, every underfunded public school district in California relies on unpaid female labor to fill in the gaps via “parent involvement” that often means mothers (many of whom were pushed out of the workforce precisely because of childcare issues) are doing the actual work of teaching, for free. It’s amazing what you can wring out of people who’ve been socialized since birth to put the care of others first. (I’m not saying men don’t provide this free labor too, but there’s no question that carework is heavily gendered.)
They recognize that “the market” won’t make a care services based economy work and that it requires serious collective effort through government and that’s good. Now for the little problem of how to make the government work on behalf of the vast majority of citizens and possibly build this economy rather than going with the “just let ’em die” option… I appreciate the work the authors have done here but it’s like they’ve shown that it is possible for human beings to function for several days in zero gravity and walk in one sixth gravity and now we just have to complete the rest of the Apollo program.
What’s required is what we’re sorely lacking: imagination, commitment, and original ideas. Someone upthread mentioned essentially self supporting group homes for the elderly. These are also possible for the handicapped, although they are very, very few and far between. This article described The Shared Living farm environment for autistic adults wherein they perform actual jobs that are meaningful and worthwhile and their language, social, and even cognitive skills improve. Vastly.
http://www.rollingstone.com/culture/features/lukes-best-chance-one-mans-fight-for-his-autistic-son-w431012
Of course infrastructure, but we need to look at this too! ‘Care work or infrastructure’ is a false choice. We need both. I thought a massive push for this should have been in the ARRA stimulus (along with a serious drive to develop new antibiotics… hello, anyone?). The population is aging, care facilities are springing up everywhere, and there are hundreds of thousands of infirm and debilitated people who now get only the barest amount of physical therapy they could use to live better and prevent even more expensive backsliding—not to mention all the need for child daycare.
Is the work unedifying? It’s probably like teaching: if you want good teachers, then offer good pay and benefits. Would a mass program like this be expensive? Not when you’ve got umpteen carrier groups floating around the world, and F-35s sitting grounded while we wage pointless trillion-dollar wars. Is it Big Gubmint? You bet it is, and we’d better wrap our minds around that concept pretty soon. The robots are coming, people! Then employment’s going to get really interesting.
This post seems to assume that if there is a job which needs to done it will be done and we can find jobs there. There are plenty of jobs which need to be done and should be done — no shortage there — but “need” and “should” do little to generate paid employment. Do these authors believe in some a weird form of Says Law applied to a class of labor?
Absolutely, my thoughts were similar. Old and young needing help aren’t cash cows, so where is the money going to come from to pay for these needed jobs? The government? US government isn’t wired that way by priorities sufficiently…yet.
A prerequisite for care work being a positive job growth generator is stopping the confiscation of wealth by the kleptocracy and properly distributing it to those in need in the US. I’m not betting on that happening without a major reset of collective thought in the US. Perhaps when enough millenials vote to make a difference, but that is a ways off.
My point comes from a definite reordering of priorities. Starting with an honest to goodness jobs bill – yes, deficit spending, and a lot of it – such as what Trotskyites like Eisenhower did. So yes, we’re making work for people, or more accurately, paying them decent money for needed work when the market won’t, so that they will in turn spend that money. That is, unless we’re happy with pissing along on 1% growth forever, which seems to be the Washington consensus (because of course Washington’s doing fine).
Also, more progressive taxation, reassessing our vast military spending and subsidies, considering an guaranteed annual income, adopting single payer health care, shortening the workweek, and other Pollyannaish ideas for dealing with a very bleak post-industrial future. Can the Left gain traction on such issues over the next generation before Naked Capitalism’s Jackpot-type features begin materializing? To my mind, that is the central question determining the character of our country hereon.
What do you mean by Naked Capitalism’s jackpot-type features?
Several other portions of your comment seem self-contradictory — e.g. the first sentence of your second paragraph.
At least until recently Naked Capitalism’s links included a Jackpot section of stories that described the dystopian outcomes that are on the way if we don’t change our present path. I don’t remember where Yves’ or Lambert’s original “jackpot” reference came from.
I was trying to offer up other policies we ought to consider in the future. Sorry it was unclear.
Eisenhower was a Trotskyite? No.
It was sarcasm. The broader point being that there was a time when Americans of many political stripes understood the need and good of substantial infrastructure and public spending.
Group care or institutionalized care for children and the elderly, in a post-antibiotic world, also becomes very dangerous. Even now, millions of elderly are dying of c-diff infections contracted in hospitals or nursing homes, and the healthcare industry, overall, is being very quiet about this. But the logic of efficiency demands exactly this kind of grouped, institutionalized care. Simply providing more caretakers isn’t enough –we have to rethink the way we provide that care.
I fully agree with you. The way all our health care is provided needs some rethinking. The Medical Industrial Complex has placed several bottlenecks in the provision of health care — each one diminishing the quality of care while enabling the collection of monopoly rents.
Putting groups of elderly people in assisted living facilities is going to drive state Medicaid spending off the rails much sooner than people think especially in New Hampshire and Maine given their demographics. The answer either isn’t just throwing much larger amounts of poorly-trained and educated home health workers either.
Most elderly people hate leaving their homes and the answer both economically and politically is to try to keep people in their homes as long as possible.
The issue is the American medical system has been in no way set up to make this a priority. Instead you have a jumble of programs at the local, state, and federal with myriads of complexities from state to state depending upon what and how they cover for this issue.