The evidence of social decay in America is becoming more visible. As other countries continue to show increases in life expectancy, the US continues its deterioration.
Life expectancy in the US fell to 78.6 years in 2017, a o.1 year fall from 2016 and a 0.3 year decline from the peak.
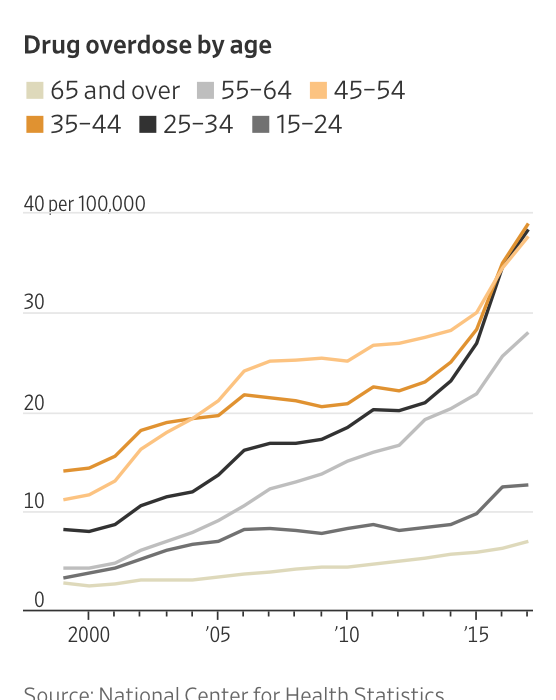
Overdose deaths reached a new high in 2017, topping 70,000, while the suicide rate increased by 3.7%, the CDC’s National Center for Health Statistics reports.
Dr. Robert Redfield, CDC director, called the trend tragic and troubling. “Life expectancy gives us a snapshot of the Nation’s overall health and these sobering statistics are a wakeup call that we are losing too many Americans, too early and too often, to conditions that are preventable,” he wrote in a statement.
While this assessment is technically correct, it is too superficial in seeing the rising rate of what Angus Deaton and Ann Case called “deaths of despair” as a health problem, rather than symptoms of much deeper societal ills. Americans take antidepressants at a higher rate than any country in the world. The average job tenure is a mere 4.4 years. In my youth, if you changed jobs in less than seven or eight years, you were seen as an opportunist or probably poor performer. The near impossibility of getting a new job if you are over 40 and the fact that outside hot fields, young people can also find it hard to get work commensurate with their education and experience, means that those who do have jobs can be and are exploited by their employers. Amazon is the most visible symbol of that, working warehouse workers at a deadly pace, and regularly reducing even white collar males regularly to tears.
On top of that, nuclear families, weakened communities, plus the neoliberal expectation that individuals be willing to move to find work means that many Americans have shallow personal networks, and that means less support if one suffers career or financial setbacks.
But the big driver, which the mainstream press is unwilling to acknowledge, is that highly unequal societies are unhealthy societies. We published this section from a Financial Times comment by Michael Prowse in 2007, and it can’t be repeated often enough:
Those who would deny a link between health and inequality must first grapple with the following paradox. There is a strong relationship between income and health within countries. In any nation you will find that people on high incomes tend to live longer and have fewer chronic illnesses than people on low incomes.
Yet, if you look for differences between countries, the relationship between income and health largely disintegrates. Rich Americans, for instance, are healthier on average than poor Americans, as measured by life expectancy. But, although the US is a much richer country than, say, Greece, Americans on average have a lower life expectancy than Greeks. More income, it seems, gives you a health advantage with respect to your fellow citizens, but not with respect to people living in other countries….
Once a floor standard of living is attained, people tend to be healthier when three conditions hold: they are valued and respected by others; they feel ‘in control’ in their work and home lives; and they enjoy a dense network of social contacts. Economically unequal societies tend to do poorly in all three respects: they tend to be characterised by big status differences, by big differences in people’s sense of control and by low levels of civic participation….
Unequal societies, in other words, will remain unhealthy societies – and also unhappy societies – no matter how wealthy they become. Their advocates – those who see no reason whatever to curb ever-widening income differentials – have a lot of explaining to do.
And this extract comes from a 2013 article, Why Are Americans’ Life Expectancies Shorter than Those of People in Other Advanced Economies?
Let’s talk life expectancy.
The stats first. They tell a clear story: Americans now live shorter lives than men and women in most of the rest of the developed world. And that gap is growing.
Back in 1990, shouts a new study published last week in the prestigious Journal of the American Medical Association, the United States ranked just 20th on life expectancy among the world’s 34 industrial nations. The United States now ranks 27th — despite spending much more on health care than any other nation.
Americans, notes an editorial the journal ran to accompany the study, are losing ground globally “by every” health measure.
Why such poor performance? Media reports on last week’s new State of U.S. Health study hit all the usual suspects: poor diet, poor access to affordable health care, poor personal health habits, and just plain poverty.
In the Wall Street Journal, for instance, a chief wellness officer in Ohio opined that if Americans exercised more and ate and smoked less, the United States would surely start moving up in the global health rankings.
But many epidemiologists — scientists who study health outcomes — have their doubts. They point out that the United States ranked as one of the world’s healthiest nations in the 1950s, a time when Americans smoked heavily, ate a diet that would horrify any 21st-century nutritionist, and hardly ever exercised.
Poor Americans, then as now, had chronic problems accessing health care. But poverty, epidemiologists note, can’t explain why fully insured middle-income Americans today have significantly worse health outcomes than middle-income people in other rich nations.
The University of Washington’s Dr. Stephen Bezruchka has been tracking these outcomes since the 1990s. The new research published in the Journal of the American Medical Association, Bezruchka told Too Much last week, should worry Americans at all income levels.
“Even if we are rich, college-educated, white-skinned, and practice all the right health behaviors,” he notes, “similar people in other rich nations will live longer.”
A dozen years ago, Bezruchka published in Newsweek the first mass-media commentary, at least in the United States, to challenge the conventional take on poor U.S. global health rankings.
To really understand America’s poor health standing globally, epidemiologists like Bezruchka posit, we need to look at “the social determinants of health,” those social and economic realities that define our daily lives.
None of these determinants matter more, these researchers contend, than the level of a society’s economic inequality, the divide between the affluent and everyone else. Over 170 studies worldwide have so far linked income inequality to health outcomes. The more unequal a society, the studies show, the more unhealthy most everyone in it — and not the poor alone.
Just how does inequality translate into unhealthy outcomes? Growing numbers of researchers place the blame on stress. The more inequality in a society, the more stress on a daily level. Chronic stress, over time, wears down our immune systems and leaves us more vulnerable to disease.
The Wall Street Journal has more detail on the breakdown of the further decline in US life expectancy, and also points out how other countries are continuing to show progress:
Data the Centers for Disease Control and Prevention released on Thursday show life expectancy fell by one-tenth of a year, to 78.6 years, pushed down by the sharpest annual increase in suicides in nearly a decade and a continued rise in deaths from powerful opioid drugs like fentanyl. Influenza, pneumonia and diabetes also factored into last year’s increase.
Economists and public-health experts consider life expectancy to be an important measure of a nation’s prosperity. The 2017 data paint a dark picture of health and well-being in the U.S., reflecting the effects of addiction and despair, particularly among young and middle-aged adults, as well as diseases plaguing an aging population and people with lower access to health care…
Life expectancy is 84.1 years in Japan and 83.7 years in Switzerland, first and second in the most-recent ranking by the Organization for Economic Cooperation and Development. The U.S. ranks 29th..
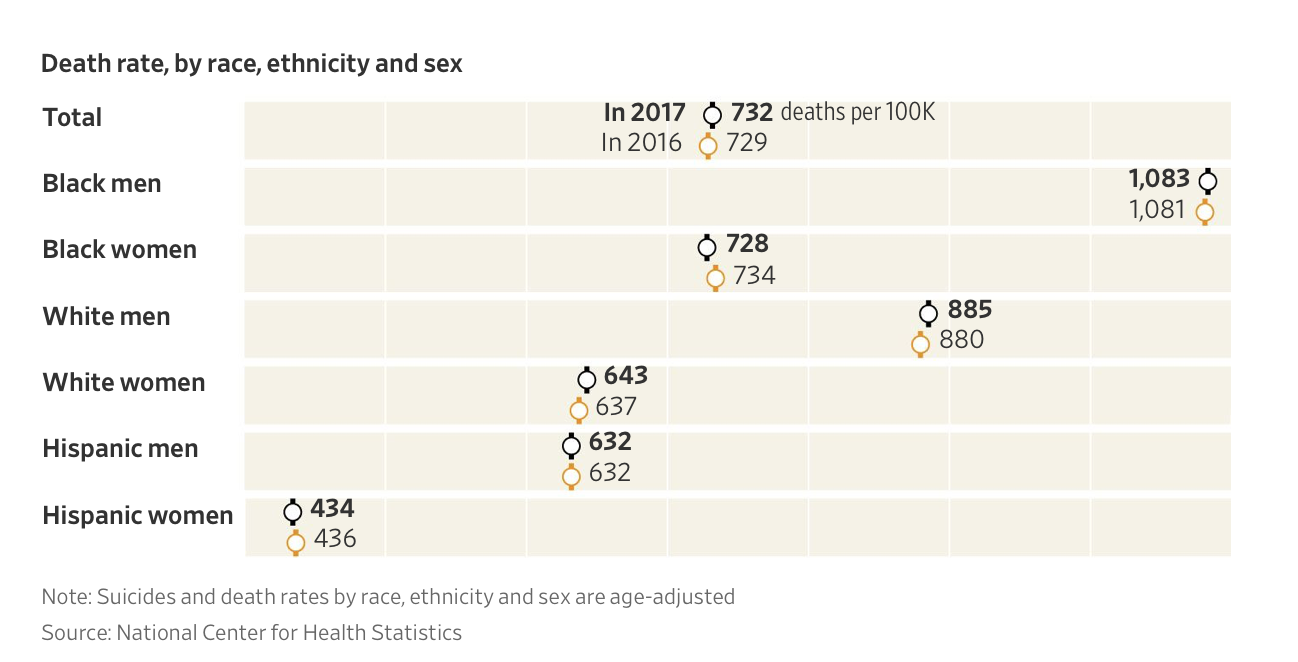
White men and women fared the worst, along with black men, all of whom experienced increases in death rates. Death rates rose in particular for adults ages 25 to 44, and suicide rates are highest among people in the nation’s most rural areas. On the other hand, deaths declined for black and Hispanic women, and remained the same for Hispanic men….
Earlier this century, the steady and robust decline in heart-disease deaths more than offset the rising number from drugs and suicide, Dr. Anderson said. Now, “those declines aren’t there anymore,” he said, and the drug and suicide deaths account for many years of life lost because they occur mostly in young to middle-aged adults.
While progress against deaths from heart disease has stalled, cancer deaths—the nation’s No. 2 killer—are continuing a steady decline that began in the 1990s, Dr. Anderson said. “That’s kind of our saving grace,” he said. “Without those declines, we’d see a much bigger drop in life expectancy.”…
Suicides rose 3.7% in 2017, accelerating an increase in rates since 1999, the CDC said. The gap in deaths by suicide widened starkly between cities and the most rural areas between 1999 and 2017, the data show. The rate is now far higher in rural areas. “There’s a much wider spread,” Dr. Hedegaard said.
“This is extremely discouraging,” Christine Moutier, chief medical officer of the American Foundation for Suicide Prevention, said of the suicide-rate increase. Studies show that traumas such as economic difficulties or natural disasters, along with access to lethal means including guns and opioid drugs, and lack of access to care can affect suicide rates, she said. More accurate recording of deaths may also have added to the numbers, she said.
Japan leads the pack in life expectancy and pretty much every other measure of social well being. Yet when its financial bubbles were bigger than the ones in the US pre our crisis, and it’s on its way to having a lost three decades of growth. On top of that, Japan has one of the worst demographic crunches in the world, in terms of the aging of its population. So how it is that Japan is coping well with decline, while the US is getting sicker in many ways (mental health, obesity, falling expectancy)?
It’s easy to hand-wave by saying “Japanese culture,” but I see the causes as more specific. The Japanese have always given high employment top priority in their economic planning. Entrepreneurs are revered for creating jobs, not for getting rich. Similarly, Japan was long criticized by international economist types for having an inefficient retail sector (lots of small local shops), when they missed the point: that was one way of increasing employment, plus Japanese like having tight local communities.
After their crisis, Japanese companies went to considerable lengths to preserve jobs, such as by having senior people taking pay cuts and longer term, lowering the already not that large gap between entry and top level compensation. The adoption of second-class workers (long-term temps called “freeters”) was seen as less than ideal, since these workers would never become true members of the company community, but it was better than further reducing employment.
Contrast that to our crisis response. We reported in 2013 that the top 1% got 121% of the income gains after the crisis. The very top echelon did better at the expense of everyone else. Longer term, lower-income earners have fallen behind. From a 2017 MarketWatch story, quoting a World Economic Forum report: “America has experienced ‘a complete collapse of the bottom 50 percent income share in the U.S. between 1978 to 2015.’”
There is a lot of other data that supports the same point: inequality continues to widen in America. The areas that are taking the worst hits are states like West Virginia and Ohio that have been hit hard by deindustrialization. But the elites are removed in their glamorous cities and manage not to notice the conditions when they transit through the rest of America. They should consider themselves lucky that America’s downtrodden are taking out their misery more on themselves than on their betters.


God, this is so depressing to read. The worse aspect of it is that it never had to be this way but that these deaths were simply ‘collateral damage’ to the social and economic changes in America since the 1970s – changes by choice. This seems to be a slow motion move to replicate what Russia went through back in the 1990s which led to the unnecessary, premature deaths of millions of its people. Dmitry Orlov has a lot to say about the subject of collapse and there is a long page in which Orlov talks about how Russia got through these bad times while comparing it with America as he lives there now. For those interested, it is at-
http://energyskeptic.com/2015/dmitry-orlov-how-russians-survived-collapse/
What gets me most is how these deaths are basically anonymous and are not really remembered. When AIDS was ravishing the gay community decades ago, one way they got people to appreciate the numbers of deaths was the AIDS Memorial Quilt which ended up weighing over 50 tons. It is a shame that there can not be an equivalent project for all these deaths of despair.
There were pictures in the Wall Street Journal article I didn’t pull over due to copyright issues, but it did show people commemorating these deaths Captions:
But to your point, these seem isolated and are not getting press coverage at anywhere near the level of the AIDS crisis.
Great post, Yves, thank you! One suggestion: might you consider putting the last word in quotes, as in “betters” ?
It focuses too much on peak oil. As if the social collapse of the United States (and the Soviet Union) was some kind of natural consequence of resources dryinf out instead of a premeditated looting.
Orlov’s posts on how Russians survived the collapse is a small masterpiece. I read it a couple of years back and it affected me greatly. I just reread it, thanks, Rev Kev, and it seems even more relevant now.
Small gems: Money becomes useless: items or services that can be swapped are paramount. Bottles of alcohol, fresh homegrown veggies (and pot), I re-fashion your old suit and you fix my broken window.
Social networks keep you alive. Know and be on good terms with your neighbors. Communal gardens keep you fed.
War-hardened men (and the women who love them), who thrive on violence abound. They will either be hired as security or rove about as free-lancers. A community is better able either to hire them, or defend against them.
Our ancestors lived and thrived without: central heating, electric lights, hot and cold running water, flush toilets, garbage collection, the Internet. We can too; it just takes forethought and planning. Densely packed cities without these amenities are hell.
Cultivate an attitude of disdain for the ‘normal’ things that society values, especially if you are a middle-aged male; career, large house and SUV, foreign vacations, a regular salary. Enjoy contemplating nature. When the former disappear, you have the latter to fall back upon. And consider a second career as a recycler of abandoned buildings, or a distiller of potatoes. (Think of all the Medieval structures built from crumbling Roman edifices.)
Russians, in many ways, had more resilience built in to their system: housing was State-owned, so there was less homelessness. Private automobiles were relatively rare, but public transportation was wide-spread and remained in good-running order. Minimal universal health care existed.
Cease from trying, futilely, to change the System. Ain’t gonna happen. Instead, prepare to survive, if only just, the coming dismantling.
> Once a floor standard of living is attained, people tend to be healthier when three conditions hold: they are valued and respected by others; they feel ‘in control’ in their work and home lives; and they enjoy a dense network of social contacts.
“Sapolsky: We belong to multiple hierarchies, and you may have the worst job in your corporation and no autonomy and control and predictability, but you’re the captain of the company softball team that year and you’d better bet you are going to have all sorts of psychological means to decide it’s just a job, nine to five, that’s not what the world is about. What the world’s about is softball. I’m the head of my team, people look up to me, and you come out of that deciding you are on top of the hierarchy that matters to you.”
iirc, there was a perspective of some economists that infinite groaf could be carried by the creative, emergent, and infinite wants of homo sapiens. But that creates compounding deprivations, never enough time, money, resources. With the 2:1 ratio of loss aversion, what is compounded are bad affects.
That ‘dense network of social contacts’ means smaller groups with symmetric interactions. The multiple dominance heirarchies is the healthy version of creative emergence, but supplying needs, not creating wants.
I think that one of the most valuable tools used by government in the Great Depression was the CCC, WPA, and TVA set of programs that provided jobs to people while they created valuable infrastructure and art. How many of those people could go back to the dams or state parks and tell their spouses and kids that “I helped build that.” During a time of despair, it was a way of making people believe they had value.
Today, it would be viewed as a waste of money that could be better spent on the military or another tax cut for the wealthy.
I’d mentioned some wrongheaded policies of Sequoia NP of 90 years ago yesterday, and they seem ridiculous in retrospect, and we no longer treat natural places as ad hoc zoos, where everybody gets to see the dancing bears @ a given hour.
Our methodology as far as our rapport with fire was just as stupid, but we’ve really done nothing to repair our relationship with trees and the forests they hang out in.
There’s an abundance of physical labor needed to clear out the duff, the deadfalls and assorted debris from huge swaths of guaranteed employment until the job is done, which could take awhile.
There’s really few graft possibilities though, we’re talking chainsaws, Pulaskis, never ending burn pile action and lots of sweat equity. If KBR wanted to be in charge of backcountry camps housing crews, that’d be ok, they’d be doing something useful for a change.
Yes, why do you think video games appeal so much to young males? Because of the pixels? What these gamers are really after is the ability to excel in a niche hierarchy. It doesn’t (usually) appeal to females as much as more traditional kinds of success but it serves a psychological need.
A traitorous ruling class that has sold out its workers in favor of foreign workers.
And it’s very lucrative – the Walton’s fortune was made by being an agent of communist Chinese manufacturers. In direct competition with US manufacturers. Does this not seem like treason to you?
The word ‘communist’ in relation to the Chinese government and party is void of content. ‘Communist’ in the current Chinese context is legacy branding, nothing more. Its use in this comment is inflammatory, as is the too-loose bandying of ‘treason’. The Waltons are loyal to their class (however fierce their disputes may be with rival oligarch factions), and since the state exists to serve the interests of their class, how can they be traitors to the state?
“Communist” is what they call themselves. They’re totalitarians. Which is what most people think “communist” means – because all countries that called themselves communist used authoritarian rule. Methinks you might be a marxist idealist. Offended by the misuse of your ideal State word by totalitarians.
Similarly, I used “treason” in the sense of acting against the interests of the citizens, not in the sense of a crime against the state. You clearly believe the state to be representative of only the ruling class. And I don’t disagree wrt the USA and its imperial machine. Which would make the State treasonous, according to the sense of the word I used.
One could always say communism is an end point developed through a process preceded by socialism and before that capitalism which replaces feudalism. The idea being Chinese Communists, the rich Chinese have bug out spots for a reason, believe Mao and the Soviets moved too quickly skipping a Marxist historical epoch.
The Communist Party officially is always a vanguard for the future society not the Communist society. Phrases such as “under communism” aren’t Soviet features as much as they are propaganda from the West.
When the Reds were the only game in town, the greedy class joined the CCP, but since 1991, they skipped signing up, leaving believers in control. What the party congress believes is probably important.
As far as branding goes, all Communists are branded because the are all vanguard parties, not parties of blocs or even current populations. Star Trek is the only communist society. The Soviet thinkers definitely wrote about what an Ideal society would look like, the nature of work, and self and societal improvement.
Overthrowing a long established government shouldn’t be done for light and transient reasons, and Xi has seemed to be concerned with the demands of the party congress. The party at large doesn’t have a single voice to rally behind which makes it difficult to overthrow a government.
the word is “communist”. The gov’t isn’t anything of the sort these days. Isn’t the chinese gov’t of today “fascist”. just like the national socialists of the german stripe? They are the state that may be lord over controller of private institutions, and ruler of other state institutions, all intermixed into what is “the chinese economy”. They allow the private wealth creation in a controlled sense. that is state function serving private wealth. and if you are a party loyal, private wealth may come to you some day too.
It is just another part of the world trend “everyone is turning into full fledged fascists”
No wonder people in the states are dying earlier.. to get back on topic
Last night, my wife and I took our boys to meet Santa at my older son’s school. Elementary school in Mississippi. The town is an outer suburb of Memphis. A mile east of the town you are in rural Mississippi. I noticed 2 or 3 parents with visible drug addiction issues. These folks were still people. Want their kids to see Santa and have a better life. The country doesn’t care.
I’ll guess that you’re near Byhalia. Happy memories of visiting family there from late forties through sixties. Wonder what its like now – how the economic changes have affected it.
Byhalia is a little further down highway 78. Kids from Byhalia drive up to Olive Branch to go to a McDonald’s and other fast food. Things may be changing because they just completed an outer interstate loop that passes close by Byhalia. Byhalia was just in news a couple months ago because a kid died during a football game. People were up in arms about no doctor at game and a 30 to 40 minute drive to closest hospital. There aren’t any doctors offices in Byhalia. Then toxicology report came back. Kid had cocaine in his system. Holly Springs and Byhalia area are big drug smuggling area. Close to Memphis and it’s distribution network, but across state line in poor rural Mississippi. NBA players linked to this area and smuggling networks.
I’m always amazed @ the suicide by gun numbers, as it strikes me as a not so fool proof way of checking out, exacerbated by perhaps dying slowly in a painful way?
Oh, and bloody, very much so.
Fentanyl seems an easier way out, you just drift into the ether and leave a presentable corpse for everybody you knew, who all wonder if they could have done something to stop it from happening, posthaste.
It’s cheap and fairly efficient, and the drug way out can be tricky. Silent film legend, Lupe Valez, is the famed example of suicide by drugs gone wrong. She still died but not on her own terms because the sleeping pills she took didn’t react well with her last meal.
How many people have tried to check out and had it not work is something to consider.
Re Lupe Valdez: probably not true, at least according to the Wikipedia page. Not that it affects your point too much, I guess.
The level of denial people are capable of can be daunting.
1). My dentist who I think is Republican told me when I brought up Medicare for all said “I don’t think we can afford Medicare for all.” This was not an immediate response to my raising the topic, but something he told me after several visits and having thought about what I had said and around the time Sanders got media coverage introducing a Medicare for all bill (I was getting a crown and required many visits). Talking to your dentist can be a one sided conversation for obvious reasons, but I thought “don’t you mean we can’t afford NOT to have Medicare for all?”
2). A co-worker of mine who is African American. When I said U.S. life expectancy is falling, this is a sign of extreme policy failure and should affect how we rate the ACA (read that here, of course!) replied “You’re assuming health has an impact on life expectancy.” I was stunned and didn’t know what to say for a second and finally said “yes, absolutely.”
These are the types that are more than happy to hand the place over to the next Bolsonaro if only to protect the status gap between themselves and those beneath them.
They also “hand the place over” when the Bolsonaro types tell everyone they have the solution and the opposition party is tainted by austerity and corruption.
“You’re assuming health has an impact on life expectancy”
I have absolutely no idea how I would respond to this either. Was this comment by this person some kind of built in knee-jerk response to criticism of the ACA/Obama?
Opps I meant to write “You’re assuming health CARE has an impact on life expectancy.”
In response to your question, I think so, yes.
actually you are assuming health coverage, even if it was real coverage for what one needed, has that much of an impact on life expectancy and from what I’ve read it probably doesn’t compared to things like poverty *regardless* of health coverage. Because the greatest link to say heart attacks is with poverty (not diet etc.)
At this point though it doesn’t even make sense to talk about the ACA circa now and say it’s Obama’s ACA, it wasn’t that great to begin with. But Trump has made it worse.
My dentist who I think is Republican told me when I brought up Medicare for all said “I don’t think we can afford Medicare for all.”
When I brought up Medicare for All to my dentist, after listening to him describe some of his ER work where he claims to routinely see people who have intentionally damaged their teeth in order to obtain painkillers (which he is not allowed to proscribe to them regardless), he said he would never want to have the kind of inferior health care they have “in Europe.” He seemed genuinely surprised when I reported that my wife had done most of a pregnancy in Italy in the mid-90s and got pre-natal care that was better than anything she ever got in this country.
My dentist is definitely a Repub. And he socializes with other medical professionals, which I presume gives him a very distorted image of the health care system. I often hear him railing against the idiotic dictates of insurance companies and he seems genuinely proud that, unlike the inscrutable and BS pricing of hospitals, dentists have to have straightforward pricing because many people do pay 100% out of pocket (so he says).
This is a part of the 10% that is going to be very hard to reach. But I tell him socialists need dental care too and so he will always have work even after we take over.
Suicide can be a rational and sensible choice.
Bluntly, if the quality of your life is shitty and not going to improve why stick around?
That the reason so many people’s lives are bad enough that they decide death is preferable to life is societal doesn’t change their circumstances.
If you are old and sick, barely surviving financially or in poor health and unable to afford care suicide might look like your best alternative.
The “Hemlock Society” has been around for quite a while, that its membership is growing in the short term says a great deal about America.
Suicide is never rational. It is arrogance that one could weigh the pros and cons of suicide like they think the have all the pertinent information. The only truth is that we have no idea what happens when we die or if there is some kind of experience that continues in a form that might not be a personal consciousness. Also, why don’t you see the decision to die is made under duress and therefor invalid like signing a contract with a gun pointed at your head? There were several times in my life that I determined “the quality of [my] life is shitty and not going to improve [so] why stick around”, but yet, I became better off going through the struggle. As a result I have made others lives better with the understanding I have gained going through the Shaman’s journey.
By considering suicide you are considering trading a known (suffering) for an unknown (Death). In what way can that be considered rational?
The sad fact is that we spend our whole lives avoiding suffering and never take the time to understand it. Opioids, all drugs, are a route to avoid suffering, to avoid looking at our trauma. Materialism is about avoiding our suffering. Suicide is materialistic because it supposes there is a mind that we can stop.
But even in the Buddhist centers I visit it has turned away from the spiritual and people go there not to understand their suffering, but rather only to escape it.
American society does not have an economic problem, it has a spiritual problem.
I respect your view that suicide is an arrogant act and that suffering is an unavoidable part of life. I totally agree with the latter philosophy. You suffer, and you wade through it and come out on the other side as a better person. Forged in fire, so to speak.
Plus, I am, by nature, an optimist. There is always something to look forward to, every morning.
But, a few years ago, I suffered a cascade of bodily failures, whose symptoms were at first ignored, then misdiagnosed, resulting in my taking medications that made me worse off. At one point, for two months, I had constant nerve pain (comparable to having teeny barbed wire wrapped around my torso and and being zapped by an electric charge every few seconds.) Plus back pain. I could not eat, and when I did, I vomited. I lost 20 pounds. I could not sleep for more than hour at a time, and that hour happened only once a day. I walked only with the aid of two walking sticks. I was totally constipated for a month (gross, but this condition just adds to one’s misery.) There was no end in sight and my condition just kept worsening with each round of new medication.
I did not seriously contemplate suicide. But I did give some thought to what I would do if I had to face life without sleep, without food, without the ability to walk, and death came up as one of the better solutions. Fortunately, I changed doctors.
I empathize with your struggles, and I have contemplated suicide myself, but contemplating death is part of the shaman’s journey. I do not think that suicide is arrogant, I think it is a misunderstanding.
IMHO, medical doctors will disrupt this journey. They should be consulted but with the understanding that they know very little about the balance of the body and what is needed to heal.
Truth is, we will die. The greater the suffering the easier to find out “who” that is suffering.
“Life teaches you how to live it, if you live long enough.”.
-Tony Bennett
“Suicide is never rational” is an arrogant assertion.
Even if it *is* a ‘rational’ choice, that is because the system is absolutely broken and must be changed.
+1000
I get in fights with my therapist all the time about this. She is always advocating for ME to change when I feel if she wants to help us all she should be helping us change the system.
Well roles like therapist are part of what props up the system and they get paid for precisely that.
I mean if we are just living our lives we see that things are both individual and systematic. And some things are strongly systematic (economic problems), and others probably have a significantly personal component (phobias etc.). And so we have to exist with both being true, but if we are drowning in economic problems the rest doesn’t matter. But therapists have a specific role to individualize all problems. But if people are just doing therapy to get stuff off their chest, who can blame them. Enough people are, although it’s not how therapists like to see their role.
Lifespan dropping, mortality going up…
Are we tired of winning yet???
The only real visible sign of decay on the train to DC from Boston is Baltimore, which nearly appears bombed out.
The train goes right by Chester, Pa, and you can see decay along the tracks all along BosWash. Except for Biden, a corrupt tool who hasn’t figured out how to cash in, the elites don’t take the train.
Remember the Kingsman movie where the president was going to let all the dopers die? Think Trump.
Not only is the WH response to the opioid problem merely cosmetic, they (and NIH) refuse to link it to the economics of human obsolescence. How convenient. As jobs die, the workers do too – less welfare burden. That is fascist thinking, and it is evident today.
Finally, let us recall that all public health leaders are Trump appointees – i.e., incompetent. CDC too refuses to link suicide to the economy. It’s bad politics. They can do this because there are no national standards for reporting deaths as suicides or even drug overdoses. It is entirely up to the elected coroner. Thus 10s of thousands of suicides are reported as natural or accidental either intentionally to ease the grief of family members or because they lack the manpower to investigate suspicious deaths. Note the bump in accidental deaths. Driving your car into a concrete abutment or over a cliff might be an accident, but more often than not, the driver was pickled (Irish courage) and the death was intentional.
So, until we do a better job of measuring the causes of death, the administration can continue to blame the deaths on moral weakness rather than its cruel economic policies.
Well we might not be thriving, but our empire is thriving. And the empire has a simple message for us: embrace the suck.
Sadly, I believe if suicide attempts were taken into account, the picture would even look far bleaker, and likely include far more Metro areas. In those Metro areas there are likely far less gun/rifle owners (reportedly the most successful method), far quicker ambulance response times, and significant expenditures have been made, and actions taken, to thwart attempts on transit lines and bridges, along with committing suicidal persons to locked down psychiatric facilities (which then adds further financial burden, significant employment issues, and possibly ugly, forced medication side effects); while doing absolutely nothing whatsoever to address the causes.
What a sickening blotch on the US, with such wealth and power – sovereign in its own currency – that it’s citizens are increasingly attempting and committing suicide because they can no longer afford to live in any manner that’s considered humane. That, while its Fourth Estate deliberately obscures the deadly problem – which cannot be cured by forcing Pharma™, Therapy™, and Psychiatric Confinement™ at it, when a predatory crippling of economic stability is the entire cause – and refuses to hold the Government and Elites accountable.
I would commend to all Beth Macy’s riveting book “Dopesick: Dealers, Doctors, and the Drug Company that Addicted America.”
Equal parts nicely written investigative reporting and painful personal stories. I’d thought that the “opioid epidemic” meme was hyperbolic. I was wrong.
This happened in Russian and Eastern European countries too didn’t it?