By Lambert Strether of Corrente.
Let’s get the engineering stuff out of the way first, because masking is too important to be left to the medical community. Covid is airborne (a.k.a. aerosol transmission); people infect each other with Covid via “shared air”, which floats like cigarette smoke. Covid is airborne in hospital settings. Masks work to prevent airborne transmission[1].
Mass General Hospital (Mass General, MGH) is Harvard Medical School’s teaching hospital. MGH is ranked #8 nationally, #1 in Massachusetts. (Mass General is also part of an corporate moloch known as Mass General Brigham, which is “the dominant, tax-exempt academic hospital organization in Massachusetts with $16 billion of annual revenue“). As such, MGH is deeply interlocked with the Massachusetts political, financial, and NGO elites. As a teaching hospital, it exerts enormous influence on health care policy and practice through its network of academics, graduates, researchers, etc. I also have MGH to thank for saving my eyesight, when I had a detached retina many years ago. (MGH also spawned Rochelle Walenksy. I’m not sure if that evens out or not.)
MGH has announced it will change its masking policy on May 12 (four days from now):
With the end of the COVID-19 Public Health Emergency, @MassGenBrigham will end universal masking at all our hospitals, clinics, and other facilities starting on May 12, 2023. Learn more: https://t.co/zAuMrcnlNm pic.twitter.com/snDkTf54aN
— Mass General Cancer Center (@MGHCancerCenter) May 5, 2023
Here is some of the press coverage:
- Mask mandate ending: Mass General Hospital and Beth Israel Lahey Health to end universal masking requirements CBS;
- Masks will become optional for most hospital patients, visitors and staff WBUR
- Most major health care and hospital systems in Mass. will lift mask requirements next week Boston Globe (including MGH)
Sadly, MGH’s announcement is disingenuous, and the press coverage is wrong. Here is actual policy. And here are its two key aspects from the patient’s perspective:
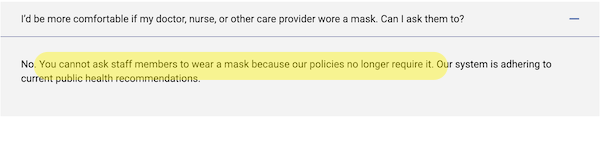
As you can see, the patient cannot even ask for staff (doctor, nurse, radiologist, anyone) to be masked; there is to be no accommodation for anyone, even the immunocompromised.
This policy is not medically justified: I mean, imagine a staffer is coughing. Patients aren’t allowed to ask them to mask?[2] Further, the policy mandates one-way masking, which permits more infection than two-way (universal). This policy is wrong for everyone, even if it endangers the immunocompromised most. Covid spreads asymptomatically; it is not possible to know if a staffer has it or not. Further, Covid is airborne and spreads like cigarette smoke; you can catch it from a cashier, or someone passing in the hall, just as well as from a doctor. Masking should be universal in the facility. Therefore, for a percentage of patients, on any given day, MGH is mandating infection.
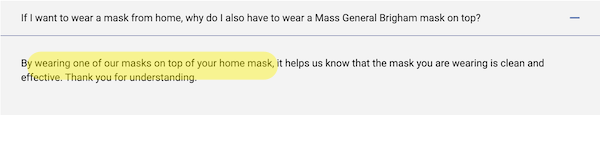
This policy is not medically justified: Double-masking wrecks fit, as MGH — in the person of Erica Shenoy, who we will meet immediately below — itself admits[3]:
It is important to note that the CDC does not recommend wearing two disposable masks or using a disposable mask over a cloth mask. Neither of these approaches improves the function of the mask in a meaningful way…. The CDC does not recommend wearing two disposable masks, as that does not improve fit. They also stress not wearing more than one KN95 mask, or a mask over a KN95.
MHG is requiring in 2023 exactly what they deprecated in 2021. Here again for a percentage of patients, on any given day, MGH is mandating infection, as we see from this telling anecdote. Shenoy doesn’t know a mask from a hole in the ground:
"If you are worried about compromising the seal you should remove your home face covering and wear the facemask provided."
i.e. I should remove my N95 and wear a surgical mask for a better seal.
I replied to both her and @ericashenoy explaining this made no sense. I was ignored
— Nurit Baytch (@NuritBaytch) April 19, 2023
How did a major teaching hospital end up mandating infection? Well, that would require more insight into the reactionary mossbacks running the institutional aspects of Hospital Infection Control than I have[4]. What I can say is the first and corresponding author of a key paper creating the permission structure for abandoning universal masking in hospitals — and the consequent addition of Covid patients to the already horrific numbers on Hospital-Acquired (nosocominal) Infection — is none other than Erica Shenoy, Medical Director of Infection Control for Mass General Brigham. First, I will look at Shenoy’s paper. Spoiler alert: It’s bad. Then, I will look at the ADA lawsuit filed against MGH: good, but not great.
The Paper
Shenoy’s paper is from the “Ideas and Opinions” section in the Annals of Internal Medicine, which KLG regards as “authoritative”: “Universal Masking in Health Care Settings: A Pandemic Strategy Whose Time Has Come and Gone, For Now” (“for now” is rich. As if these goons would ever allow masks back). The paper has in essence two reasons why universal masking should be abandoned. First, basically, “things are better now,” due to better treatments, lower mortality, “endemicity”, and so forth. Second, masks interfere with the delivery of care. I asked KLG to review the first aspect of the paper; I will review the second.
Here is the key paragraph for Shenoy’s first claim:
[T]he context and conditions of the pandemic have changed dramatically and favorably since masking requirements in health care were initially adopted… The burden of SARS-CoV-2 has been mitigated over time through access to testing, substantial population-level immunity providing durable protection against severe disease, a series of less virulent variants, and widespread availability of medical countermeasures, which in combination have resulted in decreasing infection mortality rates.
Here is a lightly edited version of KLG’s response:
This editorial is on the surface very well argued in the leading journal devoted to internal medicine. But other conclusions may rightly differ from those of the authors. They focus on “contextual factors” in the transition of mortality rates from high to moderate to lower to low during the pandemic. All well and good. But one doesn’t really know what to think of “widespread access to therapeutics.” Paxlovid? The evidence is still out on that one (I saw Paxlovid rebound in a close colleague, and it was awful) and other antivirals are still in the pipeline somewhere, one would hope…. An effective vaccine to coronaviruses is still a unicorn and likely to remain so.
As far as “improved vaccines” targeted properly to those most at risk, really? Where and what? Regarding testing, most tests are now antibody self-tests at home with no reporting requirement. Someone with a “mild” case who needs to work right now to live, is likely to be a spreader, and the case in his victims may not be mild.
While the concentration on mortality seems reasonable, this may have declined due to the culling effect of the first wave (a harsh but a reasonable assumption) and improved clinical management of a novel disease. I saw no mention of long covid or the effects of repeated infection on the health of those who get COVID-19 three, four, five, and more times. Endemic does not mean innocuous. HPV is endemic and due to this virus, I spent much of 2022 dealing with the sometimes very challenging consequences of exposure to HPV.
I guess it’s a good thing for Shenoy, then, that this is an opinion piece. Or maybe it’s just an idea, and a bad one. I really wouldn’t know what the editors had in mind. Perhaps they were doing Shenoy a favor?
Here is the key paragraph for Shenoy’s second claim. Since this is yellow wader-level, er, material, I’m going to add some letterered notes, thus “[A]”:
Maintaining masking requirements for [Health Care Personnel (HCP)] during all direct clinical encounters[A] may marginally reduce[B] the risk for transmission from HCP to patient or from patient to HCP. Those potential[C] incremental benefits, however, need to be weighed against increasingly recognized[D] costs. Masking impedes communication, a barrier that is distributed unequally across patient populations, such as those for whom English is not their preferred language and those who are hard-of-hearing and rely on lip reading and other nonverbal cues[E]. The increase in listening effort required when masks are used in clinical encounters is associated with increased cognitive load for patients and clinicians (5)[F]. Masks obscure facial expression; contribute to feelings of isolation; and negatively impact human connection, trust, and perception of empathy (6,[G] 7[H]).
Before going further, I should point out that today masking by staff is common in Asian hospital settings. Therefore, all of Shenoy’s claims are negated for almost half of humanity. If I were so-minded, I’d call out Shenoy for being Eurocentric, or colonialist, or even racist. To the detail–
[A] Shenoy — it seems hardly possible — seems not to recognize that Covid is airborne, spreads like smoke, and is present everywhere, not merely in “direct clinical encounters”; that’s why masking needs to be universal throughout the facility.
[B] Nice spin on “may marginally reduce.” But doesn’t this claim deserve a footnote? Where were the editors on that? See at engineering, the first paragraph.
[C] More spin. The benefits of masking are real and demonstrable. See again at engineering. See also this useful thread from Trisha Greenhalgh.
[D] “Increasingly recognized” by whom? When? In what publications? How on earth did the editors let a bare assertion like this pass?
[E] So make accommodations for them. Under, say, the ADA?
[F] Footnote (5) is “Face mask use in healthcare settings: effects on communication, cognition, listening effort and strategies for amelioration“, Cognitive Research: Principles and Implications (2022). N = 243, some hearing impaired, some not. Self-reported Facebook survey. Assuming all the “effects” are in fact clinically significant — I don’t — Shenoy is simply dishonest tendentious in that she erases the “strategies for amelioration” section of the paper, from which I quote:
To better understand how patients feel medical appointments could be improved, patients rated the following eight rehabilitative strategies from least helpful to what is most helpful during clinical appointments… A majority (57.5%) of patients selected written or visual instruction for themselves and/or their family members to be the most beneficial to have during their medical appointments, followed by including a family member into the appointment remotely if unable to attend by phone/video call (32.5%), microphones worn by the healthcare provider/Assistive listening technology (25%), more frequency phone/email follow-ups with your healthcare provider (20%), speech-to-text application (17.5%), longer appointment times (17.5%), additional follow-up appointments (15%), and support groups (5%).
Doesn’t all that sound like something a humane medical system should do? And isn’t it the least bit sketchy that Shenoy would rather infect patients by eliminating universal masking than — hear me out — ask doctors to speak louder or write things down?
[G] Footnote (6) is “Effect of facemasks on empathy and relational continuity: a randomised controlled trial in primary care”, BMC Family Practice (2013). N = 1030. First, the study is from Hong Kong. I would be very surprised indeed to find that HCWs in Hong Kong did not wear masks — search is completely useless on this, being contaminated by the mask wars — if only because of the lingering effects of SARS. If they do, that means they consider (as they ought) that patient safety is their primary concern. Second, “Amongst the wealth of literature analyzing non-verbal behaviour and its effect on the doctor-patient relationship, this is the first in exploring the impact of concealing facial expressions on the patient’s perception of empathy.” I absolutely deny that masks “conceal facial expression.” That’s a hypothesis, not a fact. The eyes are part of the face, and capable of communicating a full range of emotion and empathy. Third, “In this large randomized controlled trial, we found that the wearing of facemasks by doctors had little effect on patient enablement and satisfaction but had a significant and negative effect on patients’ perceptions of the doctors’ empathy.” So if the patients were satisfied when the doctor was masked, does empathy matter so much? Isn’t “patient satisfaction” a key metric for hospital administrators these days? Finally, this all boils down to “Let me see your smile.” Feh.
[H] Footnote (7) is “Morally Injurious Experiences and Emotions of Health Care Professionals During the COVID-19 Pandemic Before Vaccine Availability” JAMA (2021). To begin with, plenty of moral injury was due to there not being enough PPE, including masks, a situtation for which Hospital Infection Control is directly responsible (“I felt as though we were being ‘offered up for slaughter’ by having to stay in a COVID filled room with questionable PPE”), a moral injury Shenoy oddly omits to consider. Second, confounders: “masks and social distancing contribute to feelings of isolation. Many stated that it was stressful adapting to social distancing measures, such as having to “stand farther away from a colleague than previously” (respondent 11), not being able to see the entirety of facial expressions, or even recognizing coworkers in the hallway. The close interactions that would have bonded coworkers together are restricted, and many outlets for stress have been suspended.” Nowhere in the study are masks singled out as causing any sort of injury whatever. Third, I can only classify Shenoy whinging about the “moral injury” while establishing a policy that mandates patient infection as chutzpah. If not worse.
Finally, one cannot help but contrast the flimsiness and tendentious quality of Shenoy’s work product with the braying for RCTs that assails aerosol scientists and mask advocates. Shenoy’s work is mediocre at best; sloppy and dishonest at worst, and should form no basis for a policy change at a major teaching hospital, let alone a policy change that puts patients at risk.
Let us now turn to the lawsuit that hopes to prevent Shenoy’s dangerous bunkum from coming to pass.
The Lawsuit(s)
First, from another part of the Harvard forest, the question of liability. From “Hospitals That Ditch Masks Risk Exposure“:
Ending routine masking in hospital settings is a dangerous move. It puts patients and staff at risk for infection, and its potential long-term effects. It also exposes hospitals to the risk of liability.
Hospitals have a common law duty to act reasonably. If they unreasonably expose patients to risk, and the patients are harmed as a result, hospitals may be liable for damages. The result: patients who can show that it is probable that they were infected with COVID-19 in a hospital, and that they would not have been if the hospital had taken reasonable measures to protect them, may be able to successfully sue hospitals for damages.
Further, CDC may not be able to run interference for them:
The big question is what does it mean to act “reasonably” in a world in which COVID-19 abounds and remains a leading cause of death, including for children. Over the past century, courts have developed a variety of approaches to figuring out the bounds of reasonableness. In determining whether a precaution is “reasonable,” modern courts commonly consider the relative costs and benefits of taking that precaution. Where an individual causes harm because they fail to take a cost-justified precaution, they may be found negligent and required to pay for the damages they have caused.
Requiring masks in direct patient care settings is a prime example of a cost-justified precaution. Masking is a simple, effective, and low-cost measure that hospitals can take to substantially reduce the spread of COVID-19. And the benefits are significant in hospital settings. Hospitals concentrate people who, as reflected in the conditions that bring them to the hospital, are both more prone to infection and more likely to face serious consequences if infected. Moreover, both healthcare providers and patients are known vectors of transmission in healthcare institutions.
MGH has deep, deep pockets; $16 billion deep. I hope some clever lawyer, even now, is working out how to dig in and collect a packet. But that’s not the instant case, which is an ADA suit.
My first Patreon lawsuit — “Mass General Brigham wants a blanket ban on staff 😷 disability accommodations. I think that’s unlawful” — but never mind that. From Mathew Cortland, not actually a lawyer (but you don’t need to be one to file an ADA complaint):
In my view, filing before Monday morning is incredibly important because we are rapidly careening towards May 12th [when MGH’s new policy goes into effect[. So, while this is not the document I would have produced if I had more time, it will have to suffice.
I will now quote a great slab of text from Cortland’s complaint. MGB is Mass General Brigham, Mass General’s parent entity. Notes are omitted. Again, I have added notes thus: “[A]”:
In the context of SARS-CoV-2, masks serve two primary functions: 1) respiratory protection and 2) source control.
Respiratory protection refers to the mask filtering viral particles from the air as the mask wearer breathes in. A perfectly fitted N100 mask (also known as a “filtering facepiecerespirator”), would be expected to filter 99.97% of airborne particles. Respiratory protection, therefore, can be thought of as “my mask protecting me.”
Source control refers to the mask blocking transmission of infectious virus when the mask wearer talks, exhales, coughs, or sneezes[A]. Source control is the function whereby the mask blocks the mask wearer from spewing infectious virus in the air or onto a nearby surface[B] or person. Source control, therefore, can be thought of as “my mask protecting you.”
CDC has published a document titled “Scientific Brief: SARS-CoV-2 Transmission” which includes a key component of the scientific rational for a disabled patient asking health care staff to mask. CDC says, in relevant part, “[t]he principal mode by which people are infected with SARS-CoV-2 (the virus that causes COVID-19) is through exposure to respiratory fluids carrying infectious virus. Exposure occurs in three principal ways: (1) inhalation of very fine respiratory droplets and aerosol particles[C], (2) deposition of respiratory droplets and particles on exposed mucous membranes in the mouth, nose, or eye by direct splashes and sprays, and (3) touching mucous membranes with hands that have been soiled either directly by virus-containing respiratory fluids or indirectly by touching surfaces with virus on them.” Id.
With regard to the first mechanism, inhalation, CDC says inhalation “[r]isk of transmission is greatest within three to six feet of an infectious source where the concentration of these very fine droplets and particles is greatest[D].” Id. Even a mask that doesn’t provide complete source control, e.g. a surgical mask, will decrease the concentration of infectious very fine droplets and particles within three to six feet of an infectious source.
With regard to the second mechanism, CDC describes “deposition of virus carried in exhaled droplets and particles onto exposed mucous membranes (i.e., “splashes and sprays”, such as being coughed on)” and says that risk of deposition transmission “is likewise greatest close to an infectious source where the concentration of these exhaled droplets and particles is greatest.” Id. Even a mask that doesn’t provide complete source control, e.g. a surgical mask, will block splashes and sprays from an infectious source.
In a large health care system such as MGB, there are almost certain to be health care staff who are actively infected with COVID-19 but who are asymptomatic and unaware of that they are COVID-19 positive.
Disabled patients who are at higher risk from COVID-19 have the right to ask MGB staff to mask[E] as a reasonable modification to MGB’s staff masking policy in order to access health care provided by MGB. At least one federal district court has found that requiring mask usage can be a reasonable modification on the basis of disability. Seaman v. Virginia, 593 F. Supp. 3d 293. Instead, MGB seeks to impose a blanket ban on requests for reasonable modification on the basis of disability to its staff masking policy. MGB is doing so in violation of federal disability civil rights law.
[A] Or breathes.
[B] Fomite transmission of Covid is not supported in the literature (though China believes in it, perhaps rightly).
[C] This verbiage is CDC’s awkward attempt to reconcile droplet dogma and aerosol transmission. I don’t recall epidemiology on (2) “splashes and sprays” and (3) touching mucous membranes. The former is droplet dogma, the latter is fomite transmission.
[D] Wrong. Covid is airborne, and moves through the entire hospital facility.
[E] They do, but the limitations of the ADA approach is that it does not get us to universal masking.
I’m a little concerned that this complaint could win the battle and lose the war if (A) the abhorrence — the visceral hatred and denial — of airborne transmission shared by both CDC and Hospital Infection Control becomes enshrined in any sort of citable precedent, and (B) masking becomes, well, a “scarlet letter” for the disabled — even if they do become safer for it, as they will — but the not-yet-disabled go unprotected. At a bare minimum, everybody should be able to ask staff to mask, and double-masking would be deprecated. However, I’m a maximalist, and I think masking should be universal and a cultural norm. An ADA-centric approach, even if important tactically, cannot get us to that point.
Conclusion
Something is very, very wrong in Hospital Infection Control. From the San Jose Mercury News, “Opinion: California health care providers’ retreat from COVID masking is shameful“:
When the California Department of Public Health last month lifted mask mandates in health care settings, it didn’t even cross my mind as a physician and CEO of Roots Community Health Center to drop masks in clinics I oversee in the East Bay and San Jose.
The absence of a public health order never determined health care facility policy before, so I was shocked that several health systems dropped masks the moment they stopped being required. I did not need to be mandated to do the right thing for patients and staff at the onset of the pandemic, and the removal of a mandate did not erase my duty to protect and advocate for essential frontline workers and marginalized community members.
With the swift unmasking, I was not surprised by the COVID outbreak within about two weeks at Kaiser Permanente’s Santa Rosa Hospital and the facility’s quick return to masking. We should all be dismayed that staff and patients were allowed to be sickened despite the availability of masks to prevent the unnecessary harm.
Organized medicine’s retreat from masking is shameful. It is not data driven, and there is no experiential evidence to support the decision to de-mask. That is why hospital-issued statements fail to cite science for their policy changes. Instead, faceless committees issue platitudes about being in a “new phase” and reference available treatments.
But they paper over the very problem they are creating: In what universe is it ethically appropriate for health care institutions to infect their own patients with SARS-CoV-2 when masking so effectively reduces its spread?
That’s a very good question. Sadly, nobody in MGH’s Infection Control Department seems able to answer it. Except, I suppose, with a shrug, a sneer, and a demand to “Let me see you smile!”
NOTES
[1] There is rough hierarchy of masks according to the seal they create, starting with “Baggy Blues”, (surgical masks), through ear-loop respirators (KN95), headstrap respirators (N95, ideally fit-tested), and ending with full-on Darth Vader masks. (I’m eliding N95 and KN95 because the market has so confused them; there also many international standards). Protection should, of course, be layered, masks forming one layer.) Yes, Covid is the disease, SARS-CoV-2 is the virus. Then again, HCWs themselves say “COVID filled room” so there’s no point being tediously literal-minded.
[2] Examples of coughing and sniffling staffers who are maskless, or with a “Baggy Blue” sagging beneath their chins, are so numerous on the Twitter as to form a genre.
[3] It’s been awhile, but I would have thought we moved beyond cloth masks by March 2021. It’s also noteworthy that nowhere does MGH recommend that people use the highest quality mask, and while they write: “Patients and visitors to Mass General will be issued a single, hospital-grade medical mask. This mask has multiple layers and meets hospital standards” they very explicitly do not say these are N95-level. (So-called “hospital-grade” masks, which fit poorly, are probably optimized for droplet dogma, not airborne transmission.
[4] At this point we remember that Dr. John M. Conly, corresponding author of the infamous “fools gold-standard” Cochrane study, also made his way upward to his perch at WHO from the primordial slime of Hospital Infection Control in Alberta, Canada.


Well, that should really settle it.
Mass General Hospital intends to be a Standing Vortex of Covid Superspread.
Anyone who can possibly take their business elsewhere should do so for their own health and safety. No reason for them to be Mass General Hospital’s captive guinea pigs while that ADA lawsuit wends its leisurely way through the courts.
Maybe anyone who currently works there should get work elsewhere if they possibly can, because Covid Superspreading will naturally include the “no masks for you!” captive workforce there.
Two weeks? From the Conclusion:
Depends on how pig-headed MGH is. My bet is “mighty pig-headed.”
If only “compassionate capitalism” (via Forbes) were a thing eh? Seems to me that outside of lawsuits, the opportunity exists for some kind minded soul with ten digit pockets to usurp the infect-em-all misanthropes across a wide swath of industries, right? Can’t imagine that if someone who cares had a choice, they’d choose to go to COVIDGeneral™ instead of going to WeMaskOverHereHealthcare™. A paucity of options leaves us smack dab between the Scylla and Charybdis.
Too bad no one ran a study to determine how (in)effective masking is.
This is the newest.
https://slate.com/technology/2023/02/masks-effectiveness-cochrane-review.html
> how (in)effective masking is
There’s no “(in)” about it. Masks are effective. Check this link, provided for your reading pleasure in the first paragraph, and placed there exactly to preclude comments like this. Let’s have no false balance on the engineering side.
take my business elsewhere? like where? where are the hospitals that have not dropped mask requirements? do you know of any?
especially if you know of one in northern new england, or massachusetts or connecticut, i would very much like to know their name. thank you!
maybe some helpful citizen will start a list/wiki and post it on reddit, or someplace like that. if it can be done for consumer goods–ratings, prices, etc. etc.–surely it can be done for medical facilities. why not a list of covid-aware practitioners–ones who you don’t have to ask to put on a mask b/c their entire office is always masking? etc.
a good amount of the COVID info we DO have is thanks to citizen volunteers.
> maybe some helpful citizen will start a list/wiki and post it on reddit, or someplace like that.
As I keep saying, the Covid-aware need a Green Book, where establishments are listed that don’t encourage airborne infection.
Mass General Brigham has been taking over a lot of smaller businesses (like Leahey), they’re also notorious for hiring Moderna’s Board Member Elizabeth Nabel (twice) as CEO to get rid of anyone who didn’t want to be vaccinted. Of course, they’re also a pay-to-play player in MA.
With that said, I, and my family, moved our healthcare to New Hampshire DMC (we live on a border town). It was the best move. Same level of care, and a fraction of the cost. Now, if masking is a concern, don’t go, they haven’t required it for a while.
Out west, the guidelines for “visitors” at the institution I use are:
“Visitors will be required to wear a mask in all patient care areas.”
Does this apply to staff? My wonderful primary care physician had her N95 on last Monday and everyone in the front and back office was masked.
This am, had an 8am dental appointment to check the status of a cracked tooth. I had consulted with a dentist there last month concerning whether it would be allowable to wear a half mask and whether it would be okay to get an xray taken through clear plastic. Affirmative to both. Returned this morning to an endodontist in the same office whom I had seen before the pandemic. She and the attendant were wearing floppy surgicals. She stated she would not consent to an xray through clear plastic and seemed non-cordial. (I fashioned a very functional clear plastic bubble around my mouth with saran wrap and scotch tape that would allow insertion of the xray material) At that point, realizing I would be exiting never to return, I asked her why she was not wearing an N95 since prior to my consultation last month with another dentist I had been assured over the phone that all back office staff were required to wear N95s. She said CDC guidelines had changed. So, I left.
The institutional guidlines defer to LA County DPH guidlines:
“In addition, per the Los Angeles County Health Officer Order, workers in healthcare facilities and direct care settings are required to wear a mask when they are providing care or working in-person with patients, clients, and residents. They are also required to wear a mask in patient care areas when patients, clients, or residents are present.”
“In addition, per the Los Angeles County Health Officer Order, workers in healthcare facilities and direct care settings are required to wear a mask when they are providing care or working in-person with patients, clients, and residents. They are also required to wear a mask in patient care areas when patients, clients, or residents are present.”
http://publichealth.lacounty.gov/media/Coronavirus/docs/HOO/HOO_Masking_Healthcare_Facilities.pdf
Separately, I see that the Covid test positivity for LA County has jumped up to 6%.
Thanks for this. Since our hospital is owned by MGB, we have been dreading de-masking day. During an appointment, my doctor said he was expecting a wave of infections when they drop the mask requirement.
I wonder are hospitals looking at this as money maker?
> I wonder are hospitals looking at this as money maker?
Anything’s possible at this point, sad to say. (I would assume that any infection -> profit causal chain is obfuscated such that the class of PMC responsible for each link is insulated from guilty knowledge. That’s one reason for all the complexity in PMC social arrangements (besides the jobs guarantee aspect)).
It may be that some individuals see opportunity and have intent.
However, a positive feedback loop (hospitals as vectors for immune destruction) does not require intent. In fact, it can be a perverse consequence as seen from some particular node.
> Flows of energy develop hierarchical webs in which inflowing energies interact and are transformed by work processes into energy forms of higher quality that feedback amplifier actions, helping to maximize the power of the system — (Odum 1994, p. 251).
What’s the joke about Harvard being a hedge fund that offers classes?
I think this dropping requirements is a markering/consulting driven aim to appear friendly. We treat you like family!
yeah, like the Manson family
It’s hard to know whether we should be terrified because the people we look to for healing are indifferent toward our welfare or lost in some sort of mass delusion.
Lambert, thanks for that first paragraph whose facts you’ve established here against the tide. One can imagine a time where it would be recited as a creed against the murderous lies of those whose only concern is to keep Business As Usual hurtling toward collapse.
Re: Mass General Hospital Decrees that Patients May Not ***ASK*** Staff to Wear Masks, Even If Immunocompromised
Then I wouldn’t ask. I would DEMAND.
A man in a gurney is in a poor position to demand.
I seriously doubt this will actually happen in real life. I am deaf and read lips. So I have the opposite problem. Doctors and nurses I encountered briefly at a hospital visit for tests were very willing to pull down their masks so that I could ‘hear’ them. People (even healthcare professionals) are human and generally help you out if you ask nicely. You’ll sometime run into a hard core case, but it’s the exception. PS it was a Mass General affiliate.
> I seriously doubt this will actually happen in real life.
I think it’s obvious it will happen, because obviously MGH is completely out of control and won’t even entertain discussion (as we have seen in many, many other fields; see e.g. The Twitter Files). What happens after is the interesting question. Will an insistent “asker” be escorted from the premises?* Will the incident be filmed? And so forth.
NOTE * If any improper Boston knows where to find the three-ring binder that MGH security uses, that would be great. I would love to know their category and justification for tossing an insistent asker.
Should have just led with “some say” the Pandemic is over; That could be the entire. Shenoy opinion piece. ;)
All of this is casual murder. I like the term, because it is done so easily, without reflection or concern, or any possibility of contrition or consequence to those committing the act. If seatbelt laws were banned nationally, no one could claim with a straight face that those responsible for repeal were not culpable for the ensuing carnage. But here, this casual murder is committed for the good of the patients, for the good of society. So it is all to the good, of course.
Yet to deny that COVID is airborne, and spreads via air, is no different than denying that physics has a role in car crashes, and seatbelts mitigate the risk of an occupant being ejected from a vehicle involved in a crash. It’s just lunacy. It’s a baldfaced denial of realty.
But we have much of this among our elite, so perhaps not a shock. From Trump being a Russian asset, to Ukraine is winning, to the tech fairly will save us from climate change, to Russian blew up its own pipeline, the PMC as a class seem to be entirely detached from reality. I guess the Pandemic is just a further state of exception, where the facts of the situation do not apply.
What to do about this? I’m glad Lambert continually hammers home that SARS-COV-2 is airborne, spread via the air, and that universal masking is an essential element in a layered strategy. This no doubt is saving some lives. I only wish more could be done.
> This no doubt is saving some lives
I hope so!
I’d wanted to get a series of imaging, diagnostics & specialist visits done, before Weill-Cornell stopped masking. Didn’t quite make it. Great Cardiologist, PCP, Ultrasound tech (basically everybody I’d trusted through our first 3 infections & subsequent PASC; which they now refuse to code as anything but pre-existing, discrete conditions, mysteriously presenting as a perfect storm of long COVID symptoms, 3yrs back). Pointless to say anything litigious, but I’ve had to reschedule five pretty time sensitive appointments due to practicioners up & quitting & was just through a maskless skin cancer screening, after my unmasked replacement cardiologist lecturing me about my hippy-dippy snake-oil easily disguising damage, since results were boringly right down the middle. It’s not like anybody’s going to mention cursory or didactic visits. If you’re magically to walk out, upright?
> subsequent PASC; which they now refuse to code as anything but pre-existing, discrete conditions
Uh oh.
You could write to the hospital’s general counsel and say you are papering the record for fraudulent coding, and if this practice is not immediately stopped, your next letter will be to the insurer’s general counsel and the NY insurance regulator, or if Medicare, to Medicare. Medicare does care about coding fraud.
You could also write the Kaiser Foundation News person (rebranding of Kaiser Health News) to see if they’d do a piece, Make clear you’d go on the record if your name was disguised.
Get records of the changes in coding before you go to war.
THANK you! My partner & I had both done annual physicals (I’d inquired about stress-test, CCC & AAA imaging) ~2 months before D614.G, mid-March, 2020. ALL were very clear, aside from LPR. She’d 2 preexisting conditions. But, before IgG testing 6mo later, we’d NO positive PCR (like 2-3 million other NooYawkers. We’d magically acquired 7-9 measurable conditions, simultaneously & so did ALL healthcare workers, who’d failed to skedaddle to upstate “vacation cottages” to Zoom, try out their InstaPot, Shun & AllClad cook-wear, Peloton & stream Babylon Berlin & Giri Haji? Thank heavens I’d gotten the TTE before mRNA-1273!
I dont understand how you can have a policy forbidding asking something. Given the quasi government/non profit status, isn’t that a violation of the 1st amendment? Assuming its not, what is the hospital going to do –turn you away? 1) I believe thats illegal for public hospitals to do. 2) That would seem to be in poor financial interests of the hospital
As there doesnt appear to be any mechanism for the hospital to actually enforce this policy, it seems to be entirely designed to avoid having to respond to reasonable accomodation requests in the first place–so good for Lambert and the lawsuit for seeing and fighting this policy for what it is
> doesnt appear to be any mechanism for the hospital to actually enforce this policy
Well, they can stick their fingers in their ears and sing: “La la la, I can’t hear you!“
I seriously suggest wearing a Darth Vader mask and telling everyone LOUDLY in the waiting room how they are putting everyone at risk.
The are actually more comfortable to breath through than an N95 but pinch the face more. This is the type I use:
https://www.amazon.com/GVS-SPR644-Elastomeric-Professionals-Replaceable/dp/B095YBV2T9/ref=sr_1_10
You can get the more extreme version and really freak people out. This is the sort you use for handling nasty chemicals. Serious carpenters who have to strip paint use this type:
https://www.amazon.com/gp/product/B01ND42P1Z/ref=ppx_yo_dt_b_asin_title_o04_s00
I own both. No half measures here!
Sorry for Amazon, late so was lazy about search.
Exactly my thought. Ask loudly while mentioning that your brother-in-law the lawyer is on his way. Even better, have a bodyguard with camera at your side and your brother-in-law there.
Staff members not being obliged to wear as mask when requested is one thing, and that’s quite bad enough. But you cannot ask? How does the hospital punish the patient for asking? Refusal of service, I suppose.
> does the hospital punish the patient for asking
I suppose the patient could be escorted from the premises by security. There was a rumor on the Twitter to the effect that this was indeed MGH’s policy, but the source was a couple of bent MD’s saying that’s what they would do.
It’s also possible that the incident could go on the parient’s “permanent record,” though how they would code for it I don’t know.
The real question is how long will these doctors last themselves. By dropping protection, they themselves and their families through them will be continuously exposed to infection and potentially get sick over and over. If we are right and use of the respirator, specifically N95, provides significant protection and reduces the risk of infection, then it is only a matter of time before we see spaced out, brain-fog doctors unable to perform their duties, leading to an increase in malpractice and malpractice insurance cost — hitting them where it matters, followed by doctor shortages. Furthermore, doctors are not uniformly cavalier, repeat infection and disability should purge out the more reckless ones, leaving the survivors to change the policy on the respirator use.
Second, another profession that relies on facial expression to sell stuff is used car salesmen. If doctors were serious about “human connection, trust, and perception of empathy”, they would also take off their white coats. There is something called the white coat syndrome — this is stress and anxiety that doctors induce in patients, leading to high blood pressure. Anxiety + facial expressions of authority and domination + numerical dominance (many doctors against one patient) are used to hector vulnerable patients into accepting procedures of questionable necessity. I have experienced this and heard this from others. So, it may be that the hospitals think masking impedes their ability to sell medical procedures. But then if they go all mask-free, they may run into malpractice costs and staff shortages — eventually they find a $$$ “happy” middle.
Third, a one way N95 respirator is good enough. If someone does not want to have a mask, it is fine by me — we have freedom, I to wear it and you not to wear it. In fact, I no longer have a respirator to protect against COVID, I do it for the allergies. So, the approach is — “No, no, you don’t have to put a mask on, I have it for the allergies, I discovered during the pandemic that it is good for the allergies and keep on wearing it now that the pandemic is over for that purpose”.
A giant Darwinian filter.
If there is still Public Health as a field of study in the future, they’ll have a lot to write about. I hope that some of the guilty figures are still alive in future decades and not so brain-fogged that they are unaware of the condemnation of history.
> another profession that relies on facial expression to sell stuff is used car salesmen. If doctors were serious about “human connection, trust, and perception of empathy”, they would also take off their white coats. There is something called the white coat syndrome — this is stress and anxiety that doctors induce in patients, leading to high blood pressure. Anxiety + facial expressions of authority and domination + numerical dominance (many doctors against one patient) are used to hector vulnerable patients into accepting procedures of questionable necessity. I have experienced this and heard this from others.
Excellent points. The “Let me see your smile!” trope systematically erases all power relations.’
> one way N95 respirator is good enough. If someone does not want to have a mask, it is fine by me — we have freedom,
I disagree. The goal is to minimize the virus in the air. One way masking does not do this. Two way masking does. Everyone should work together to accomplish this (as they did in the beginning of the pandemic, in fact, before libertarian ideologues began to corrupt the discourse and the billionaires yanked the chokechains of the political class).
“We have freedom” = “The right to infect others shall not be infringed.” I don’t accept that for a moment. “Your right to swing your fist ends where my nose begins.” “Nose” being particularly appropriate for a lethal pathogen, spread in shared air, that first starts to multiply in the nasal tissues.
I am of the view that masks should have been mandated, and vaccines should not have been. A proven, low-cost, no risk, high-reward solution was systematically flouted and denigrated, while an unproven, high-cost, high risk but high profit solution was optimized for. Go figure.
I don’t care for any ism, except for realism and pragmatism. Realistically speaking trying to put a respirator on them invites them to take one off me… And I just care about going about my business, so some trade-offs need to be made, or we are risking restrictions on respirator use and/or sale… That’s all.
Our pulmonologist wore both 3M Aura 1870+ & goggles (three months back) in a clinic that (then) enforced droopy (procedure) masking & immediate PCR before any use of any shared testing equipment. The packed waiting room was a tiny, airless, dank cesspool o’ contaigen with coughing, sneezing folks, hobbling in and out of a pretty disgusting bathroom. I’m guessing all of us has encountered specialists who’s specious non sequiturs, dogmatic pontification & sneering grandiosity epitomizes brain damage?
Here’s a 2023 study finding that face masks actually don’t have an effect on perceived empathy:
https://www.semanticscholar.org/paper/Empathising-with-masked-targets%3A-limited-side-of-on-Scheibe-Grundmann/c5172945c2fbdb3edccdd647bb09d97de9237949
Perhaps it’s a clever ploy to nudge the population in the direction of more pro-active health preservation practices.
People who were old when I was young remembered being afraid to go to hospital; that was where people died. Between the CV and the drug-resistant microbes, perhaps we’re not far from a world in which hospitals are where people get sick.
I suspect that there are people in Pharma-world who are salivating over all the money to be made in long-term tumor management therapies, what with T-cell exhaustion in long COVID.
As a resident of Massachusetts, I strongly object to the categorization of Mass General as a hospital. It is primarily a land developer in the West End and a research organization. While it does perform some medical services, it’s trying to wiggle out of as many of the less profitable treatment as possible.
It’s buying up hospitals throughout eastern Massachusetts and now New Hampshire, which results in ERs closing, but no worries, Mass General will open urgent care centers instead. Only they won’t treat people who are injured or the job and many without insurance.
Mass General certainly isn’t alone (look at Brigham & Women’s), but for me it stands out more than all of the others because when it was given its charter over 200 years ago, its purpose was to treat all of the people of Massachusetts for both physical and mental health. But like many of Massachusetts’ other institutions (Harvard, MIT) it shows little concerns for the people and state that funded it and instead wants to have prominence on the world stage
> As a resident of Massachusetts, I strongly object to the categorization of Mass General as a hospital. It is primarily a land developer in the West End and a research organization. While it does perform some medical services, it’s trying to wiggle out of as many of the less profitable treatment as possible.
Excellent point!
I’d lived a needle-drop from UPMC, when they were the transplant center of the western world. We’d have more choppers overhead than Mogadishu (& about as much chance at affordable care?) We’d rent resident parking placards to HCW & stay healthy during Reagan’s Miracle, by cycling, walking, dumpster diving & eluding the po-po, trying to eek out a living (see Goodfellas?) Aside from training Iranian refugees to transplant or regrow organs for oilgarchs & play Guinea pig for very scary PhARMA firms (MoBay, Heather Bresch’s Mylan & “Chinese” fentanyl weren’t new, to us.) I’m kind of amazed, they’ve not bought up the Dawn of the Dead mall, as of yet?
Went to our small town ER yesterday. New sign on door saying masks are required again. After preliminary exam and blood draw they closed the exam room door: infection control. All were masked and approved of my N95.
Went to PCP’s to schedule follow-up. New sign on their door: masks no longer required if no symptoms.
Went across the street to pharmacy for more test kits. Out of stock, none available after 5/11
Thanks, Joe Biden!
> Went across the street to pharmacy for more test kits. Out of stock, none available after 5/11
At all?!?!?!?
I keep wondering what rich people do these days. Eg, the ones who are over 70 and need, say, a hip replacement surgery. With the mortality rate of hospital-acquired Covid being around 10% (if we generously forget about the post-accute sequelae), do they just suck it up and roll the dice?
(What about the two invariants to the basic rules of neoliberalism in this situation?
https://www.nakedcapitalism.com/2014/03/neo-liberalism-expressed-simple-rules.html)
> What about the two invariants to the basic rules of neoliberalism in this situation
I’m glad somebody looked at those two invariants. They’re important.
> do they just suck it up and roll the dice?
Concierge medicine would be my guess. Does anyone know if concierge medicine has a trade journal? I bet it’s full of information about how to make your office #DavosSafe. (Dentists already know how to do this, of course.)
Here’s an alternative point of view – a recommendation written by Dr. David Pate [formerly head of a hospital system in Idaho] recently on Twitter:
Free advice for health care workers: when your patient and their family members are wearing masks, it is most likely that they are trying to avoid getting infected, or perhaps are worried that they may be infected and trying to protect others. In either case, the courteous thing to do is simply put on a mask. Don’t ask patients if they want you to mask. Patients already get that you don’t want to or you would be wearing one. They already feel vulnerable. Don’t put them on the spot. They are likely to say no, it’s okay, even though they really wish you would mask, because they don’t want to risk upsetting or angering the person they feel dependent upon.
Dr. Pate is co-author of a book published last month: Preparing for the Next Global Outbreak: A Guide to Planning from the Schoolhouse to the White House.
And with his explanation, Dr. Pate offers a great lesson in empathy. MGH, take note: this, unlike a smile that does not reach the eyes, is the real deal.
Do we currently still think masks help with source control? As opposed to slowing spread of infection among staff by protecting the wearers.
It’s likely that a well fit N95 will reduce the amount of virions expelled into the vicinity
But many of us fail to ensure the seal…
My guess is masking by the COVID infected will reduce the amount of virus in the air but not eliminate it…
> Do we currently still think masks help with source control?
Non-woven polypropylene fiber filters on the way out, as well as on the way in, so yes. From the Journal of Occupational Hygiene (2021):
So of course we “still think” that. There’s no reason we would not have thought that, from the beginning — masking is already well-proven in industrial settings — except for propaganda and bad-faith studies by well-funded anti-mask goons, and massive resistance from closet droplet dogmatists in Hospital Infection Control*.
Of course, just as parachutes need to be properly folded, seat-belts need to actually lock, protective goggles must be worn over the eyes and not on the forehead, hands need to be washed thoroughly and not in a cursory manner, etc., etc., etc., there is a level of social engineering to masking as well. How would it be otherwise? (If the anti-masker brigade put a tenth of the effort they put into whinging about freedom into making sure that people understand that masks need to form a seal, many thousands of infections would be prevented.) So, fit matters, size matters, facial shape matters, straps v. loops matter, and the market is virtually unregulated, and 3M’s monopoly is keeping masks firmly in the stigmatizing medical appliance box, instead of allowing them to become fashion items and hence social norms. There is a post to be written about all those factors as well, which I intend to write in due course.
On fit, see “Face mask fit modifications that improve source control performance” (2022):
If we could just get the “Baggy Blue” crowd wearing “elastic braces” many infections would be prevented.** But of course, then Hospital Infection Control would have to admit that Covid is airborne through the entire facility, and not from splashes and sprays, or from “Aerosol-Generating Procedures” during surgery. This they are deeply, vehemently, tenaciously opposed to doing. I don’t even think the rationale is financial (although the effects may be); I think the opposition is to a paradigm shift (“By gawd, those aerosol engineer whippersnappers may have won the day in some journals, but they’re not telling me how to run my department, and twenty years of schooling tells me what I know is right.”
NOTES
* That’s all that “baggy blues” protect against, so what Shenoy and her ilk really believe shows in their actions.
** The “elastic brace” is a “Badger Seal” (earliest I can find at NC is July 2021).
Thanks, that helps. I asked because I remembered an FDA post saying to stop worrying about valved vs unvalved masks for that purpose. I’ve mostly been wearing valved N99’s but am running low on them so will go back to unvalved.
Nothing like fear porn on a Tuesday morning, from a neurotic poster.
No one is now wearing a mask in the Civey street anywhere around the hospital or in normal life, since no believes the fantasy flu is as dangerous as it was portrayed.
If you want to be afraid, be afraid of all the taxes you will have to pay for the rest of your life, to pay for all this nonsense with the flu.
Also, be afraid of the laws passed, that are still existant, that allow politicians to restrict your movements and behaviour, these will be used again for other “emergencies”
I’m approving this just so readers can recognize and deal with some of the usual anti-masker tropes. Of course, I can step in, but have fun!
They are determined to “reverse the conspiracy.” Works for climate change as well.
One million+ dead and massive economic dislocation, all just to teach us to obey. Makes sense to me. Not. Especially in a country where schooling, wage slavery and behavior-modifying prescription drugs are already doing a pretty good job.
We really were accused of fear-mongering; wearing KN-94 on our ancient, tiny elevator (tyring to avoid infecting our Fresh Direct friend, who’s wife was barely alive after cursory intubation (low SpO2, while Black?) We’d expressed concern about something called an airborne “pandemic” 2 days before our phones & TVs sounded an ominous “all hands report” alert & we’d had 815+ (30% unreported excess mortality). Our neighbor seemed aghast at losing her media conditioned DENIAL. Cuomo reported 17K, de Blasio: 19K of the 32K excess mortality. So, I’m wondering if the GBD/ Brownstone Institute troll has ever contemplated NEVER seeing Jeffrey Tucker in a maskless, impromptu interview or venue devoid HEPA, far UVC, MERV 13, recently PCR tested stagehands; like Rochelle, Jha, Joe & Panglossy minimizes at Atlantic, WaPo, CNN or Fox?
I never get challenged about mask wearing. Of course, they might get the vibe that I’d rip them a new asshole if they tried. You just have to learn to look Not Even Remotely Nice in circumstances like this.
I’m a 6’5″ Kraut hillbilly, who fought cranked-up red state steelworkers for 34yrs. I’ve yet to be tased, but gased & whupped by PR-24 upon numerous occasions. The replacement Cardiologist is half my age & built like a kick-boxer! It’s like elephants’ fear of mice?
The “They Live” stereotype yuppie neighbor, later admitted to being as sick as a dog, a year later, Sp02vof 86!
Proverbs 22:3 comes to mind: (NIV)
“The prudent see danger and take refuge,
but the simple keep going and pay the penalty.”
—
On the upside, “science is popping” and those of us who don’t expire prematurely of multiple Long COVID sequelae (I’m most concerned about the clotting disorders and impairment of T-cell responses to micro-tumors) can look forward to a really … interesting world. Of course, it will probably also be a more highly stratified world, and most of us who remain will be in the sub-strata.
—
I’m trying to up my game in the plants propagation department this year — got a drip irrigation system to reduce some of the burden of watering containers. This year I’m heavily emphasizing decoratives. Skill in propagating them could come in handy in future years. It might even be an income source, what with all the foreseeable funeral flower arrangements and new graves to decorate.
Cultivars that have been in the trade for a long time are usually easy to root. If they were in the trade prior to IBA, they are a good prospect for easy rooting. Always fun to make plants. Good luck.
Full disclosure: The first cuttings I took were from a plant that doesn’t root much at all(wax myrtle), and it had been sprayed with roundup the day before I took the cuttings. Needless to say zero out of 400 rooted. I realized I needed to do a bit more research.
I’ll write this knowing it is just most likely ridiculous but honestly, if I didn’t know better this policy is just part of a “Pre-Purge” in society as a whole (thinking of the Purge movies, only at this moment it’s without the overt violence).
A policy like this is just a subtle way to get rid of the weak, poor, immunocompromised, lower class workers that can’t defend themselves, you name it. All without yet the economic collapse that is to come. No need to suspend laws against murder for a 12 hour period for people to “vent”. Yet…
Again, ridiculous rant I know but think of how many science fiction, futuristic movies that have come along in the last 30 years that rather than be a warning to us have just become instruction manuals for our”leaders”?
If there were ever a better reason to take care of yourself, your loved ones, your health, get the hell out of large metropolitan areas ( maybe there are no sanctuary areas). We are on our own.
I believe that “stochastic eugenics” is the phrase you’re looking for.
Great term, stochastic eugenics. You’ve done it again, Lambert!
i dont think all that’s tinfoil, at all, Randall.
when NC turned me on to covid, circa feb 2020, a sort of pre-purge LIHOP Culling(“let it happen on purpose”) was the first thing i thought about.
second thing was “remember how our elite imported all those Nazi’s after the war?”…
lol.
and that after doing bidness with and admiring them openly before the war.
so as i was running through walmart…the only one within maybe an hundred miles with a mask on…grabbing up handsan and whatnot before the rush…i was thinking about how this could be a “kinder, gentler holocaust”, with ample room for plausible deniability…including performative incompetence, as we’ve seen.
back in my LATOC days, we ran lots of scenarios regarding methods of reducing population…given that this issue is at the very root of all the great big global problems humanity faces.
the one thing we never thjought the PTB would attempt was a pandemic…too easy to splash back on them and theirs.
oh, well.
“Kinder, gentler holocaust”
Pretty much sums it up for me and you owe me for cleaning a t-shirt as I coughed my coffee reading that one. Thanks for that chuckle ( though not really funny I suppose),and thanks Lambert for “ Stochastic Eugenics”.
Learn something new everyday.
It’s not just LIHOP. It’s gone past HIHOP all the way to MIHOP.
Now that is an opening sentence.
This is consistent with a long history pre-covid of hospital acquired infections which still today kill on average several hundred thousand per year, and complicate the recovery of many others. This is why elective surgeries need extra careful considration before choosing; the risk of harm is generally always higher than the surgeon or health care facility will ever admit pre-op.
How can a hospital outlaw free speech? They cannot outlaw patients asking for the consideration of masking. Patients are supposed to monitor doctors, nurses, staff for hand washing; patients are expected to speak up in that case. There’s always room to advocate. It’s just why, oh why, do patients have to also be advocates when we feel most sick and weak?
I don’t mean to go all rah rah, but the Hospital for Special Surgery in New York is spectacular about infection control. They do their surgeries with the surgeons not breathing the air in the OR, for instance.
But they only do orthopedic procedures, so they aren’t (normally) dealing with people expelling lots of fluids via say diarrhea, or projectile vomiting, or coughing their lungs out. Nevertheless they seem like sanitation nazis.
FWIW I brought my trusty CO2 monitor to my MD visits to the offices for MDs connected to the hospital. Readings in the 600s even in the exam rooms so very good ventilation.
I agree that HSS is exceptional. However, HSS is housed within a larger hospital complex that certainly does have much higher rates of hospital acquired infection which they would rather you never learn about. One can walk between the two areas without ever going outside or being subject to security checking. Further there is more than one way to acquire sepsis or another infection. Each and every catheter is a potential vector; infection is a very serious problem in hospitals that has yet to be solved. Many good people try, but the complexity of the issue is a problem.