Yves here. As usual with health care profiteering American style, the methods for patient gouging are complex, so this story is about more than just an egregiously priced medication.
Note that this is Kaiser Health News monthly feature provided jointly with NPR to analyze medical bills. If you have a bill you’d like to see if they will puzzle out, can submit yours here. Be sure to give the background.
By Shefali Luthra, who covers consumer issues in health care. Her work has appeared in news outlets such as The Washington Post, CNN Health and NPR.org. Originally published at Kaiser Health News
During Anne Soloviev’s semiannual visit to Braun Dermatology & Skin Cancer Center in Washington, D.C., in January, the physician assistant diagnosed fungus in two of her toenails. Soloviev is vigilant about getting skin checks, since she is at heightened risk for skin cancer, but she hadn’t complained about her toenails or even noticed a problem.
The assistant noted some unusual discoloration where the nail meets the skin. “They took a toenail clipping and said, yeah, you have a fungus,” Soloviev recalled.
So the PA called a prescription into a specialty pharmacy with mail-order services, which would send medication to Soloviev’s Capitol Hill home.
It seemed like an easy fix to an inconsequential health issue. “I did not ask how much it cost — it never crossed my mind, ever,” said Soloviev, a former French teacher, who still works part time.
Then the bill came.
Patient: Anne Soloviev, 77 on March 18, of Washington, D.C.
The Bill: $1,496.09 for Kerydin, a topical medication that treats toenail fungus. Originally produced by Anacor Pharmaceuticals Inc., it is now a product of Sandoz, a Novartis division.
When Anne Soloviev, a retiree who lives in Washington, D.C., received a prescription to treat toenail fungus, she never thought to ask how much it cost. As it turned out, she was prescribed a topical medication costing almost $1,500.
Service Provider: My Express Care Pharmacy, plus Braun Dermatology & Skin Cancer Center
The Medical Treatment: Shortly after the physician assistant phoned in the prescription to My Express Care Pharmacy, in Maryland, the pharmacy contacted Soloviev for her health insurance information.
Soloviev is covered by Medicare, Parts A and B, and has supplemental insurance through her late husband’s government health benefits that covers prescription drugs. She also has a health reimbursement account (HRA), which contains almost $1,500 pretax dollars each year to pay for uncovered medical expenses. She typically uses that pot of money to cover copays for the other medicines she takes regularly.
Kerydin, the toenail medication, arrived by overnight mail, and an automatic refill came a few weeks later. She began swabbing it on the two toenails, as directed, having been told it would take about 11 months to treat the fungus.
She thought little of it.
But when Soloviev went to her local CVS to pick up another medication — a statin that is usually paid for by her HRA — she discovered her reserve was empty.
Unbeknownst to her, Kerydin, which it turned out costs nearly $1,500 per monthly refill, had wiped out her entire reimbursement account.
 Anne Soloviev’s prescription for Kerydin, at $1,496.09 per monthly refill, wiped out her entire health reimbursement account for the year. (Courtesy of Anne Soloviev)
Anne Soloviev’s prescription for Kerydin, at $1,496.09 per monthly refill, wiped out her entire health reimbursement account for the year. (Courtesy of Anne Soloviev)
What Gives: We’re talking about mild toenail fungus. The price tag is difficult to rationalize, experts said.
“Reality check — this is $1,500 for a medicine to treat [it],” said Wendy Epstein, an associate law professor at DePaul University, who researches health care law. “That’s quite a chunk of change.”
Leslie Pott, Sandoz’s vice president of communications, explained that Kerydin is patent-protected and priced “at parity” with its one market competitor, Jublia. She also pointed out that to secure a place on an insurer’s list of approved drugs — its formulary — the drugmaker often had to offer substantial discounts to insurers and various middlemen. “We have no visibility into the extent to which these discounts are passed onto patients or payers,” she wrote in an email.
There are many prescription treatment options for toenail fungus — both older medicines in pill form and newer topical treatments such as Kerydin, said Dr. Shari Lipner, an assistant professor at Weill Cornell Medicine and director of its nail unit. The patient in this case would have been a candidate for “quite a few” of them.
Patients are likely to pay less for the pills, for which a course of treatment lasts three months, compared with the newer topical treatments, she said, adding that the pills also seem to have greater efficacy.
In its application for Food and Drug Administration approval granted in 2014, Anacor Pharmaceuticals highlighted that a yearlong treatment of Kerydin completely cured toe fungus in 6.5 percent of patients for one trial, and 9.1 percent of patients in another.
Over-the-counter treatments are also available, but there’s not much data on them, Lipner said.
Xavier Davis, Braun Dermatology & Skin Cancer Center’s practice manager, said a drug’s price tag simply isn’t a factor when prescribers recommend a course of treatment.
“When our providers are treating patients, we’re not treating them based on what the cost’s going to be. We look for what’s the best care for the patient,” Davis said. “If the patient calls and says that’s too expensive, then we’ll look for alternatives.”
Kavita Patel, a nonresident fellow at the Brookings Institution and a practicing physician, said this process contributes to the problem. “My sister’s a dermatologist, and she’ll do the same thing — she’ll prescribe and she doesn’t know. You’re getting at many layers of how [messed] up the system is, starting with the doctor doesn’t know.”
And patients often don’t see the actual price. Or they see it too late, when they’re at the pharmacy counter picking up medicines they have been told they need or in a roundabout way discover unexpected payouts.
In January, Soloviev’s insurance plan was billed the full price of Kerydin. Of that, $1,439.57 came from her HRA. The difference, $56.52, was covered by a patient-assistance program from the drug manufacturer, explained Jonathan Lee, a pharmacist for My Express Care.
In February, when Soloviev’s prescription was refilled, her plan was again billed the full drug price. But she didn’t know about that either. A manufacturer coupon was applied to cover what remained of her insurer’s $2,000 annual deductible and the $60 copay. Her insurance then kicked in to pay the difference.
Such patient-assistance programs and coupons are meant to insulate patients from cost sharing, so that they don’t feel a pinch from a drug’s price. But in this case, the drugmaker’s patient-assistance program apparently took effect only once Soloviev’s HRA has been wiped out, allowing the manufacturer to maximize revenue from both patient and insurer.
DePaul University’s Epstein said it took her “15 minutes to figure out what was going on” here. And, unlike the average patient, she studies this issue for a living.
Lee, the pharmacist, said even he didn’t realize that money could be withdrawn directly from a patient’s HRA without her knowledge, and he’s been in the business for the better part of a decade.
None of that is consolation for Soloviev, who said: “I just find it is outrageous for a fungal medicine to cost $1,400, to be prescribed for 11 months, and for neither the PA nor the pharmacy to warn you,” Soloviev said.
Resolution: Though she has told My Express Care not to renew the prescription, Soloviev’s HRA is depleted. For the rest of the year, she’ll have to pay out-of-pocket costs for any other medications, an expense she hadn’t planned on.
The Takeaway: For even the most informed of patients, getting a new prescription can mean walking through a financial minefield. And Soloviev hit a number of booby traps.
Bottom line, experts say, medical professionals should make the patient aware if they prescribe a high-priced medicine and explain why it’s beneficial.
Patients should play defense and ask their physicians about the cost of every new prescription. They should ask again at the pharmacy — even if that means calling a mail-order pharmacy. Because costs can vary depending on each patient’s coverage, they may need to contact their insurance carrier or the PBM that handles their medicine claims.
And if the cost is extremely high, they should ask their doctor about generic or over-the-counter alternatives.
“This is an important component of the decision a patient’s going to make,” Epstein said. “If it’s toenail fungus and not life-or-death, it strikes me … an individual might want to have relevant data.”


shameful.
Shame is a 20th century concept ill-suited to this modern post-tobacco settlement world. Where some saw a consumer victory after decades of warnings on packs by getting big tobacco to acknowledge risks, others saw methodology victory for the neo-liberal machine, and an instruction manual.
Like the Big C, cancer, that machine keeps rolling along. Now it is mainstream, to be emulated instead of castigated. At least that is what appears to have happened among those shame-free star pupils of Big Pharma and their fellow travelers in FIRE, aided and abetted on the Big Screen where deviancy got defined down so far it got erased. Political and economic trends ebb and flow, with some elements of populism appearing on the horizon. Greater awareness of the plight of one’s fellow humans may help focus the mind.
Bottom line, it’s doctors and patients fault for not defending themselves against the ludicrously corrupt health insurance industry. Bottom line, medical professionals and patients have to spend their time and effort (increasingly dwindling, because markets) to try to avoid being charged a month’s pay for a tube of ointment. Because, bottom line, changing the system is not an option, so keep banging your head against that wall!
Yeah, try getting a straight answer on what this stuff will cost BEFORE you take possession, er…, are treated. “$200” has turned into $1000 bills from a third party device company that magically turns to $0 after 3 months of emails and phone calls. I’ve walked out of hospitals after getting full disclosure of costs minutes before a procedure that was scheduled weeks in advance.
The neolib corruption numbness has to seep through the cartilage into the bones to call these practices anything but criminal.
There is really no excuse for the crooks in the medical (health care? nah!) industrial complex not to provide costs of any procedure or service ahead of time. I admire you for walking out minutes before the procedure and more people should do the same. I would do the same and have.
If there’s no “Price Discovery”, is it really a “Marketplace”?
towards the end of my six and a half year slog through the disability process(sic), I learned about Cuba. I got a price for a new hip pretty easily from them(around 10 grand, including a “bungalo on the beach with a private nurse for recovery”)
so I called the nearest hospital, and asked what a new hip would cost me, cash money, walking in the door.
The person obviously didn’t understand the question, and after some time of me waving my arms and trying to word the question in a form she would understand…she said” oh…insurance takes care of that…and it depends on many factors”
“such as?” sez I
Her:” like what kind of replacement they use…which is up to the surgeon…and many things”
This went on and on, and I finally got her not nailed down at around 300 grand.
Then I asked her what medicare would pay for the same thing and she hung up on me.
It ain’t a “Market”, it’s a Racket.
(and, about the toenail fungus…my grandmother would tell her to just pee on it….)
By the “logic” of the guest post, bottom line is it’s that baby’s fault for not being strong enough to defend itself against the big kid who took its candy. It’s the woman’s fault for dressing that way before she was raped. The victims should be blamed because they didn’t play defence well enough against the criminals who write the rules of the system. I presume your comment is to flesh out the BS justification from the article, Gandhi, not to endorse it. Excuses like the one capping the guest post, instead of rabid outrage, are part of what allows the crimes to continue. I can see why so many Merkins want to burn the (family blog)er down, even though they wind up voting for Trump as a means of expressing that feeling.
Seriously, who are these ‘experts’!?!? Between the ‘experts’, who blame the victims, kick cans down the road and pass the bucks to the lay-people (no one is an expert in everything, i.e. everyone is ignorant about something at some point in their lives) they’re suppose to be advising whenever ‘expertise’ is required, and the ‘journalists’ who give them a venue to spew their apocryphal twaddle in an attempt to portray themselves as ‘experts’ when their true intentions are to gaslight, obfuscate and divide common sense and decency. Throw in the politicians, crony capitalists and all the other puppet masters and you have the perfect storm so many Americans, like myself, finds themselves drowning in. Once upon a time expertise inferred wisdom. Those days are history.
I don’t know if it works but I’ve been told that petroleum jelly will cure toenail fungus. it seems salves or topical medicines are usually expensive. I use a salve that I apply to the rash from my. Eczema. I have used it for years and the price is constantly increasing. When I started using it the cost was $50 per tube.The last tube I got cost $480. I was prescribed an inhaler for Bronchitis. It cost almost $500 and didn’t seem to do much to relieve the symptoms. fortunately my insurance payed for the medicine. It still makes me mad when I think about what was charged for these prescriptions.
There are much cheaper alternatives to inhalers for asthma or bronchitis. Buy a “Nebulizer” (we just bought a portable one for $50), which is a vaporiser, and get your doctor to prescribe “nebules” of albuterol sulphate and/or sodium chromalyn to load into the nebulizer. We get a prescription refill of nebules for $3.49 v. over $50 for a ventolin inhaler . And there is no propellant in the nebulizer which there is on an inhaler.
The greed and parasitism of the pharmaceutical cartel is criminal.
My gp told me to use Vick’s VapoRub for my toenail fungus. I asked the pharmacist and she said it has about a 10% success rate, same as the petroleum jelly from which Vick’s is made. There was some branded treatment, $40 for a 2ml bottle that she said worked maybe 15% of the time. Only been a few weeks, but so far I haven’t seen much of a change.
Yes, I used Vick’s Vaporub on a toe fungus and it worked. I was told it wouldn’t work.
The People’s Pharmacy has a lot of information on toenail fungus and also has an article recommending treatment with mentholatum.
I now go to their website before filling any prescription I’m given by a doctor.
I did (after trying other topical but non-prescription products) and it didn’t initially.
But then I used it in conjunction with a lotion with a lot of hyaluronic acid in it. Hyaluronic acid is widely used in cosmetic products to increase penetration of the active ingredients into the skin.
Worked great.
Just by sure to apply any treatment to the cuticle, particularly at the root of the nail. That is where the fungus lives.
It is a fungus, so being outside in the sun wearing flip flops might kill it.
Last summer I had toenail fungus and researched how to treat it. Soaked my feet is diluted vinegar a few days and scrubbed the area. Then I used https://www.cvs.com/drug/miconazole. It worked. Next time I have an annual checkup I will talk to my nurse practitioner. Web MD was a big help. https://www.webmd.com/skin-problems-and-treatments/guide/fungal-nail-infections-topic-overview#1
So was Mayo clinic
https://www.mayoclinic.org/diseases-conditions/nail-fungus/diagnosis-treatment/drc-20353300
I am not recommending websites replace physicians, but apparently it is necessary to always second guess the physicians.
My treatment cost less than $10.
How about requiring every provider to give a firm quotation on every product and service? Every other industry has to live with this constraint.
I’m amazed this simple idea never gets traction. Car mechanics, e.g., are required by law to provide a written estimate before work begins; if something is found that will change the estimate, they have to get your OK. Car repairs are usually much cheaper than medical bills and are often equally or more opaque to diagnose.
Having doctors and medical offices provide you with an estimate after diagnosis but before treatment does not seem like it would be terribly hard. They (uniquely) have visibility into your insurance arrangements, their reimbursement rates, their costs, overhead, profit rates, and so on. Software for this purpose would make pretty short work of boiling this down to the out-of-pocket for the patient. The patient could then either OK it, negotiate other options, or decide to shop around. If the provider later tries to charge more, the patient would have something on paper to justify refusing it.
There’s no reason patients should be treated like a bottomless bank account by the medical industry.
Many doctors have no clue what things cost. I received a single shot of cortisone for an arthritic shoulder and was charged $200. When I complained to the health care system, I was told that, had I been insured, the cost to me would be $100 less. When I complained to my doctor, he had no idea about any of this.
P.S. I knew the owner of an herb farm who had foot fungus. She visited a podiatrist and was prescribed some expensive salve which didn’t work. The woman then went out on her farm, gathered some herbs according to an old remedy, made her own salve and was cured.
I was told to get the shot for shoulder pain (was a bad idea from this quacK). The “doctor” had no idea what it would cost!! At any rate it cost me over a $100 even with Kaiser coverage and it did NOT help. It hurt a lot for a few days (in more ways than one). What a fraud this industry is.
I dread the day I’d have to go to the hospital where I it was such an emergency that I’d be at the mercy of this robber baron system
Had any car or truck repair work done lately? Or speaking of things automotive, have any of us had experiences with the sales machinery of car and truck dealers, new or used? Speaking of transparency in pricing, firm quotes and all that? As just one example of how The Machine actually works? Catch-22: “They can do anything to us they want that we can’t keep them from doing.” http://www.slate.com/articles/life/the_spectator/2011/08/seeing_catch22_twice.html
Big ones twice in the past four years on the RAV4. 2 different shops, in different states. They both gave me firm, up front price quotes. One was wrong on the low side, and the owner called me with the real price and an apology before doing the work. Just like the law requires.
This kind of fair dealing and respect for the customer never happens in medical practices. The doctors rarely soil their highly educated minds with matters of cost; everyone else in the office has little authority, and the chubby young women who sit up front in scrubs do as little as possible for the captives they call patients.
“This kind of fair dealing and respect for the customer never happens in medical practices. ”
This! And stress over billing affects health!
it is stressful and aggravating that doctors can’t/won’t address cost at the point of service. This destroys patient’s trust in the physician as well.
Therapeutic relationship is wrecked as well as health and personal finances.
This NYS law applies to services, not drugs. It’s a start:
Emergency Medical Services and Surprise Bills Law – New York State …
https://www.health.ny.gov/regulations/…bill…/ems_and_surprise_bills_law_faq.htm
If they do not participate in a patient’s health care plan, they must upon request from a patient inform the patient of the estimated amount they will bill absent unforeseen medical circumstances that may arise. Under subdivisions (3) and (4), physicians in private practice also must provide information regarding any other ..
“We’re talking about mild toenail fungus. The price tag is difficult to rationalize, experts (and every breathing human) said.”
What kind of “expert” tries to rationalize cost of prescription on severity, rather than, say, cost of making the product?
16,500 for the course of an eleven month treatment with 6 percent chance of working. Seems like a medical RX vacation almost anywhere else in the world would be prudent.
What kind of expert, you ask?
Today’s fast-paced, stimulating world in pharmaceutical revenue management and marketing needs H1-B visa assistance to hire the kind of expert that is not available in sufficient quantity or quality to allow efficient pursuit of medical excellence. In past years, such personnel were to be found only in select industries such as tobacco and other personal care products. Building the right team, with applicable key performance indicators and mission-critical elements, is too important to be left to chance so every avenue must be explored, every base touched. Consumer options are opened up in the free market of healthy competition for products rather than stifled under excess regulatory and legal layers.
That kind of expert. /s
I really enjoyed that!
Man oh man!!!!
Had a deja vu moment there — thought I was back as an employee during a leveraged buyout by the typically sleazy PE firm of Baird Private Equity!!!!!
Sounds like Soloviev wasn’t a “smart shopper”!
Teatree oil, anti fungal. >$3.00. They only have a license to practice.
Just be careful with the natural stuff…
“The results of our laboratory studies confirm that pure lavender and tea tree oils can mimic the actions of estrogens and inhibit the effects of androgens,” said Korach. “This combinatorial activity makes them somewhat unique as endocrine disruptors.”
https://www.nih.gov/news-events/news-releases/lavender-tea-tree-oils-may-cause-breast-growth-boys
My wife is a massage therapist and dispenses oils occasionally. NEVER use straight oils – ALWAYS use a carrier oil in conjunction.
BTW – anyone else notice the toe fungus ad placed above the comments…we’re being watched!
Another myth propagated by the hand maidens to the Pharma industry.
The title of the post is a bit misleading.
It should have been “Bill Of The Month: For Toenail Fungus, A $16,500 Prescription and less than 10% effective”.
. . . She began swabbing it on the two toenails, as directed, having been told it would take about 11 months to treat the fungus.
– – – –
Unbeknownst to her, Kerydin, which it turned out costs nearly $1,500 per monthly refill . . .
– – – –
In its application for Food and Drug Administration approval granted in 2014, Anacor Pharmaceuticals highlighted that a yearlong treatment of Kerydin completely cured toe fungus in 6.5 percent of patients for one trial, and 9.1 percent of patients in another.
The post’s title diminishes the scale of the scam by a factor of at least 100.
Very well articulated and thought out!
Props and kudos!!!
That last bit blew my mind. Why in the hell is the FDA approving anything as a treatment that can only be shown to cure what it’s supposed to less than 10% of the time!?!? And we know how the approval process scam works – the companies only submit the best results in the first place and leave out the data the shows treatments to be less successful.
That being said, who would like to try out my new wonder drug? It cures absolutely everything that ails you at least 5% ot the time. I call it Plaisibeaux – the ingredients are French and they’re a trade secret. Any FDA employess around who can fast track this one for me?
A 5% cure rate: with some illnesses wouldn’t that be roughly the success rate for placebos in blind drug testing ? I dont know, except that some illnesses/patients can respond to placebos.
Regardless, let’s bring on the snake-oil sales-persons…oh, I guess, that’s really just Big Pharma. Silly me, they don’t need encouragement!
Good point. Placebo rates are way high for lots of drugs, starting with anti-depressants.
My simple stupid solution just avoid them entirely, the docs the tests the meds the hospitals. Advil is cheap and works for most of the pain. A couple of other basic meds for occasional random stuff that I buy when I travel outside the US. Try to work out a bit and eat more or less right. Except for easy obvious stuff I never met anyone that actually got better by going to a doctor. When its time to die I guess I will die.
X1000
Couldn’t agree more.
+1
In our healthcare system (and I guess totally), when you’re healthy you’re wealthy!
It’s really worse than the article suggests. Kerydin (tavaborole) isn’t even all that effective. In one trial, “cure” was achieved in about 7% of cases and in other trials “completely or almost clear nail rates” were achieved in 15 – 30% of cases:
In clinical trials, tavaborole was more effective than the vehicle (ethyl acetate and propylene glycol) alone in curing onychomycosis. In two studies, fungal infection was eliminated using tavaborole in 6.5% of the cases vs. 0.5% using the vehicle alone, and 27.5% vs. 14.6% using the vehicle alone.
https://en.wikipedia.org/wiki/Tavaborole#Therapeutic_trials
For those interested, this is the original paper that the Wikipedia entry is based on:
https://www.sciencedirect.com/science/article/pii/S0190962215015121
Last visit was a snake bite. Antivenom was about 60k. Pretty sure same can be had in Mexico for less than $1,000, maybe much less. That was 5 years ago. I refuse to participate any longer, & I have good insurance. I hope eating better, exercise, & homeopathic treatments can work for me. Have not seen a doctor since & won’t unless taken unconscious.
Agree with you. Eat healthy foods, exercise, homeopathic or ayurvedic treatment when absolutely necessary. No need to go for their “free” physicals. Listen to your body.
I wouldn’t try using homeopathic stuff for snake bites, because you may end up dead. Homeopathy doesn’t work in any meaningful sense, it’s more a case of ‘take this and wait for your self-limiting condition to resolve’.
If you don’t have a self-limiting condition – i.e. you have cancer, a heart condition, a serious infection, or whatever – it’ll do precisely nothing. Believe me, I know all about ‘toughing it out’ in the face of illness, and it landed me in intensive care with acute kidney failure.
And doing the diet and exercise thing is great, but it is postponing the onset of ill-health. It’s an unfortunate part of the human condition that age will catch up with you eventually, no matter what you do.
So a physicians assistant diagnosed a fungus strictly on observation, calls in a prescription for an ineffective and more difficult to use but massively expensive prescription and it is the patient’s fault.
Don’t know about the rest of you, but I see at least three problems in that that have nothing to do with the patient OR even the obscene greed of the pharmaceutical industry but a whole lot with the Braun Dermotological Center.
I have no proof, but my guess is that these medical centers have sweetheart deals with mail-order pharmacies for various overpriced drugs. We took my son to a dermatology place several times for acne treatment; they would commonly propose something I had never heard of and urge us to order from a particular mail-order pharmacy, often providing coupons. I saw no reason not to get it from our local pharmacy but they were strangely insistent on us doing it by mail.
One obvious problem with mail-order pharmacies is made clear in this piece: by the time you find out how much things cost, it’s already a done deal. At a retail pharmacy, you can walk away without paying. This is obviously a feature of mail-order pharmacies, not a bug.
The proliferation of specialty medical centers around the western Chicago suburbs has been amazing to witness – similar to the proliferation in the number of bank outlets prior to the crash…
No kidding. How is prescribing a drug, even a cheap one, that’s “effective” only 7% of the time even considered medical “treatment?”
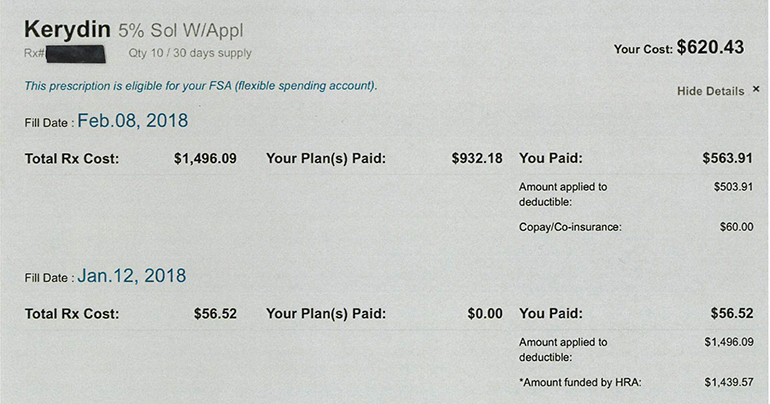
And what in the world is that “statement” pictured above? It’s flat out false. Is it somehow supposed to be official? Where did it come from?
“Total Rx cost” in January: $56.52???? No, it was $1,496.09–same as in February.
“You paid” (Patient paid?) in January: $56.52? No, the patient paid $1,439.57, “funded” through her HRA and shown with an asterisk at the bottom. $56.52 was apparently a drug company rebate / coupon.
About the only true thing in January was that the insurance paid $0.
The “You paid” in February was not, in fact paid by the patient, but by another drug company rebate / coupon. She was not even asked to write a check for the copay, an expense she would have expected.
The “Your Cost” of $620.43 at the top appears to be the sum of the two drug company coupons for January and February, although no time frame is specified. At this point, the patient had written NO checks, even for the copays.
As an aside, where is the $60 “Copay/Co-insurance for January?
The patient’s actual “cost” over the two months would most accurately be represented as the sum of the two months’ Rxs–about $3000–plus two $60 copays. “You Paid” should be what she actually paid, either out of pocket or through the HRA, and any fees or copays that were covered by drug company rebates should be clearly noted as CHARGED but ABROGATED.
I’d suggest that deliberately confusing and understating seemingly obvious terms such as “cost” and “paid”
deliberately obfuscates the situation in order to sell expensive drugs that people would balk at purchasing if they knew the true “cost.”
And all of this is before figuring out, for a Medicare recipient, how all these worthless, expensive drugs, coupons and rebates propel the patient toward the “donut hole,” an entirely different kettle of fish in which nobody pays for nuthin’ except the patient.
+1 These “statements” web pages or whatever are designed by either morons or sadistic fiends. Probably the same ones that design cell phone bills
This reminds me of the time I was billed $300 for a foot splint by a podiatrist that my insurance refused to pay for. I could have bought a foot splint off Amazon for $30.
Always ask for prices for any treatments or medicines. I trust my dentist way more than any doctor I’ve been too.
this stuff is free in france for anyone with a social security number
Kerydin has not been approved by the European Medicines Agency. You shouldn’t state things as fact unless you can back them up.
I’m sure he meant “medicine that fixes toe fungi” is free in France, not Kerydin. And of course Kerydin isn’t approved in Europe, with a 7% efficacy rate, it’s doesn’t really have medicinal value. It would only be prescribed in the US.
Stories such as this are infuriating.
I went to a Podiatrist a couple years ago for a different problem but mentioned I thought I had a toenail fungus, too.
The Dr confirmed that but instead of prescribing something he recommended coconut oil. He said it worked much better & faster than any pills he could prescribe & he was right.
I had a large jar of solid coconut oil (around $6) & applied it with a Q tip.
In very short time the fungus was gone.
A girlfriend had gone to her Dr who prescribed pills.
Her fungus returned within a few months.
Mine hasn’t.
This is not surprising – before I read your post I was thinking, there is probably a simple home remedy for that condition. There are a lot of useful drugs out there, but there are probably just as many that are useless, ineffective, or that have dangerous side effects and unintended consequences. I took over-the-counter anti-allergy meds for my hay fever for years, only recently reading that they (Claritin, etc) are now implicated in the onset of Alzheimer’s. Thanks a lot…
I caught a similar prescription with a high co-pay and refused to pick up the merch from the pharmacist.
I then treated my fungus with Lamisil an OTC product which works for me.
I was written a script for a tube of cream that supposedly cost nearly $3k. It’s hard to know what the pharmacy benefit manager actually paid because they are pretty secretive about that sort of thing. Per a friend she estimated it at probably $50 which is still idiotic. It was an anti-itch cream and wasn’t any better than a $2.50 tube of cortisone cream.
For the love of Pete. Isopropyl alcohol costs $1.79. Cut your toenails then apply with q tip. No more nail fungus. One bottle = many years supply.
I’m amazed people will take pills to cure nail fungus. So Dumb.
$14.000 annual toe cream. Dumb dumb dumber.
Thanks for posting these absurd bills. It lays bare the financialized health care holocaust underway in the USA.
Toenail fungus? Get apple cider vinegar.
Why do people not first look at home remedies?
Apple cider vinegar clears that up in a snap.
“Why do people not first look at home remedies?”
Good question.
Why will people spend $ 20 on an automatic car-wash when they could often do it at home in 20 minutes and at 10 % of the cost ?
Why spend $ 5 on a Vitamin B/C drink when a multi-vitamin from a bulk bottle would cost 10% of that? I’m sure we could add 1000’s of other examples.
So why?
Not enough time ? Lot’s of spare money? No fore-thought ? A sense that mass produced “products” must be better ?
Simply NO idea that an entire universe of things exist outside of “worldly” goods? A literal discomfort, even unconscious fear of acting outside of the usual, everyday system of exchange?
(Incidentally couldn’t agree with you more about apple cider vinegar. Wonderful stuff. I find it excellent for dealing with chest infections — ie place vinegar into pan, dilute as needed, bring to a low simmer, breathe in vapours. (Garlic, organic or in capsule form, is great, too). Not that I would suggest that one not contact a doctor, if the infection is truly bad — use vinegar in conjunction with antibiotics, if so prescribed.)
Fungus can be treated by soaking in a 25% solution of vinegar, twice a day for two weeks.
Change the pH, kill the fungus.
That was my prescription for a fungus on my foot, by my doctor. And it worked.
I pay less for my medicines when I pay cash as the pharmacy gives me a discount. But, because Part D has a penalty for not enrolling, I use it for 5 of medicines and then pay cash for one of them and pay about $5 more per month. Not to mention my doctor offered to do my stints for half price if I paid for cash. The whole healthcare system is a mess.
I don’t know about other countries, but here in the U.S. you should always, always, always assume that in any transaction you engage in, the seller has been financialized and will actively try to squeeze more money out of you, the ideal being to take all your available money and give you nothing in return. Be wary.
There are plenty of honorable exceptions, like the honest doctors and the mechanics described above. Cherish those sellers, patronize them, spread the word of mouth, especially if you think capitalism is the best of all possible economic worlds. The rent-seekers, if they continue unchecked, will destroy capitalism, because it requires some minimum level of trust to work. The odds that the seller will provide a good product or service have to be at least better than even.
Philia is a necessary casualty of identity politics. Society depends on the collective will of people to take actions that are not in their direct benefit because they know others will make them. The “Tragedy of the Commons” does not occur when philia is strong because people know they can trust others not to abuse common resources. Once people do not trust others to act for the greater good it is a race to the bottom. The problem with identity politics is that it creates distrust of others outside ones own identity group as ‘others’ who cannot be trusted.
oh yes identity politics created that, as if there wasn’t far stronger prejudice by dominant groups long before identity politics was even a glimmer in it’s dad’s eye.
Ten years ago or so in Corte Madera California, I was very lucky to find a podiatrist who was doing research on toenail fungus. I had nine of ten toe nails involved, some since high school (so for decades). His protocol for this was
1) pulse dose of two Lamasil tablets at the start of treatment
2) OTC bottle of fungoid tincture (with little brush built into the cap) from drug store with half a Lamasil tablet dissolved in it
3) every morning in the shower, scrub the nail ends with a toothbrush and a chlorine powder cleaner like Comet
4) brush a small amount fungoid tincture onto nail ends after morning shower and at night before bed.
5) keep nails short with clean cut ends
As I recall, the Lamasil pulse dose kills the fungus in the nail bed right away, and the fungoid tincture wicks into the nail every time and carries the anti-fungal drug to the fungus residing within the nail. The chlorine cleaner acts as a dessicant and pH modifier.
Ultimately, he gave me the few necessary Lamasil tablets as free samples, and back then the fungoid tincture was maybe $4/bottle at walgreens.
The new nails grew in from the nail beds perfectly, and after many months I had perfect toe nails and ceased treating them. They have remained so ever since.
I have always wondered if this approach was ever published in a medical journal. No significant money to be made from it by the manufacturer of Lamasil, so it’s hard to see who had an incentive to promote it.
Disclaimer: I am not a doctor and am not giving medical advice. Pursue at your own risk.
Thanks!!
Why your pharmacist can’t tell you….
WASHINGTON — As consumers face rapidly rising drug costs, states across the country are moving to block “gag clauses” that prohibit pharmacists from telling customers that they could save money by paying cash for prescription drugs rather than using their health insurance… The pharmacist cannot volunteer the fact that a medicine is less expensive if you pay the cash price and we don’t run it through your health plan.”
The White House Council of Economic Advisers said in a report this month that large pharmacy benefit managers “exercise undue market power” and generate “outsized profits for themselves.”
I’m going to get in trouble for saying this but toenail fungus isn’t exactly leprosy. I’ve had a case continuously for 40 years after damaging my toenails in an accident. About 20 years ago I went to a doctor to see what could be done to get rid of it. He said I can give you a prescription that may cure it . But would you rather risk your liver or take the fungus with you to the grave after a full and healthy life with the fungus. I dont know what it would have cost because I chose the fungus. If it had cost $1500 and he hadn’t told me the cost I would have been most unhappy.
This is shameful and absurd. However, the article mentions that there are “pills” that can be prescribed to treat the toe fungus, but some people taking those pills (terbinafine aka lamisil) have developed severe liver damage leading to liver transplant or death.
How much does it cost to just remove the toenail?
Why does this prescription cost $1,650 per month and not $16,500? Or $165,000? Or $1,650,000? Who decided that $1,650 was reasonable and $1,650,000 wasn’t?
Oops, I meant $1,500 per month. But it probably costs more now anyway.
And how do they make an ointment last only a month? I’ve got some ointments under my sink that are 30 years old.
I’m a lawyer. I took Contracts 25 years ago in law school, but I seem to remember that there are certain elements to a contract that have to be present before the parties can be bound. Let’s see…
1. Offer
2. Acceptance
3. Consideration
4. Mutuality
Now, it seems to me that Consideration can’t just be left blank. It is a very rare (non-medical) contract indeed where the buyer says, “I want X, no matter what it costs.”
If I stay at a hotel and they have a mini-fridge with various refreshments and snacks, and I take a Diet Coke and a Milky Way, they can’t legally charge me $10,000 for that.
I don’t know why this isn’t considered defrauding the consumer. We should be able to sue the crap out of these companies.
Give the medical practitioners a break! So now they need to puruse the Wall St Journal daily to see what pirate has acquired what formerly cheap generic drup to monopolize it and raise the price 500%?
Yes, the price was outrageous. How is the practitioner supposed to know every patients health care coverage and what one particular insurance carrier will cover for what drug? What’s $50 for one person is $1500 for another, depending on their insurance.
Our entire health care system sucks. The only people who like it are the Insurance and Pharma execs.
I won’t give a doctor a break that prescribes a non-essential medicine with a 6% success rate.