By Lambert Strether of Corrente
I was considering using “All that is fomites melts into air,” but I couldn’t bring myself to, so count yourself lucky (and anyhow, it’s not really true). From the beginning of the #COVID19 pandemic, we’ve been washing our hands, masking up, cleaning surfaces, and social distancing. These measures have worked (especially masking), but now we know more. There’s mounting evidence that airborne transmission indoors is a key — perhaps the main — pathway to SARS-COV-2 transmission. In this post I want to look at why that’s so, give examples, and suggest a simple heuristic to stay safe. Material like this might also be used to inform public policy (here; here) by reducing superspreader events in enclosed spaces like churches (airborne transmission via singing), restaurants (loud talking, especially if room is noisy), bars (ditto), nursing homes (shouting[1]), gyms (grunting), meat-packing plants (shouting), call centers (talking), offices generally (air conditioning), and other hot spots, but working that polucy out is not the object of this post (see here for engineering controls for airborne transmission, and here for covid-proofing public spaces).
Airborne Transmission of SARS-CoV-2 Indoors
This article from PNAS seems to be the index publication for airborne transmission. From “The airborne lifetime of small speech droplets and their potential importance in SARS-CoV-2 transmission“:
Speech droplets generated by asymptomatic carriers of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) are increasingly considered to be a likely mode of disease transmission. Highly sensitive laser light scattering observations have revealed that loud speech can emit thousands of oral fluid droplets per second. In a closed, stagnant air environment, they disappear from the window of view with time constants in the range of 8 to 14 min, which corresponds to droplet nuclei of ca. 4 μm diameter, or 12- to 21-μm droplets prior to dehydration. These observations confirm that there is a substantial probability that normal speaking causes airborne virus transmission in confined environments.
That experiment was done inside a box. Vox translates to real world terms:
A crowded indoor place, then, with poor ventilation, filled with people talking, shouting, or singing for hours on end will be the riskiest scenario. A sparsely populated indoor space with open windows is less risky (but not completely safe). Running quickly past another jogger outside is on the other end of the spectrum; minimal risk.
(In other words, the problem is not density or proximity; the problem is transmission of the virus, through the air, by human vocalization[2] (of which coughing and sneezing are a small, and symptomatic, subset.)
That would explain why masks have worked. (One could argue that masks need only be worn indoors, but most people are constantly moving from the outdoors to the indoors and out again, which would involved touching the mask constantly to remove and replace it; better to wear it all the time. In any case, minimal risk, to others, is not no risk). From the South China Morning Post, “Coronavirus: hamster research shows effectiveness of masks ‘huge’ in Covid-19 battle, Hong Kong scientists say”:
Hong Kong scientists conducting research on hamsters have offered the first proof of what many residents have believed all along – that wearing surgical masks can significantly reduce the rate of airborne Covid-19 transmission.
The study, which the team called the first of its kind, found the rate of non-contact transmission – in which the virus was transmitted via respiratory droplets or airborne particles – dropped by as much as 75 per cent when masks were present.
(See also “If 80% of Americans Wore Masks, COVID-19 Infections Would Plummet, New Study Says,” from Vanity Fair.)
Examples of Airborne Transmission of SARS-CoV-2 Indoors
So far as I can tell, there are two main villains: Air conditioning, and vocalization:
Air conditioning. Here is the very first article I spotted on airborne transmission, back on March 9, 2020. From the South China Morning Post, “Coronavirus can travel twice as far as official ‘safe distance’ and stay in air for 30 minutes, Chinese study finds”
A passenger, known as “A”, boarded a fully booked long-distance coach and settled down on the second row from the back.
The passenger already felt sick at that point but it was before China had declared the coronavirus outbreak a national crisis, so “A” did not wear a mask, nor did most of the other passengers or the driver on the 48-seat bus.”It can be confirmed that in a closed environment with air-conditioning, the transmission distance of the new coronavirus will exceed the commonly recognised safe distance,” the researchers wrote in a paper published in peer-review journal Practical Preventive Medicine last Friday. They said the study proves the importance of washing hands and wearing face masks in public places because the virus can linger in the air attached to fine droplet particles.
Here is a seating chart of the bus:
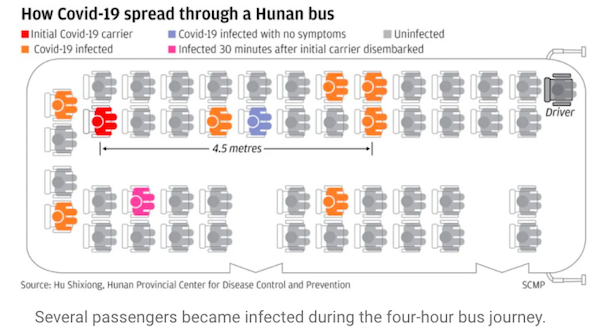
After reading this, I altered my practice not to mask up, which I was already doing, but to avoid (air-conditioned) public transportation entirely, and indeed air-conditioned spaces entirely.
Here is a second example, a Chinese restaurant. From the CDC’s Emerging Infectious Diseases, “COVID-19 Outbreak Associated with Air Conditioning in Restaurant, Guangzhou, China, 2020“:
We conclude that in this outbreak, droplet transmission was prompted by air-conditioned ventilation. The key factor for infection was the direction of the airflow. Of note, patient B3 was afebrile and 1% of the patients in this outbreak were asymptomatic, providing a potential source of outbreaks among the public (7,8). To prevent spread of COVID-19 in restaurants, we recommend strengthening temperature-monitoring surveillance, increasing the distance between tables, and improving ventilation.
Here again is a seating chart:
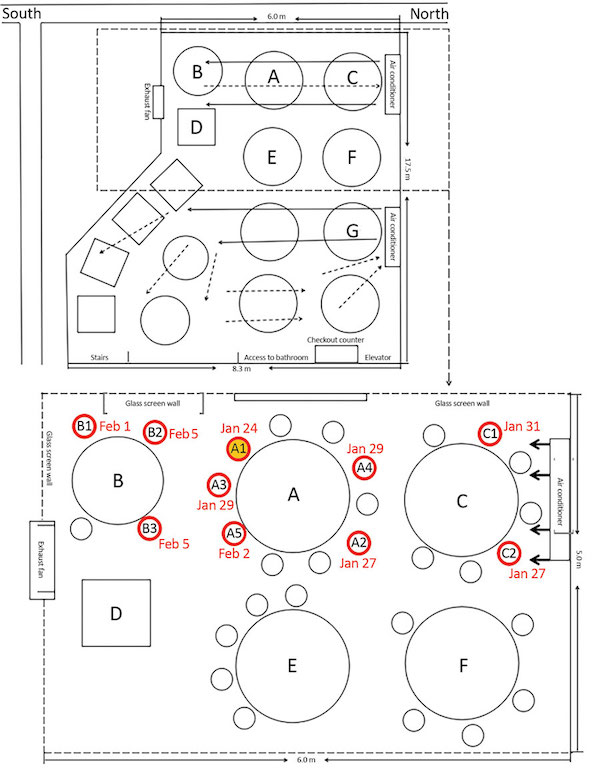
I was already not going to restaurants because of the Chinese bus episode, if I had been, I would have stopped. One can’t wear a mask while eating!
Vocalization. We have several examples of vocalization (singing, shouting, talking, grunting, etc.) causing transmission.
On March 29, we had an event at the Skagit Valley Chorale’s rehearsal in Mount Vernon, WA. Here is the report, again from the CDC: “High SARS-CoV-2 Attack Rate Following Exposure at a Choir Practice — Skagit County, Washington, March 2020“:
Following a 2.5-hour choir practice attended by 61 persons, including a symptomatic index patient, 32 confirmed and 20 probable secondary COVID-19 cases occurred (attack rate = 53.3% to 86.7%); three patients were hospitalized, and two died. Transmission was likely facilitated by close proximity (within 6 feet) during practice and augmented by the act of singing.
(Sadly, privacy concerns forbid a seat diagram.) I don’t agree that proximity in and itself transmits anything; it seems clear to me that singing was the issue (although transmission through fomites was possible, as choir members put away chairs, etc.). Supporting evidence from Missouri’s Daily Journal, “A surprising way you may risk getting Covid-19“:
The possibility that singing might help transmit infectious diseases is not a new concept. A 1968 article, “Singing and the Dissemination of Tuberculosis,” described an elaborate box that volunteers could talk, sing and cough into, allowing investigators to measure the number, size and length of time airborne of individual infectious droplets they breathed out. And a few TB outbreaks have featured singing, including one in a New Jersey church choir in 1995.
(This is good local journalism, too.) Science confirms, in “Why do some COVID-19 patients infect many others, whereas most don’t spread the virus at all?“:
Some situations may be particularly risky. Meatpacking plants are likely vulnerable because many people work closely together in spaces where low temperature helps the virus survive. But it may also be relevant that they tend to be loud places, [Gwenan Knight of the London School of Hygiene & Tropical Medicine] says. The report about the choir in Washington made her realize that one thing links numerous clusters: They happened in places where people shout or sing. And although Zumba classes have been connected to outbreaks, Pilates classes, which are not as intense, have not, Knight notes. “Maybe slow, gentle breathing is not a risk factor, but heavy, deep, or rapid breathing and shouting is.”
We also have the following case in Chicago. From the CDC, “Community Transmission of SARS-CoV-2 at Two Family Gatherings — Chicago, Illinois, February–March 2020“:
This report describes the cluster of 16 cases of confirmed or probable COVID-19, including three deaths, likely resulting from transmission of SARS-CoV-2 at two family gatherings (a funeral and a birthday party)
Here, instead of a seating diagram, we have a timeline:
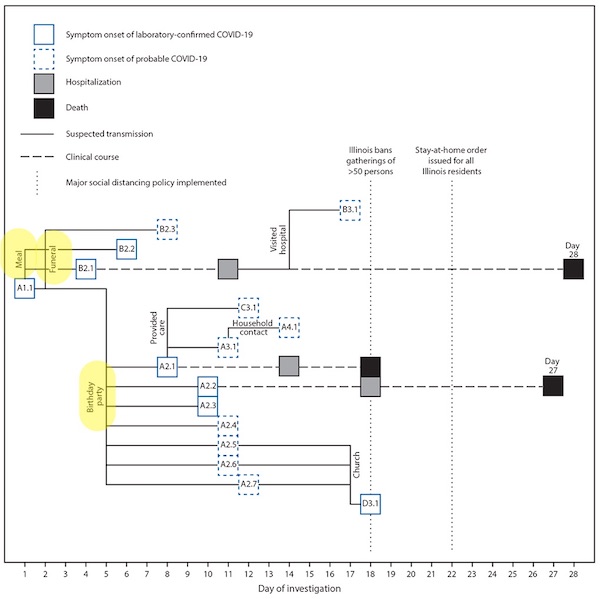
I’m guessing “Happy Birthday” was sung at the birthday party, hence the greater number of cases originating from it.
Here is the case of a South Korean call center. From the CDC, “Coronavirus Disease Outbreak in Call Center, South Korea”:
We described the epidemiologic characteristics of a COVID-19 outbreak centered in a call center in South Korea. We identified 97 confirmed COVID-19 case-patients in building X, indicating an attack rate of 8.5%. However, if we restrict our results the 11th floor, the attack rate was as high as 43.5%. This outbreak shows alarmingly that severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can be exceptionally contagious in crowded office settings such as a call center. The magnitude of the outbreak illustrates how a high-density work environment can become a high-risk site for the spread of COVID-19 and potentially a source of further transmission. Nearly all the case-patients were on one side of the building on 11th floor. Severe acute respiratory syndrome coronavirus, the predecessor of SARS-CoV-2, exhibited multiple superspreading events in 2002 and 2003, in which a few persons infected others, resulting in many secondary cases. Despite considerable interaction between workers on different floors of building X in the elevators and lobby, spread of COVID-19 was limited almost exclusively to the 11th floor, which indicates that the duration of interaction (or contact) was likely the main facilitator for further spreading of SARS-CoV-2.
Here we do have a seating diagram:

It seems unlikely to me that air conditioning was the major factor, because otherwise — HVAC mavens in the readership will correct me — the cases would have been distributed throughout the floor. However, what call center personnel do is talk, a lot. Hence I would urge that vocalization is the driver, not mere proximity.
And finally, we have the case of a South Korean gym. From the CDC, “Cluster of Coronavirus Disease Associated with Fitness Dance Classes, South Korea”
Characteristics that might have led to transmission from the instructors in Cheonan include large class sizes, small spaces, and intensity of the workouts. The moist, warm atmosphere in a sports facility coupled with turbulent air flow generated by intense physical exercise can cause more dense transmission of isolated droplets (6,7). Classes from which secondary COVID-19 cases were identified included 5–22 students in a room ≈60 m2 during 50 minutes of intense exercise. We did not identify cases among classes with <5 participants in the same space. Of note, instructor C taught Pilates and yoga for classes of 7–8 students in the same facility at the same time as instructor B (Figure; Appendix Table 2), but none of her students tested positive for the virus. We hypothesize that the lower intensity of Pilates and yoga did not cause the same transmission effects as those of the more intense fitness dance classes.
Here is a really neat map of the cases (full size version):
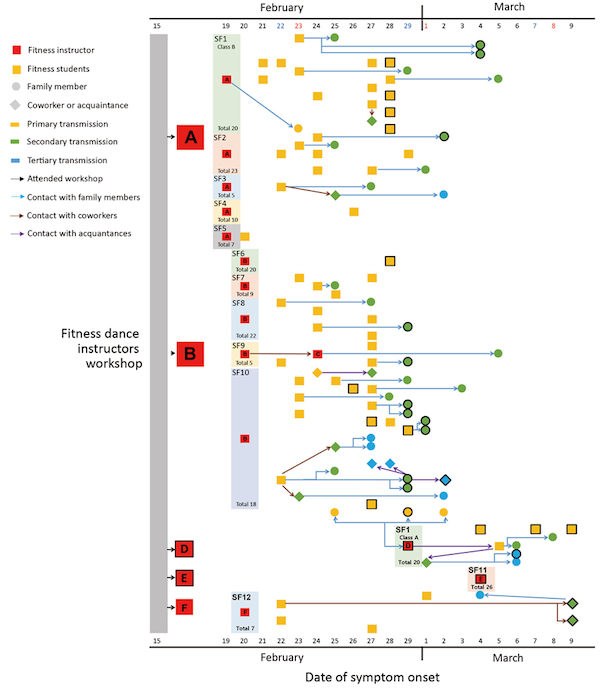
We see that “high intensity” classes accounting for all the transmission; there was no transmission from Yoga and Pilates classes. Here the vocalization would be heavy breathing, huffing and puffing.
Heuristic of Avoid Transmission of SARS-CoV-2 Indoors
One salutary result of focusing on indoor transmission of SARS-CoV-2 is that we don’t have to get all het up [4] about photos like this anymore:
The foreground/background compressed photos of people enjoying outdoor spaces are becoming an irresistible genre. This one from the Washington Post shows a few hundred people in the space of a few hundred meters. In other words, reasonable numbers. The moral panic will backfire. pic.twitter.com/MBBNNMVcXP
— Pinboard (@Pinboard) May 25, 2020
Photographer’s tricks aside, these people are outdoors; the risk is minimal (though I still won’t answer for, say, small groups of people sitting on a beach blanket, sharing beers and singing old songs). I would avoid groups like this, but then I would anyway, virus or no virus.
The Japanese seem to have had some success by focusing on indoor transmission as well, following a rule called “The Three C’s.” Here is a poster:

Bloomberg explains, in “Did Japan Just Beat the Virus Without Lockdowns or Mass Testing?“:
Experts are also credited with creating an easy-to-understand message of avoiding what are called the “Three C’s” — closed spaces, crowded spaces and close-contact settings — rather than keeping away from others entirely.
“Social distancing may work, but it doesn’t really help to continue normal social life,” said Hokkaido University’s Suzuki. “The ‘Three C’s’ are a much more pragmatic approach and very effective, while having a similar effect.”
However, I think that knowing what we know now, we can add two more almost-C’s to avoid: Air Conditioning, and “Vocalization (or perhaps Cacophony?) However, all in all, I think the best heuristic is offered by one Ángela Caída’s Twitter account:
This “Three C’s environment is the same as a crowded, musty cave full of tightly packed, chattering bats, which makes sense, because that’s where the coronavirus evolved.
Caves are also cool, like air conditioned spaces, and while bats vocalize, I doubt they transmit SARS-CoV-2 as well as we do[3].
So, to avoid SARS-CoV-2 airborne transmission, don’t be like a bat! Avoid bat caves! Also, learn sign language?
NOTES
[1] Thanks to the NC commentariat for a really useful discussion on shouting in nursing homes.
[2] There is a big debate over whether vocalization produces big and small droplets, or a continuum of droplets (with “aerosols” at the small end) but I don’t think that matters for the purposes pf this post.
[3] “Much of the cacophony in a bat cluster, the researchers suggest, is bats voicing their annoyance with those in very close quarters around them.” Bat vocalizations are “ultrasonic“, “repeated bursts of only a few hundred milliseconds.” So making the assumption that lower-pitched and longer human communication emits more virus, one might speculate that bats would be less vulnerable to airborne transmission of #COVID-19 than humans.
[4] Terry Pratchett, The Truth:
“Mrs. Tilly, I think you wrote a lovely well-spelled and grammatical letter to us suggesting that everyone under the age of eighteen should be flogged once a week to stop them being so noisy?”
“Once a day, Mr de Worde,” said Mrs. Tilly. “That’ll teach ‘em to go around being young!”


So, if you must stay in a hotel while driving interstate to avoid air travel:
– choose an older hotel with (noisy) under-window AC rather than the more efficient but potentially deadly central HVAC in newer buildings?
– minimize your (masked) time checking in; wipe down all surfaces w/ bleach esp bathroom, TV remote, table tops; shove bedcover into a drawer; decline room service if only staying one night; avoid common areas; skip breakfast entirely or at most grab and go; remote checkout?
– any other suggestions?
Ask how much they charge for having your own (inside sanitized at home) tent on their lawn.
I’m depressed —and vulnerable—enough to seriously consider bringing along a lightweight 2 person tent, and pop it up on top of the motel bed. Sleep, read, surf Internet in the tent. Another option is sleeping in an RV a campground or a WLMart parking lot.
Age and health issues mean I need to start thinking this through or spend remaining years at home.
Ugh.
A camper isn’t a bad investment. You’ll have fun with it.
Air travel is not in the same category as riding on a bus. Airplanes have HEPA filters. From an interview with an associate professor of aviation maintenance:
https://thepointsguy.com/news/airplane-air-hepa-filter/
So the risk in flying is not the air circulation. It is:
1. An unmasked person coughing, sneezing, or talking loudly, and you get their cooties before the air gets sucked into the filtration system. Everyone on a plane is supposed to be masked up but it’s not easy to enforce, given that the airlines can’t toss someone out at 39,000 feet.
2. Getting to the plane and your sear. Hard to imagine that people can stay 6 feet apart when dealing with airline security and getting on board. Passengers are now required to be masked up from TSA onward, so that can be enforced. Airport security can remove people.
3. Those bins at security! Filthy! Wear gloves for that part and remove/replace shortly afterwards.
Yes, as I understand it the issue with air travel isn’t the air circulation, but the passengers and contact surfaces. Everything is so tightly packed together its almost impossible to not touch surfaces, passengers and equipment (carts) that may or may not have been properly sanitized before you boarded and then sitting there for a couple hours or so without even inadvertently touching an eye or rubbing your nose.
And watch out for the bus was that takes you from the terminal to board the plane! I don’t know how common this is in the US but in Europe it’s standard for any carrier except the major ones. Just as the crisis was becoming public knowledge, I flew between Paris and Madrid. On the Paris side, we all got packed into a bus and then had to wait 30 minutes in the bus on the tarmac while they prepared the plane for boarding. People started yelling at the driver to let us out. Miracle if no one was already sick and bigger miracle if no one got infected.
friend flying a few weeks ago was required to remove her mask 3 times by the security people
HEPA filters are good for everything except germs.
At best case they trap viruses and they could return to the cabin.
No filter designed to deactivate viruses & bacteria,
these are other technical solutions that should come soon,
some based on UV C some on chemistry.
You are straw manning what I said. Moreover, HEPA filters are more effective than n95 masks, which are widely viewed as offering good protection versus coronavirus:
https://www.vaniman.com/do-hepa-air-purifiers-filter-out-the-covid-19-virus/
https://www.alencorp.com/blogs/articles/air-purifiers-and-coronavirus
When handling linens, such as that dirty bed cover that hotels never wash–hold them away from your body, and don’t shake them around! Hotel linens have always been an object of suspicion to me. I like to take my own pillows, too, although probably not necessary. I like the idea of wiping everything with bleach, just the same as I scrub my groceries and mail. Probably, going overboard, however, some things, just make us feel better and are harmless, so why not? All this sure takes the fun out of travel but an RV fixes the problem! At the moment, the state park we like to RV in still has closed camp grounds. The private camp grounds are open, but not very nice and more expensive, too.
If you are in the west you can park your RV or pitch your tent on BLM or National Forest land for free.
HVAC maven here:
Lambert, it really depends on how the HVAC system is configured; different zones on a particular floor may be served by different airhandlers.
Some buildings have large central A/C plants with massive airhandlers that serve the entire building, especially in 1960’s though mid 1970’s vintage high-rise office towers.
Several of NYC’s larger office REITs are considering installing UV equipment in the airhandler fan chambers, but I haven’t heard of any contracts being let just yet.
Seconding the uncertainty.
I’m not an HVAC maven; I worked in a groundwater modelling lab and have some familiarity with plume dynamics. There were some interesting air-plume studies published recently. Most have been concerned with spatial layout of rooms and pathways.
As small droplets evaporate, they become lighter and more subject to diffusion, spreading by random Brownian motion. This can be very fast; when my dog got skunked, she was in the living room for two or three seconds. Janet’s nursing bag was across the room, and when she opened it at a patient’s house, she got a solid waft. However, this does not lead to heavy viral loads (‘dilution is the solution to pollution’).
Dispersion is different, dependent on both flow speed and physical barriers. Fast enough and you’ll get turbulent mixing in open situations. Slow enough and you’ll get laminar flow even in a crowded field. Mixing, like diffusion, expands the space but decreases contaminant load.
Main image to take away, the worst place to be is downstream of a point source/infected person in a slow-moving plume. I’ll suggest the Florida spring break spread was more from bars than beaches, for example. Depending on conditions, even a well-ventilated space could put a concentrated plume right in someones face.
Thus, uncertainty. Protect yourself at all times. Wear the mask.
But Steve H., I wear my mask to protect YOU.
Thank you, good point. I’m really talking N95 masks, though the surgical masks did lessen transmission by a third, iirc. I had a couple, but am now sparing them, generally wearing a cloth mask which I spray with alcohol ;)
Masked/’Free’ is a strong signal, isn’t it? I particularly note the FU mask, N95 with a vent. The ones I’ve seen do no filtration on the exhale, but are more comfortable for the user. I hate them worse than no-mask.
> Main image to take away, the worst place to be is downstream of a point source/infected person in a slow-moving plume.
Good rule of thumb, and suggests unmasked joggers are not as dangerous as one might think, since their plume, though rich with droplets, would be fast-moving
UV equipment in the air stream is common in hospitals.
A full and fairly complete examination of HVAC systems, air flow, ventilation rates, outside air, zones, etc. is well established in the ASHRAE manuals. Now of course most folks are not interested in the technical details however the point is that there is a well established, commonly available, body of knowledge about HVAC systems, air flow, and air stream treatments which will be helpful in choosing a clear path forward in regards to air borne transmission of infectious diseases. .
By referring to the industry standard we can come to a clear understanding and establish a common path forward.
It might be worth noting that the ASHRAE standards have changed considerably from years past. In the 70s, 5 CFM per occupant of fresh air was the norm; that has changed to 15 CFM per occupant. Might also be worth noting that in most all modern buildings the amount of air filtration has greatly increased from years past.
As a final point, layout and the diffusion of air flow ( is air directed upward or downward, or is room pressurized from wall vents?) can vary greatly and would determine where it might be safer to arrange a classroom, for instance.
I have a suspicion that operable windows might have a renaissance due to this virus.
Thank you. A lot of good HVAC material in these comments.
As for the Japanese and avoiding cramped closed close contact spaces: i did not know they had shutdown subways and trains…
Also places like karaoke bars…were they closed in S Korea?
Not sure about S. Korea but most karaoke bars in Japan have been shut (not compulsary shutdown but under enormous social pressure) since the state of emergency was declared. The state of emergency was lifted yesterday but I doubt there will be many people going for karaoke for a while yet
Bars have been open in most Japanese cities more or less continually – not quite as bad as karaoke, but I’m still amazed that they haven’t been sources of outbreaks. I suspect though that there has been a lot less business for them than before. I do feel for some of the bar owners, tens of thousands of them are small, one or two person operations.
Having said all this, I have quite a few Japanese friends (mostly quite apolitical, as most Japanese are), and all have been unanimous that the government has been consistently lying about the extent of the virus in the country.
it is likely true that govts lie about this. and the extent to hide the results at some point become limited. It clearly is NOT exploding or we WOULD know about it
Since the state of emergency was declared there have been reports of up to a 60% decrease in passenger volume on the trains. This includes yours truly, who hasn’t been to the office in Shinjuku since late Feb.
Even so, 40% of normal volume is still a lot of people.
Nevertheless, even before the state of emergency was declared, the trains don’t seem to have given rise to many clusters for whatever reason. My best guess is that a lot passengers were wearing masks, and there isn’t an awful lot of conversation during peak commuter times either. March is peak hay-fever season, so a lot of people would have been wearing masks anyway, and wiht the news from Wuhan, even more so this year.
Thanks.
“Photographer’s tricks aside, these people are outdoors; the risk is minimal….”
That might be true for for deep focus shots along seaside boardwalks,
but maybe not for the overhead shots of Lake of the Ozarks resorts that we’ve all seen.
Not to mention that drunks trying to impress the other gender can get very vocal.
It will be a very long time before my nuclear family unit ventures forth.
It seems like the trick might be to stay within your nuclear unit outdoors and not mix with others. We’ll need luck trying to teach that to pool bound Arkansas high schoolers (see link below) or possibly Lake of the Ozarks revelers.
https://www.star-telegram.com/news/coronavirus/article242967096.html
I have been out mountain biking with my younger son lately. We feel pretty safe so far. The nice thing about biking in a relatively secluded place is that we literally touch nothing that isn’t “ours”. Our only debates are if we need to press a button to cross a street.
Sometimes I can use my elbow to press the button. Otherwise, I try to use a knuckle.
> Not to mention that drunks trying to impress the other gender can get very vocal.
Good point!
Shutting down churches without shutting down trains (no HEPA filters there, presumably) if their choral music is taped, not live performance, would seem selective, for those who do not believe in livin on bread alone (thus spiritual nourishment is essential).
Except if one person in the choir gets it then they transmit it to the group during rehearsal or taping. We go to church virtually these days.
Read the Bible for nourishment.
No quibbles with your conclusion re: airborne transmission, but the first study you cite above (“How Covid19 spread through a Hunan bus”) was retracted:
https://retractionwatch.com/2020/04/22/study-claiming-broader-spread-of-aerosolized-coronavirus-is-retracted/
This is apparently the retraction notice, but it is, well, Chinese to me: http://c61.cnki.net/cjfd/Withdraw/SYYY/SYYY20200304003.pdf
Annoyingly, I can’t find the original academic publication.
Dear me! Thanks for the information. Interestingly, the retraction doesn’t explain why. I’m still not going on any buses any time soon, though; the restaurant study backs this one up.
My impression at the time was that the retraction was political. (See ‘permanently disqualifying‘ for an American example.)
I thought the study was well-done, then it went away. iirc, it was the first confirmation of aerosol transmission, but there were so many unknowns at the time that true airborne would’ve been panic-inducing. But it was valuable for guidance, ie Nope don’t go there!
> My impression at the time was that the retraction was political
That was my impression. Everything in the SCMP article seemed well-founded. And yes, it was valuable for guidance.
One of my basic rules of thumb is to only go into buildings with very high ceilings (typical big box store) and low density of people. There is lots of air available then for recriculation and you should be able to avoid the virus if you generally stay away from people. I avoid all conversation with people.
By definition, this is generally not going to be a restaurant or bar, so they are out for the foreseeable future.
I like the way that this article brings together so many threads and articles over the past few months into a handy page. It looks much better when you see it all on one page and start to make your own conclusions. Of course some of the conclusions suck as in no public transport, no restaurants, no gyms, etc. Of course some people will not take note-
https://www.youtube.com/watch?v=OFl_KQGyyC4
When talking about church transmission I thought about something from history. About two centuries ago many Scots followed religions that were not exactly in line with the British Army’s professed Church of England. So to avoid getting caught at their own lay services, they would head off to a field or hill and post guards at each corner to give warning of spies and proceed in their services.
So yes, a lot of these churches could have their services in fields while the local sky-pilot could use a megaphone to give the service. They just need to space themselves out a bit. More to the point, some groups forget that their people are the church and not just the buildings that they happen to use. We have even seen services conducted over the net or in drive-in like services. I think that, for example, those people in that Mississippi church that had their church burnt down may have forgotten that fact.
No. They are waiting for the Rapture..From a NC Contributor Tom Stone, “I have no problem with individual Christians rushing to their Heavenly Rewards, it’s when they take others with them without their consent that I see an issue..”
In my comment I see that I neglected to say that it was not Scottish people that were going off to fields and hills to have their lay services but Scottish Regiments.
Yes, the people ARE the church. And the minister knows it. That’s why they want a full church and not a social distance meeting. More congregants more money in the “offering” plate. Ministers refer to their work as a calling, but we all know its a professional service.
> Yes, the people ARE the church.
That doesn’t imply that the church needs to a building. If I recall my Episcopalian theology correctly, the body of Christ is not corporeal.
The author needs a lesson in logic, specifically how to identify circular reasoning.
The referenced study analyzes “speech droplets” ASSUMING they are carrying an infectious agent.
Sometimes one refrains from stating the obvious (especially in an abstract, which is what I quoted). From the first paragraph of the study:
This is why you — I assume — cover your mouth when you cough, or cough into your elbow.
I loved the suggestion at the end of this, from slatestarcodex.com:
Our first confirmed community transmission of Covid-19 patient was believed to have acquired it at church.
I would think that much of the same thing is true in cold regions where heat is required. Especially if it’s a central heating system.
Again, it’s going to be specific to the office building in question.
Forced air heat will spread the virus, but hydronic baseboard or one pipe steam radiators not so much.
> while bats vocalize, I doubt they transmit SARS-CoV-2 as well as we do[3].
: Neuweiler, The Biology of Bats: In a human speaking at normal conversational level, subglottic pressure is equal to about 8 cm H20. The echolocation signals emitted by bats are extremely loud, reaching sound pressures of 110 dB SPL. Accordingly, … subglottic pressures of 30-45 cm H2O have been measured.
Bassists talk of ‘pushing air’ based on the power of their amp. Bat vocalizations might be quick, but they are powerful. Normal human conversation is about 60 dB, the loudest human scream was measured at 129 dB, and dB is measured on a log scale. The little critters can push serious air.
> The little critters can push serious air.
The NC commentariat is indeed the best commentariat.
U.S. Americans are loud. We open our mouths wide when we talk, we show our teeth, … we laugh a lot. We use our ‘outside voice,’ inside.
I was not aware of this until about 20 years ago, my spouse and I had been living and working in the French Alps, near the Italian border, for three months. I had commented that dining in the local restaurants (definitely not haute cuisine, as this was a gritty working class town, where the local workmen crowded into the bars for the plat du jour) was a treat; there was no background music or TV, just a low contented hum as hungry people chowed down.
At the end of the our time there, we bicycled across France to the southwest coast, near the Spanish border, to join a group of American cyclists for a three week trek through the Pyrenees, following the Tour de France. We arrived at the hotel late and exhausted. Next morning we started downstairs to join the group and my ears were assaulted by the noise level of twenty or so really really loud Americans, laughing and … well …. shouting at each other. In a way it was good; being the straggler in the group and cycling into a strange village late for lunch, I could easily find where the group was dining … just follow the loud laughter.
So, maybe this cultural tendency towards loud speech and widely opening our mouths is one of the contributors towards our higher CoVid 19 numbers. We just can’t keep our viruses to ourselves.
Much good information can be found at the web site microbe.tv podcasts, and other place lined to there. Out of Columbia University. Recent topics under discussion include transmission in choirs and particle sizes.
I am linking the following primarily because it features a photo of a hamster in a mask. An apt antidote for our time.
That Viral Mask Study Was Done on Hamsters Slate
I’m assuming the opening sentence is a reference to O’Connor; for which I thank you.
Ha! Not “Everything That Rises Must Converge,” but “All that is solid melts into air” (from The Bearded One).
marshall berman had a beard too.
A few HVAC resources:
https://www.ashrae.org/technical-resources/resources
https://www.esmagazine.com/articles/100256-a-coronavirus-conversation-with-dr-stephanie-taylor
Thanks. That second link is very useful.
Below are some follow-up links. Two points to note:
: Desiccation changes the concentration of solutes and thus chemical properties in the droplet. This seems to kill bacteria.
: With enough humidity, a tiny droplet will grow in size. This means that aerosol droplets can grow in size and drop out of the airstream. That’s important.
ncbi.nlm.nih.gov/pmc/articles/PMC5981065/
pubs.acs.org/doi/full/10.1021/acs.est.9b04959
inscc.utah.edu/~tgarrett/5200/Notes/Kohler.pdf
Lambert (or others), what do you think of hiking on a crowded trail ?
I did a 6mi round trip on a Sat in western NC. Lots of groups of people to pass or who passed me within a couple feet, talking loudly, or huffing and puffing. Lots of overhanging fauna. Humid.
I pulled my doubled-over bandana over my nose/mouth as much as I could when passing, and stood off to side if there was space.