By Phil Galewitz, a Kaiser Health News Senior Correspondent and a former board member of the Association of Health Care Journalists. He previously wrote for The Palm Beach Post, Associated Press and The Patriot-News in Harrisburg, Pa. Originally published at Kaiser Health News
STUART, Fla. — Dr. Christopher Rao jumped out of his office chair. He’d just learned an elderly patient at high risk of falling was resisting his advice to go to an inpatient rehabilitation facility following a hip fracture.
He strode into the exam room where Priscilla Finamore was crying about having to leave her home and husband, Freddy.
“Look, I would feel the same way if I was you and did not want to go to a nursing home, to a strange place,” Rao told her in September, holding her hand. “But the reality is, if you slip at home even a little, it could end up in a bad, bad way.”
After a few minutes of coaxing, Finamore, 89, relented and agreed to go into rehab.
Keeping patients healthy and out of the hospital is a goal for any physician. For Rao, a family doctor in this retiree-rich city 100 miles north of Miami, it’s also a wise financial strategy.
Rao works for WellMed, a physician-management company whose doctors treat more than 350,000 Medicare patients at primary care clinics in Florida and Texas. Instead of being reimbursed for each patient visit, WellMed gets a fixed monthly payment from private Medicare Advantage plans to cover virtually all of their members’ health needs, including drugs and physician, hospital, mental health and rehabilitation services.
If they can stay under budget, the physician companies profit. If not, they lose money.
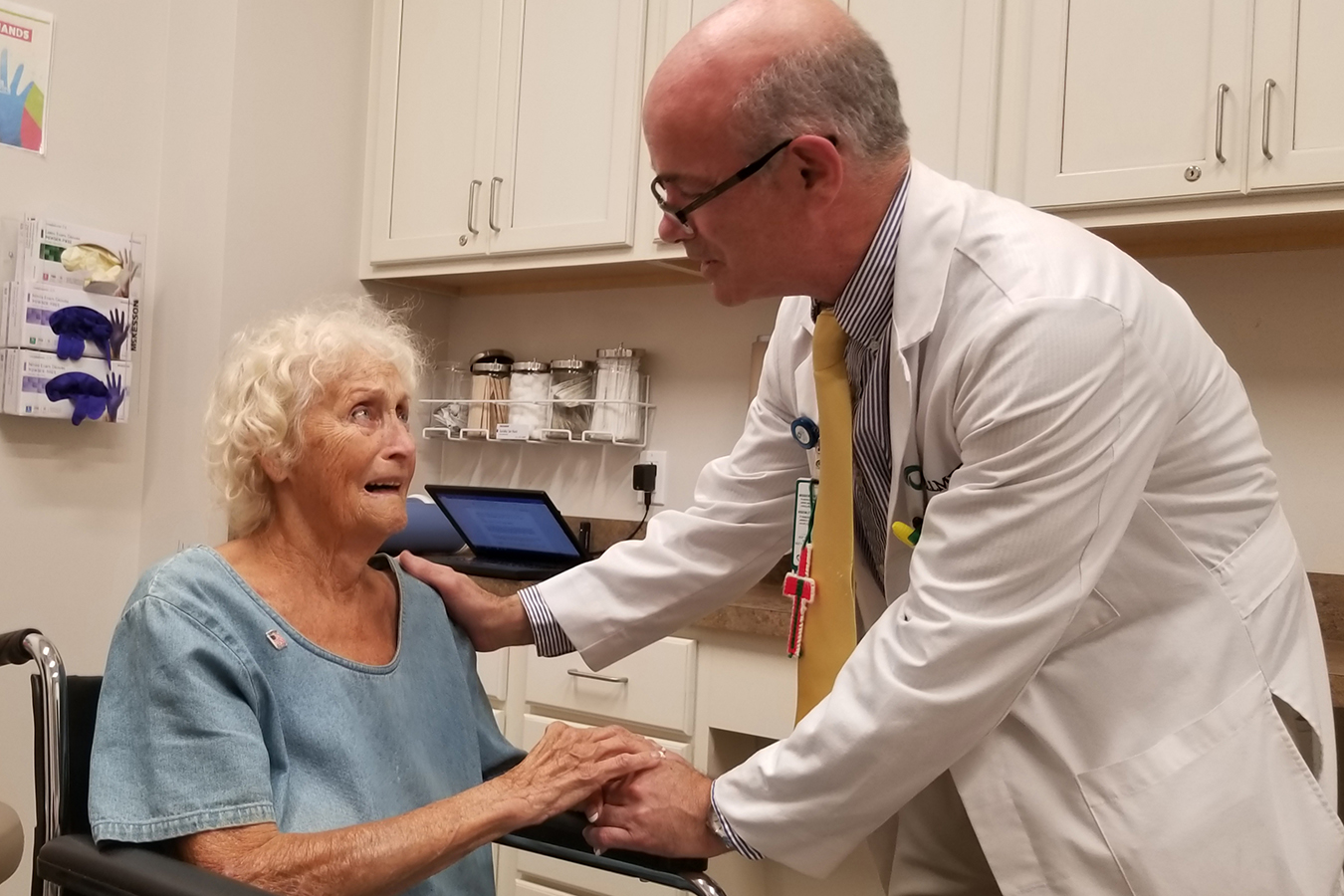
Dr. Christopher Rao, a family doctor at WellMed in Stuart, Fla., comforts Priscilla Finamore about seeking inpatient rehabilitation care. (Phil Galewitz/KHN)
Dr. Christopher Rao, a family doctor at WellMed in Stuart, Fla., comforts Priscilla Finamore about seeking inpatient rehabilitation care.(Phil Galewitz/KHN)
This model — known as “full-risk” or “global risk” — is increasingly used by Medicare plans such as Humana and UnitedHealthcare to shift their financial exposure from costly patients to WellMed and other physician-management companies. It gives the doctors’ groups more money upfront and control over patient care.
As a result, they go to extraordinary lengths to keep their members healthy and avoid expensive hospital stays.
WellMed, along with similar fast-growing companies such as Miami-based ChenMed, Boston-based Iora Health and Chicago-based Oak Street Health, say they provide patients significantly more time with their doctors, same-day or next-day appointments and health coaches. These doctors generally work on salary.
ChenMed doctors encourage their Medicare patients to visit their clinic every month — for no charge and with free door-to-door transportation — to stay on top of preventive care and better manage chronic conditions. If patients are not feeling well after-hours, ChenMed even will send a paramedic to their home.
“We can be much more creative in how we meet patient needs,” said Iora CEO Rushika Fernandopulle. “By taking risk, we never have to ask … ‘Do we get paid for this or not?’”
A Way To ‘Provide Less Care’
Some patient advocates, pointing to similar experiments that failed in the 1990s, fear “global risk” could lead doctors to skimp on care — particularly for expensive services such as CT tests and surgical procedures.
“At the end of the day, this is a way to keep costs down and provide less care,” said Judith Stein, executive director of the Center for Medicare Advocacy.
Dr. Brant Mittler, a Texas cardiologist and trial attorney who has followed the issue, said Medicare Advantage members should be suspicious.
“Patients don’t know that decisions made on their behalf are often financially based. There may be pressure on doctors to cut corners to save money and that may not be in the best interests of a patient’s health,” he said.
The insurers and physician groups disagree. They said limiting necessary care would only exacerbate a patient’s health problems and cost the doctors’ group more money.
Noting that Medicare members stay with Humana an average of eight years, Roy Beveridge, the insurer’s chief medical officer, said the plan would be unwise to skimp on care because that would eventually leave the company with sicker patients and longer hospitalizations.
“It makes even less sense for physicians at financial risk to skimp on care because patients are typically with their physicians much longer than they are with a health plan,” he said.
A study that examined care at ChenMed, published last month in the American Journal of Managed Care, found health costs were 28 percent lower among patients who had more than double the number of typical visits with their primary physician. The study was conductedby researchers at ChenMed and the University of Miami.
To offer more personal care, ChenMed doctors typically see only about a dozen patients per day — about half as many as is usual for a doctor who gets paid for each individual service.
Medicare beneficiaries, who can choose a private health plan during the open-enrollment periodthat runs from Oct. 15 to Dec. 7, generally have no idea if their health plan has ceded control of their care to these large doctors’ groups.
After choosing a Medicare Advantage plan, they generally sign up for a medical group that is part of their health plan’s network, often because doctors are close to where they live or because the doctors offer extra benefits such as free transportation to appointments.
Eloy Gonzalez, 71, of Miami, said that before switching to ChenMed a couple of years ago his doctors always seemed to be in a hurry when he saw them. He’s happy with his ChenMed physicians.
On a recent visit, he spent nearly 20 minutes with Dr. Juana Sofia Recabarren-Velarde talking about keeping his blood pressure and lung condition under control. She also showed him exercises to manage back and shoulder pain.
“If she thinks she needs to see me once a month to monitor my blood pressure and see if anything else is happening, it’s OK with me,” said Gonzalez, who pays nothing for the office visits or generic drugs under his Humana Medicare Advantage plan with ChenMed.
A Growth Spurt
Nearly one-third of the 57 million Medicare beneficiaries are covered by private Medicare Advantage plans — an alternative to government-run Medicare — and federal officials have estimated that the proportion will rise to 41 percentover the next decade. The government pays these plans to provide medical services to their members.
The “global risk” system has been used in South Florida and Southern California since the late 1990s and nearly half of Medicare Advantage members in those regions get care in the model. The use has spread further in the past two years as large physician companies have become more common, and about 10 percent of Medicare Advantage plan members across the nation are in them now, health consultants say.
In addition, new information technology allows these groups to better track their patients. With mixed results, Medicare Advantage insurers for years offered doctors bonuses to meet certain quality care standards, such as getting members vaccinated against the flu or controlling diabetes and other chronic diseases.
Under the “global risk” arrangements, the health plans give the physician companies the bulk of their Medicare funding when they take on the mantle of being financially responsible for all patient care.
For the doctors’ groups, the arrangement means they get paid a large amount of money upfront for patient care and don’t have to worry about billing or having to get insurers to always preapprove treatments.
Because the “global risk” arrangements are designed to reduce plans’ costs, they potentially allow the companies to lower premiums and attract more customers, said Mark Fendrick, director of the University of Michigan’s Center for Value-Based Insurance Design.
“I see this trend continuing to grow as clinicians will be accountable for the first time for the care they provide,” he said.
Historical Lessons
But Ana Gupte, a securities analyst with Leerink Partners in New York, noted providers can also lose money if not successful.
That’s what happened in the late 1990swhen some physician-management companies such as FPA Medical Management and PhyMatrix took on financial risk from insurers only to later go bankrupt, interrupting care to thousands of patients.
Health insurers say they now trust only doctors’ groups that have shown they can handle the financial risk. They also retain varying levels of control. Insurers set benefits, handle member complaints and review which doctors are allowed in its network.
Martin Graf, a partner with consulting firm Oliver Wyman, said the old financial arrangements failed because provider groups did not manage the risks facing their patients.
“Now they know physician groups must be vigilant about their patients — whether they are in the office or not,” he said. “Everyone is aware of the failure of the past.”


Nice mention of Dr. Brant Mittler, I tweeted it so he could see this article as we communicate. Indeed you are correct on the So Cal model, I live there. When you look at managed care, you will also find that United Healthcare is now the largest employer of doctors in the US, more under management than Kaiser. They also have doctors managing hospice care and taking on the risk there as well. Pay for performance, as if they don’t make the bonus money, their income averages around 12% less than Medicare pays with payment for services. Of course, you can add on the OptumRX PBM who controls and manages the prescriptions these patients receive as well, I call it quantcare, it’s not real healthcare anymore. Quantitative Analysts are making too many of the decisions and running it all off of risk assessments, and some of the black boxes are just that when it comes to the risk math associated with the care given.
The Direct primary care model offers a nice alternative for day to day general medical care coupled with having insurance for anything major.
Choosing a Medicare Advantage plan is like checking into the Hotel California. While seniors can switch between competing Advantage Plans during open enrollment, (assuming of course that they live in an area where multiple options are available, and that insurers continue to offer attractive plans) but switching back to Original Medicare is problematic for those with preexisting conditions. While they can re-enter Original Medicare, they cannot be assured of obtaining Medigap or supplemental coverage, leaving them exposed to significant out of pocket expenses for serious illness.
Many Advantage plans, particularly those with low or no premium, are HMO type plans with narrow networks, controlled access to specialists, and all of the other things that make people hate HMOs. And even if a senior finds a plan that works well for their needs and lifestyle, there is no guarantee that the plan will be available in future years.
As far as I can distill it down, Advantage plans usually provide no cost or very low cost prescription meds in return for restricting the physician and facility choices of their members. But the drug formularies are subject to change at any time, so if an expensive drug is dropped from the formulary or placed in a higher cost tier, the senior is s**t out of luck and may be stuck with crappy docs and no way out.
And Advantage plans, as demonstrated by this article, are fast headed for future crapification. Many seniors, completely unbeknownst to them, are being herded via these plans into global risk arrangements in which their entire medical team is incentivized to keep the cost of their healthcare down. I would never let anyone that I cared about choose a Medicare Advantage plan.
One difference between Medicare advantage and a traditional HMO plan, at least for now, is that the flat fee the provider gets from Medicare to provide patient care is pretty generous. My father got pretty sick when he was in such a plan and I was really worried about how his MA HMO would treat him but they were great, even for out of network things when he ended up in the hospital for a week and then with a month of PT while visiting me. I ended up having several long chats with their administrative people and I concluded they were still making money off him, or at least breaking even, despite his care needs.
Of course, no guarantees that will continue. And some HMOs are worse than others.
But he might not be offered a new hip that his healthier peer is able to receive. The real problem with these setups is that, like HMOs, they are a good value when you’re healthy, but woe be the chronically ill. No incentive for doctors to take on difficult referrals. The patient with lifelong PTSD from childhood abuse who develops MS and cancer? Sorry my clinic is currently full.
And that is the name of the game. When it comes to risk management in healthcare nothing beats selecting the healthiest patients otherwise known as cherry picking. And trust me the big plans are really good at cherry picking.
I am a doctor and I have been with Kaiser for over 25 years. I am now in a Medicare advantage plan with Kaiser Southern California. I continue so very pleased with the care I get and the “system” managing my care is terriffic. Anyone who tells you anything negative about this HMO is either not able to figure out how the “system” works or they just got unlucky and have a bad doc. Switching doctors is easy as going online and choosing a new one. No explanation needed. Getting referral to specialist has always been easy for me. Appointments for regular care within 2 weeks. Appointments for specialist care within two weeks. I LOVE KAISER. I will never switch. The surgeons are fantastic. I just had surgery July 19, 2018 And I cannot even hardly see a scar. I have so much confidence in Kaiser doctors I had cataract surgery in both eyes at the same time!
Is Kaiser a huge, fairly wealthy non-profit organization?
Or are they a for-profit company like United Healthcare & Humana called on the carpet by Wall Street hedge funds q 3 mos quarterly report?
I would like to know this also- I’ve heard it both ways. It started as the company doctor system for Henry Kaiser’s industrial empire based in Oakland, CA. If you’ve heard of the “Kaiser Willy” car, he built it. Shipbuilding, aluminum, etc.
Kaiser Permanente is all that’s left. I can’t tell if it is non-profit or owned by a bunch of doctors and is just very well operated.
I won’t settle for Blue cross/aetna etc. after using Kaiser. It’s amazingly good for what it is. But, yes, there are always rough patches and you have to be your own advocate.
It looks like there’s a ton of incentive for these plans to de-select unhealthy, expensive patients. I expect to read horror stories about their failures ten years from now, just like every other time the US health system went with something other than public provision of care.