Yves here. It’s worth remembering that medical professionals and officials were successful in limiting the spread of the earlier SARS and MERS viruses. Why did Covid-19 instead become a pandemic? Ignacio picks apart some of the key lapses.
I wonder how much of the disease spread was bad luck, with the infections taking hold in Hubei right before the Chinese New Year, putting the central government in the position of having to shut down holiday travel and partying (meaning spending) if it had acted promptly. Recall also the refusal to shut down a large official banquet in Wuhan during the window when it might have been possible to contain the disease.
This Associated Press story supports Ignacio’s analysis:
In the six days after top Chinese officials secretly determined they likely were facing a pandemic from a new coronavirus, the city of Wuhan at the epicenter of the disease hosted a mass banquet for tens of thousands of people; millions began traveling through for Lunar New Year celebrations.
President Xi Jinping warned the public on the seventh day, Jan. 20. But by that time, more than 3,000 people had been infected during almost a week of public silence, according to internal documents obtained by The Associated Press and expert estimates based on retrospective infection data.
Six days.
That delay from Jan. 14 to Jan. 20 was neither the first mistake made by Chinese officials at all levels in confronting the outbreak, nor the longest lag, as governments around the world have dragged their feet for weeks and even months in addressing the virus.
But the delay by the first country to face the new coronavirus came at a critical time — the beginning of the outbreak. China’s attempt to walk a line between alerting the public and avoiding panic set the stage for a pandemic that has infected more than 2 million people and taken more than 133,000 lives.
As Ignacio points out, there is plenty of blame to spread around. Other countries’ failure to stop or severely restrict travel from China (for instance, imposing strict quarantines on arriving passengers) was another big fail.
By Ignacio Moreno Echanove, an epidemiologist
These days, lots of analyses, that retrospectively try to explain Covid-19 outcomes in different places are, I believe, quite faulty. Articles assert that this country has done far better than that other country, frequently on the basis of a single snapshot of data.
My favourite expression that I borrowed from NC commenter David, is that we are immersed in tunnel vision, overwhelmed by the enormous amounts of info coming to our radar through all possible channels. Much of the information and analyses are, again, flawed, ideologically driven, and in the worst cases totally disingenuous.
I thought it would be useful to perform some additional analysis. Instead of relying on snapshots, one should carefully analyse the cascades of events resulting in the pandemic with a hierarchy. I soon realised this was quite a hard job so I have modestly tried to scrutinize a few of these events.
From an epidemiological perspective, the data points to trace should be contagions, particularly early contagions in each region. Then, using estimates on the reproductive rate of SARS CoV 2 (R0), hospitalization rates, ICU entry rates, mortality (M) trace the progress of the epidemic. And do it with real-time data!
Since this information is not available, the published data have to be cured and lots of assumptions have to be made in the process of tracing.
By now, everybody knows that the number of confirmed cases is not a metric in both the time dimension (because gaps between contagion events and test reporting) and in quantitative terms (because the rate of tested/infected is almost always and everywhere much closer to 0 than to 1). That ratio will vary with time and geography, so confirmed cases is an unreliable source for epidemic tracing. This is truer during the early days of an epidemic, when events are critical.
Tracing casualties does a better job in quantitative terms but it is true that this information is also unreliable for some reasons. There may be political reasons to hide numbers or at least not to push for accuracy, and Covid-19 associated casualties are reported in most cases only if there is a test result demonstrating SARS CoV 2 infection. A large disease outburst will result in diagnostic and clinical systems very much overwhelmed with serious under-reporting of cases. Finally, to make estimates using deaths you will have to make assumptions on mortality rates.
Another data source is the recording of registered deaths in countries that report these in a daily basis (MoMo, Spain MoMo as an example). Of course, this is not all about Covid-19 but you can trace “excess deaths” compared with “normal” expected deaths and assuming the excess was driven mostly or totally by the epidemic, in a few instances you might come with better quantitative estimates. A mortality spike can be used to trace the progress and extent of an epidemic, identify when contagions peaked etc. I will try this and subject the results to critical examination.
If one is to use casualties or mortality to estimate “real-time” contagion events, we need to know first the approximate lag between contagion and death events.
In China it was reported that median time from contagion to symptom onset is about 5 days (large dispersion with a long tail, so better using median than average). The median lag between symptom onset and death was estimated to be about 19 days (again high dispersion and even longer tail) so I use 25 days as a proximate contagion-to-death lag. Official data in Spain validate the lags observed in China almost exactly.
Then, if there is available good data on mortality rates (M) it is possible to estimate numbers of contagions in a given day resulting in deaths about 25 days later. In Spain the mortality rate of Covid-19 has been estimated at about 1.3% on the basis of serological surveys and casualties though I don’t know if they used reported casualties or if they estimated M using MoMo “excess deaths” data. If they used reported casualties, the, real value of M in Spain would be closer to 1.6% once unreported “excess deaths” are added.
I compiled data from MoMo for Spain and using the official mortality rate (1.3%) estimated the number of contagions occurring about 25 days earlier (“real contagion time”, red line in next graph). Then, and supposing Covid-19 R0 = 6 (it has been estimated at 5.6 in some outbreaks and) we can trace events backwards up to patient 1-10 (blue-sky line before the red line in next graph).
The graph compares these estimates with reported cases as per WHO reports (dark blue) which I also represent 12 days backwards when the contagion events leading to such confirmed cases could have occurred approximately (brown line). So, the brown line would represent a picture of possible “real-time” contagion events based solely on official confirmed cases. Bear in mind the numbers depicted in the graph are in logarithmic scale.
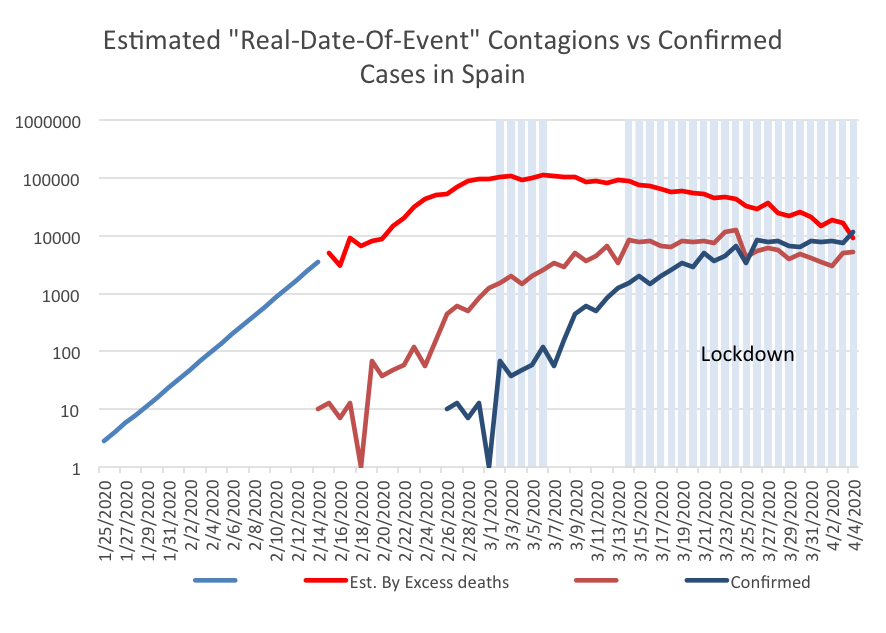
This tells a story on how events possibly unfolded in Spain and something similar could be done for countries like Italy, France, Belgium, the Netherlands, or the UK.MoMo data allow to conclude that in Spain the peak of daily contagions occurred between the 2nd and the 6th of March and then declined nearly steadily until and after the emergency and lockdown were enforced by the 14th of March. The peak of contagions is estimated at about 110.000 per day using M = 1.3% but would be much lower, about 42.000 contagions/day, if M = 1.6%. Before this peak, by February the 26th, the R0 was already dropping sharply as the slope of the red line suggests, and continued to drop into the shadowed lockdown period (remember, this is logarithmic).
So, something was changing spontaneously before the government response was enforced. In my opinion, what was changing was public awareness on the risks of Covid-19. After this, the curves in different countries could diverge in response to the milder or stricter rules imposed.
Conclusion 1: Most lockdowns were late and reactive measures that didn’t avoid the worst but only accelerated partial clearance of the epidemic. Alarm felt by the population at large was probably the first force to reduce R0 by ways of self-isolation of symptomatic individuals in countries like Italy, Spain, France the UK and in the State of NY. The “let’s flatten the curve” message was issued very late in such places when the curve had already been flattening spontaneously for some time.
The distance between the brown line (confirmed cases, moved back 12 days) and the red line (estimated contagions), is more or less equal to three orders of magnitude in early days and then drops. This shows that the detection systems in place were absolutely not up the challenge.
Conclusion 2: Lack of preparedness was severe. One cannot get ready for a challenge like this in a couple of weeks or even in a month. You need to have equipped and trained teams for sampling and testing with validated methods all around the country, fever check-points etc.
Conclusion 3: This severe lack of preparedness was probably common to most European countries, but some coped much better than others with Covid-19 suggesting that in the absence of proper preparedness risk awareness, should have done the trick.. Being late in the pandemic probably helped a lot to increase awareness at all levels. Probably, one can speculate, public awareness was inversely related with the R0.
Last but not least, the sky-blue line representing estimated daily contagions backwards assuming R0 = 6 suggests that the SARS CoV entries that resulted in the outburst in Spain could have occurred by the end of January. We should give that estimate ample margin and guesstimate that those entries possibly took place somewhere between Jan 15th and Feb 5th.
Conclusion 4: flights from/to China should have been grounded globally by Jan 15th at the latest. Scientists had long ago estimated that by mid-January SARS CoV 2 was already in Italy, unnoticed but starting the cascades of events that led to the first large European outburst.
Next graph shows a time course of excess mortality “Z score” composed with maps from 2020 week 6 to week 15 according to the MoMo web in Europe. Not all countries report, only those in grey-blue.
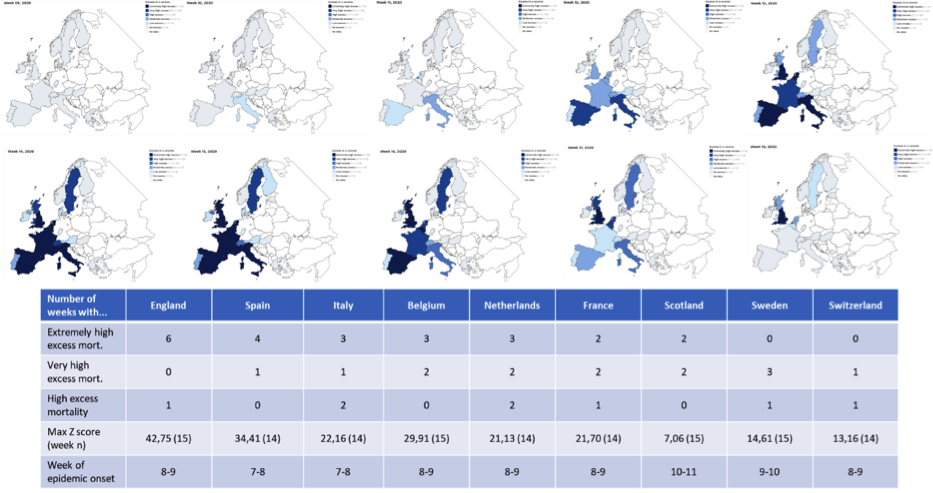
The table below the maps is mine. It summarizes the number of weeks under “extremely high”, “very high” and “high” mortality rates, plus the max “Z score” value and the first week when excess mortality is detected by this metric.
In between those countries showing clearly positive Z scores, Switzerland did the best while the UK did the worst relegating Spain to an honourable 2nd worst position. Scotland probably benefited from suffering the latest outburst with about three-week gap to become aware of what was coming. Sweden had two weeks to improve awareness and this is probably the reason they could avoid extremely high Z scores compared to other countries that showed earlier unnoticed outbursts. You can see that countries with a more ‘liberal’ approach (UK, Netherlands and Sweden) showed excess deaths lingering up to week 15 (and possibly later). When this graph was done, not all data for weeks 14-15 was gathered and the definitive results could vary with current data.
If one is to select a country that did well, Norway, Finland, Austria, Hungary, Greece, Portugal, Denmark or Ireland would be much better examples than Sweden. Switzerland, that was earlier than Sweden in the epidemic did better by all those metrics suggesting much better reaction by both, the leadership, and the population.
In those maps above the absent elephant in the room is Germany represented only by the states of Hesse and Berlin which didn’t show significant mortality spikes by the Z value.
Germany, as WHO accounts show, was amongst the first countries in Europe to report confirmed cases in significant numbers. Anecdotally, the first positive case reported in Spain was a German citizen and I find this very telling. My opinion is that German citizens were more aware than Spanish on Covid-19 risks and more prone to report their symptoms, isolate themselves etc. Besides, Angela Merkel was famously said to trust her actions on German institutions experienced in epidemiology and this country was the first to confirm home contagions and to report untraceable community transmission. This suggests both better preparedness and awareness than the other large hyperconnected countries in Europe.
Again, digging in speculative territory it could be the case that political stability, or a government that had been standing for long could possibly help for better reaction. Macron hadn’t been that long the President of France (less than 3 years), neither Conti in Italy (nearly 2 stormy years), not to mention the inexperienced Johnson and Sanchez heavily immersed in difficult internal and international affairs. Mr. Rutte in the Netherlands had been governing nearly for 10 years but possibly had not as good reaction as Merkel. It might be the case that German preparedness can be traced back as long as to 1967 when a (then) rare haemorrhagic disease (Marburg Virus, Ebola-like) erupted in Hesse infecting 31 and killing 7. Who knows?
Back to the initial outbreak in Hubei province: My initial thinking about Hubei was that given it all started in Wuhan at an explosive rate, one could expect initial stupor resulting in not the best communication of risks. Two critical data items should have been be obtained ASAP: identification of the causative agent of the disease, and determination of possible human-to-human spread.
The identification and release of SARS CoV 2 genome sequence was achieved by January the 3rd, 5 days after the alarm sounded, fairly enough fast to start tracing the new disease soon.
By January the 7ththe new pathogen was confirmed as the causative agent of the new disease. Regarding human-to-human spread, critical for switching the Precautionary Principle on, it was not officially confirmed until the 20th of January, way too late and when it had already been reported in some Chinese provinces, Thailand, S. Korea and Japan and probably had already spread to many other countries.
Only ten days later, the US-CDC was confirming person-to-person transmission within the US. This, was way too late, as we can retrospectively say, to prevent global spread. The contrast between the relative promptness with the identification of the pathogen and the sluggish reporting of the other crucial epidemiological fact was stark.
Was this crucial info withheld until the international spread of the disease helped, for instance, to rule out a blanket travel ban from/to China?
Or, is it true that thorough confirmation was needed before ‘unnecessarily frightening’ the rest of the world?
The fact is that reading both the Ch-CDC report (Feb 2020) and a study published by March 26th, it can be concluded that human-to-human spread was strongly suggested by early data. Figure 3 from the study linked above shows that 5 out of 12 cases detected in December and grouped in 4 different clusters had NO exposure to the wet market in Wuhan, but exposure to other cases.
By the time the genome sequence was published, it should have also been announced that person-to-person transmission was, to say the least, very likely.
In fairness, though it might be true that Chinese bureaucracy delayed the release of crucial information, it should be admitted that an earlier notice might have met with deaf ears in many places around the world. I haven’t found any link showing foreign authorities forcefully asking for evidence or likelihood on human-to-human transmission, or lack thereof, before January the 15th. If anyone knows better, particularly Japanese, Vietnamese, S. Korean or German readers, please comment. This is not to say there wasn’t a clamour for better and timely release of information by Chinese authorities from concerned scientists but not only scientists and through social media. As an example, this report titled “Pressure builds on China to share info on new coronavirus” and published on January10th was possibly issued hen to try to prompt a better response.
At this point, it would make sense to try to trace Hubei’s outbreak to its origin in order to check early responses and detection methods but there is no adequate data. Important questions about the origin of the disease are still unanswered and have been discussed in a previous post.
Yet we can try to trace the international spread of the virus and check downstream responses for mistakes.
First, we already have identified here one important point that was shared worldwide: most authorities in relevant positions, including the WHO, showed a lack of proper awareness of pandemic risks. Everyone was more worried about immediate effects of bold measures (like closing airways, railways and roads to human traffic from/to China) than the unknown risks of a pandemic.
As an example the head of the WHO was still ostensibly failing in his risk assessment by February 5th. In some sense he was right: By this date, SARS CoV 2 had already spread all around the world making a blanket travel ban unnecessary. By January 31st many countries started grounding flights to China but as we know this was already a late reaction that ended with worse consequences resulting in the grounding almost all fleets between 13-31st of March.
The E-CDC Technical Advising Council enclosed for a two-day meeting (Feb 18-19th) near Stockholm, about two weeks before the peak contagion period in places like Lombardy and when so far only 45 cases had been confirmed in Europe. The minutes of the meeting have been recently commented upon at El Pais (in Spanish). They reveal too much casualness about Covid-19. By this time ECDC protocols for testing were still restricted to Wuhan-related patients. This allowed for SARS CoV 2 having a wild undetected run that led to the, so far, worst outcomes we have seen with the exception of the outburst of NY a week later.
In defense of the ECDC it has to be said it is just a consulting institution without real responsibility. According to the minutes only the Danish representative prompted to search beyond Wuhan links and extend to any pneumonia. The Finish representative answered it was impossible, “everyone will be demanding tests and we don’t have enough”. This is telling; most representatives were focused strictly on clinical outcomes and forgetting about epidemiology. Only the German representative announced they had already delivered test kits to 20 hospitals and were well ahead of the rest on tests already done. Everyone was reporting difficulties purchasing clinical equipment and only Ireland stated they had already declared HC emergency and purchased in advance.
Other Asian outbreaks: tracing the epidemic in Southwestern and Pacific Asian countries would indeed be of high interest, particularly given the relatively mild outcomes in these countries that suggest more or less appropriate responses. A lot has been said about S. Korean response, less about Vietnam, Singapore, Taiwan or Japan. Unfortunately, studying separately each case would have required a lot of effort.
Though I somehow feel here out of my depth I think it can be safely concluded that there was at least one common feature to these countries: awareness on the risks of local outbreaks. Both, at the level of public authorities and citizens, awareness was widespread and this helped to keep the R0 low in these countries without the need of painful extended lockdowns. Besides, as in the case of South Korea, there was preparedness in the form of pre-existing alarm and early detection systems, as well as protective equipment etc. Their awareness was a fully internal thing that did not transpire into other foreign countries tenaciously focused on ignoring the risks. I don’t know whether they tried to give timely advice or how forcefully but this says something about the international state of affairs: Mutual trust and confidence are very much lacking.
Awareness of the population at large: Once the leadership had failed in so many places it is worth looking if the public response made any difference. As a proxy I used Google Trends and entered “Covid” as the searching term. This could somehow indicate how the population at large was aware of the risks and searching internet for information. The results are fairly consistent with previous observations.
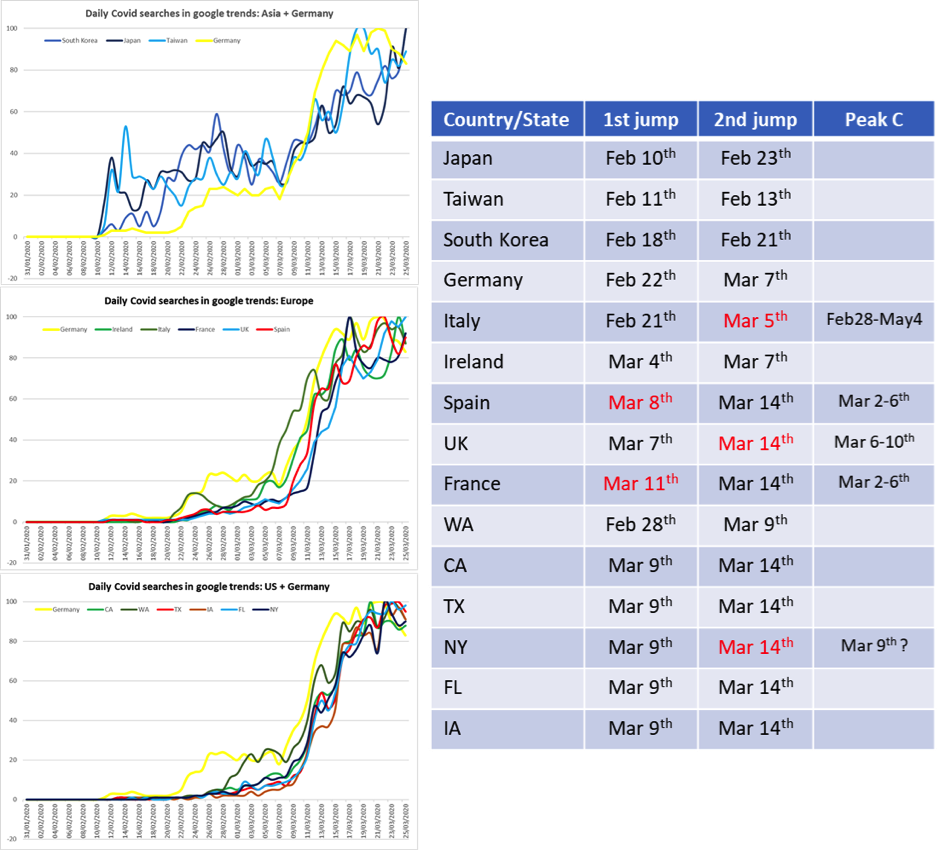
The three graphs in the left show the results obtained for a few Asian (upper graph) European (middle) and US states (lower) using Germany (the yellow lines) for comparison in the three graphs.
As expected, Japan, Taiwan or South Korea were faster to worry about Covid-19, suggesting these were more ready to increase social distancing, self-isolate if showing symptoms and accept alarm bells. Germans showed more prone to get informed than the rest of Western countries, though behind the Asian countries. It is surprising to find some initial interest in Italy in line with Germany that somehow faded later until it was too late.
The dates in red (table right to the graphs) show late reactions in countries/states that suffered the largest outbreaks probably guided by the realisation that something was wrong and when contagion peaks had already been passed. Ireland showed a jump in awareness in advance of hard-hit EU countries and I wonder what prompted this.
Regarding the US, Washington State was the canary in the mine that nobody dared to care about probably because the outburst was limited to a few counties there. Bad luck in some nursing homes! A first large wave of reactions can be noticed in the US –represented by WA, CA, TX, IA, FL and NY in the graph– driven probably by news from the other side of the pond and a second wave almost certainly related with the outburst in NY that probably helped most of the rest of the US to keep the R0 below max levels seen there. Public awareness possibly helped to keep many countries/states relatively safe as have been shown here using different approaches. Note that this metric is not about absolute search numbers but relative to a peak that has the value of 100.
One can conclude that Google Trends is a good tracker for “interest” but not necessarily suggest awareness. It was the job of the leadership and their councils to inform us about the risks of Covid-19 but most failed miserably.
As a concluding remark, I believe that future outbursts won’t be as explosive as the worst we have already seen given we have been primed to have good reaction and better detection systems are in place. I think that those tough lockdowns can and should be easily avoided.


Thank you for this Ignacio, an excellent overview.
A few random points:
As to the speed of international response, a few weeks ago the Guardian had a long form article on WHO – it aimed the blame at the claimed ‘over reaction’ to bird flu. It seems that quite a few countries (China included) were very unhappy at what was perceived to be economic damage caused by Bird Flu related restrictions. I wonder if politically this was one reason why WHO was slow to insist that China reacted more quickly, and it particular why they waited so long for ‘proof’ of human to human transmission (rather than the other way, waiting for ‘proof’ that there was no human to human transmission).
It also seems that the Germans themselves are somewhat puzzled as to how they got away so lightly – their own response seems to have been quite haphazard. One article I read referred to unknown variables. Perhaps there is something to the question of both social norms in those countries (i.e. less physical contact, different socialising patterns) and also underlying health issues – from existing inoculations, vitamin D levels, etc.
I’m curious about your conclusions that lockdowns largely came after, not before the ‘flattening of the curve’. I’ve seen articles indicating that the speed of lockdown seems to have mattered more than the nature of the lockdown – for example, in Ireland vs Britain, and Denmark vs the Netherlands. You seem to be suggesting that this is less important than informal changes in behaviour?
One final point – I’ve seen quite a few articles, especially from Europe, which seem to indicate that the worst is now over. But I’ve seen few studies to indicate that more than 5% or so of populations have been exposed – this to me strongly indicates that second or third waves are highly possible or even probable – this could make current ‘winners’ look like losers, and vice versa. I’d like to hear your opinion on this.
Regarding Germans, if we talk about cultural differences, I don’t think direct physical contact or other patterns made the difference. In my opinion, and this is why I brough the example of the German patient in the Canary Islands that reported a cough, this let’s call it “sense of public responsibility” that could make someone report and stay isolated possibly made the greatest difference keeping the R0 low. Many Italians or Spanish feeling some symptoms during February possibly didn’t even think on the possibility it was Covid-19, neither felt the need to tell the authorities, their family, friends and employers, or to self isolate in case it could be Covid-19. Possibly many thought it was a plain vainilla cough, this is not going to stop me!
But as it was spreading an increasing number of infected started to realise it could be another thing and then self-isolated themselves, spontaneously reducing the R0, as the data suggests, well before general alarm and lockdowns. At some point the R0 becomes lower simply because not the 100% of the population is susceptible but the curve suggests there is something more dramatic. A change in behaviour. This doesn’t dispute the fact that the sooner the lockdown the better but that when alarm came late, hospitals becoming flooded, there had already been a spontaneous flattening. So, what beneffited Denmark or Ireland was possibly that this spontaneous change occured earlier in the development of the epidemic. One should analyse each case separately, determine the peak in contagions, the R0, and the date of lockdown to be more precise, but this is almost certainly true for all those countries that were hit early and hard. Anyway the case of Spain was an extreme showing faster development that most others.
Regarding the last question I believe that we have seen the worst outbursts. This is not to say that there won’t be new disease escalations, but because there are now better detection systems in place and we are generally more aware of the danger, I wouldn’t expect these to be worse in extension and amplitude than those we have already seen. Some local spikes here and there, I believe and I hope!
Hello Ignacio. Fascinating analysis. I’m a reporter at CBC in Canada working on a story about different countries’ successes in dealing with the pandemic. I would love your comments. Would you kindly contact me at roberto.rocha@cbc.ca? Thank you.
But don’t get ne wrong, I think is right for the authorities to warn that the worst is yet to come precisely to keep the good spirits alive.
Thanks for this excellent piece.
There’s little to add apart from a narrow national observation from the UK. Following this from the start, I’ve been struck — and remain astounded given the significance of the implications — at how little consistency there has been about any aspect of COVID-19.
It’s probably fair to blame the failure to a degree on the political class. The UK’s is well-known to be fairly dreadful when it comes to reliably articulating what it is doing at any particular moment and why it is doing it. Having a consistent approach would have led to a lot less confusion in the minds of the general public.
But the media in all its various forms has not helped in the least. It veers from one unsubstantiated cry for action (or a different action to that which is in progress) to another without apparently any thought or pausing to draw breath. It’s only thankful that cognitive dissonance isn’t fatal. Just by way of example, here’s the Guardian (a persistent offender, but by no means the worst) on, again, just as an illustration because it’s what’s floated to the top (or near the top, as Trump as usual sucks the oxygen out of the news cycle) of the headlines today. The subject (and the decision-point) is whether the UK should have a quarantine for new arrivals. Now, being an island, you’d think that a quarantine would be — and many have said so here — a no-brainer in reducing the impact of COVID-19.
Here on May 5th was the Guardian bemoaning the lack of an early (or even a belated) hard quarantine for the UK https://www.theguardian.com/world/2020/may/05/just-273-people-arriving-in-uk-in-run-up-to-lockdown-quarantined. As an example of some of the political exchanges which the Guardian ran under the headline “UK government under fire after ‘big influx’ of Covid-19 cases from Europe revealed“:
The guardian also lamented in the sub headline “Just 273 of the 18.1m people who arrived in UK by air in run-up to lockdown were quarantined“.
So, we should have a quarantine then?
Erm, well, no. Or maybe not, anyway. Because here’s today’s Guardian https://www.theguardian.com/world/2020/jun/01/critics-round-on-no-10-over-ridiculous-rules-for-14-day-quarantine-coronavirus with the spleen-venting headline “Critics round on No 10 over ‘ridiculous’ rules for 14-day quarantine” and an “Exclusive:” sub head’er “Opponents claim exemptions to rules could mean great economic pain for little public health benefit”
I follow these things about as intently as it’s possible to follow them. But even I can’t say whether a quarantine is a good thing or a bad thing (or at least maybe an ineffective thing). Common-sense and hunches suggest that a quarantine is an important tool for controlling the spread. We can’t though, play at being amateur epidemiologists. If the government lacks a strong scientific bases for its policies, the media should call that out. But epidemiology doesn’t tend to undergo rapid, seismic shifts. It’s a fairly cautious and settled science. So why is the same media outlet criticising the UK government for both not having a quarantine and having a quarantine?
Little wonder a sizeable chunk of the population simply gives up on trying to ascertain the facts of the matter and merely does as it thinks best (even if it isn’t necessarily making the best choices). Who can blame them? And who can not have at least some sympathy if people believe no public health interventions are effective or reduce harms? If the media both undermines our governments and then goes on to undermine itself through shameless inconsistency, what choice do people have?
Regarding quarantining travellers my opinion is that there was a short frame of time when this should have worked very well: very early in the pandemic. At some point there is this Diamond Princess dilemma. What do I do with this 3.000 thousand? Or, how I am sure that the million passengers arriving today will self-quarantine? I think that the 5th of May was waaaay too late to make calls for quarantine: the epidemic was well stablished in the UK!
One reason why it took so long was that quarantining travellers was originally seen, in Europe at least, not as a health issue but as an ethical and philosophical one. Because quarantine (and even more closing borders) violated rights to free movement and was by extension racist, xenophobic etc. it was a policy only extreme nationalists could approve of. And anyway, said the same idiots, viruses don’t have passports hahaha. It took a while for the centime to drop that the issue was not a chin-stroking moral one, but an issue of life and death. How many dead people, in other words, were they prepared to accept to avoid infringing the sacred principle of free movement?
But actually, this has been one of the problems all along. It’s the same with the Civil Liberties NGO Industrial Complex: you simply cannot morally (or even practically) make a equation between your subjective sense of living in a free society on the one hand, and a pile of dead bodies on the other.
I think the influence of the airline/tourism industry shouldn’t be underestimated either – I think there was very intensive lobbying behind the scenes from airlines and airports and related interests on not slowing down travel through airports.
Here I think the failure of WHO and health authorities in general to emphasise the importance of travel in the spread of disease was catastrophic. When you have powerful economic forces saying ‘you can’t stop people travelling’ and health advisors saying ‘well, we really don’t know…’. There is only one outcome.
In a previous life I studied historical geography. That infectious disease spread through trade and travel routes was seen as so obvious it hardly required qualification, and that this spread was a fundamental factor in historical forces was considered entirely logical (see, for example, William McNeill’s classic book on the topic, although his conclusions were not new or controversial among economic or historical geographers). This is something that humanity has known for millennia…. quite literally. And yet somehow in the last few years this has been ‘forgotten’.
Yes, most definitely. Intra-EU politicking I suspect played a part in ending up with a strong tendency to make sure everyone looked like good little Europeans and didn’t put up any of those nasty old barbaric borders and for the U.K. I can say for definite that the U.K. government didn’t want to feed the incessant cries of how Johnson was a dictator who was going to enslave the entire population of Britain, sell Scotland to Donald Trump and send child migrants up chimneys or something.
While done with good intentions, this civilisation proving by open borders virtue signalling was a disincentive to right action.
For an example of the prevailing contemporary mood music, here’s the sort of thing that was being put about https://www.europarl.europa.eu/RegData/etudes/BRIE/2020/651343/IPOL_BRI(2020)651343_EN.pdf — I was going to quote abridged excepts but, what the heck, everyone can have a read at the nonsense which was being shoved down our collective throats at the time:
“The legality of cross-border mobility restrictions introduced in the name of COVID-19 is put in doubt by some analysts […] The proportionality of the sanctions imposed for violation of the restrictive measures remains an issue to be followed […]”
I have not seen such a clutching of pearls since I watched The Little Mermaid.
a stable with open door and a stable with closed door in relation to a horse?
I wonder what the response would have been if this virus originated in the US? It scares me to even think about this scenario considering our governments anti science administration. Considering all of the facts, I believe China generally acted prudently. This being a completely new pathogen , China had nothing to go on. It’s easy to second guess, but China took , in my opinion, very fast action. It does no good to try to blame China. Instead world governments should be working together not blaming others. The behavior of the US government is shameful and not defendable.
China, didn’t exactly have nothing to go on, in that they say unlike the US, UK, & EU, had a lab studying bat coronaviruses. No I don’t think any leaked out into the Wild. They didn’t have anything in the lab (based on data hey turned over to WHO) that could jump to humans. And the Chinese had plenty of PPE. Really, another excellent article/post. Regarding future outbreaks in the US, as long as trump is around, he creates a real danger that nothing will get done right. So, I’m worried. Not of one big spike, but of a never ending series of outbreaks.
At this point, it does no good to cast blame. But the atypical pneumonia (observed as early as November 17), resembled SARS, so China had its history with that illness as a basis. Detentions of physicians who raised alarms:
“Wang Guangbao, a surgeon and popular science writer in eastern China, later said speculation about a return of Sars-like virus was rampant around 1 January within medical circles, but the detentions dissuaded many, including himself, from speaking openly about it.”
https://www.independent.co.uk/news/world/asia/coronavirus-china-outbreak-wuhan-who-latest-a9313241.html
On or around Dec 31st, the date Taiwan notified the WHO of probable human-to-human transmission, Chinese officials themselves most likely suspected human-to-human transmission of a SARS-like pathogen:
“China is investigating an outbreak of atypical pneumonia that is suspected of being linked to severe acute respiratory syndrome (SARS), the flu-like virus that killed hundreds of people in the early 2000s, state media reported Tuesday.
A team of experts from the National Health Commission were dispatched Tuesday to Wuhan, in central China’s Hubei province, and are “currently conducting relevant inspection and verification work,” state broadcaster CCTV reported.”
https://www.japantimes.co.jp/news/2019/12/31/asia-pacific/science-health-asia-pacific/outbreak-sars-like-pneumonia-investigated-china/#.XtZ8LojYrrc
As late as Jan 23, the WHO declined to declare the outbreak a global emergency /2020/01/23/health/china-virus-who-emergency.html
I liked your piece, Ignacio, but I think something important is missing.
Why did Covid-19 spiral out of control? Because people need masks and social distancing to control it. No country has been able to avoid both Covid-19 and masks & social distancing. It’s either one or the others.
In Europe, Covid-19 spiraled out of control because masks & social distancing are a difficult sell without the previous experience of SARS.
All this is bad news. It means masks & social distancing are going to stay here undefinitely, or be replaced by Covid-19 spiraling out of control again.
Which is why I think that We The People of The United States of America should have been issued masks.
I mean, come on. It could have been a fashion statement. Don your washable Made in the USA mask in that fetching red, white and blue color scheme.
>As a concluding remark, I believe that future outbursts won’t be as explosive as the worst we have >already seen given we have been primed to have good reaction and better detection systems are >in place. I think that those tough lockdowns can and should be easily avoided.
I hope you’re right, but I doubt it. I believe this pandemic will mirror the historicals, which means a bad second wave in the fall. I’ve seen NOTHING that gainsays this, and indeed, if you listen to him carefully, this is what Michael Osterholm is predicting (in less inflammatory language).
As for our ability to respond, that’s been put on pause by the riots. We don’t know how long those will last, but they’re certainly epidemiologically equivalent to a Phase III reopening. It don’t think we’ll see marked effects, because the apparent seasonality of the virus is in play for the next several months. But we really don’t know.
I’m with you, Pessimist, altho I’d love to be wrong. The social conditions are very poor. I think the social conditions are more deterministic than medical science.
Thanks, Ignacio for a really interesting survey. I’d only add that if there is a common factor to the failure in a number of different countries, it’s the inability of technocratic governments to handle genuinely complex issues. That may sound strange at first, but “technocratic” here doesn’t mean “knowledgeable” or “technically qualified”, it means Ministers and officials obsessed with the mechanics and procedures of government, dominating public opinion and getting and staying elected. As a result, most governments looked at the epidemic for far too long as a PR problem, a foreign policy problem, a media problem, a political management problem, instead of seeing it for what it was. Initiatives and statements were often confusing and even contradictory.
France is a case in point. For weeks, the government told people that masks were unnecessary, and even pointless. It then became clear that they had only said this because there were very few masks available, and they didn’t want to seem unprepared. Now, masks are compulsory in shops and public transport, and this rule is being strictly enforced. It’s no wonder people get confused, and start disbelieving the government: fortunately, innate good sense and social responsibility appear to be saving the day. The episode was made worse because communication was originally left to the government’s official spokesperson, a nonentity whose “job” (she uses the English word) is actually to be the token African woman in the government, rather than to actually do anything. It didn’t help that she denounced press reports that schools were to be closed as “fake news” (in English again) a few hours before the government announced that that was going to happen. Those two episodes did a lot to damage the government’s credibility, and produced the universal reaction Ils se foutent de notre geule , which is difficult to translate and not very polite, but means roughly “the (familybloggers) are taking the (familyblogging) (familyblog) out of us”.
Notions of accountability fade with the next news cycle, but don’t have to. There are structural problems to address regarding various government actions or inactions to allow some after-the-fact review or post-mortem. That has worked in different areas, so why not allow citizens the same courtesy? After all, they voted for the taxes to pay for those actions or inactions.
That suggests not just sunset laws but periodic and episodic reviews during that long day’s journey that serve as objective, impartial witness to what transpired.
fortunately, innate good sense and social responsibility appear to be saving the day
This is what has/is been happening in my little corner of washington state, thankfully.
I have kept as up to date as possible with the help of nc’s wise european readership with special kudos to ignacio. Many thanks, I’ve been waiting for this post
There wasn’t only the masks cockup, there was also the idiocy of maintaining the first round of municipal elections on March 15th, when no one was yet advised to wear masks. Add to that the absurd circumstances that led to the LREM candidate withdrawing from the Paris mayorial race only to be replaced by the sitting Health Minister, who herself had said that the elections should have been entirely postponed and that maintaining them was a “mascarade”.
As an Italian friend put it, “i francesi sempre chaotici”.
Yes! A one-time mentor used to argue that the world was divided into ‘engineers‘ and ‘courtiers‘ by which he meant respectively those whose motivation was to make and fix things and those whose first – and often only – thought was of presentation.
It seems the courtiers have completely taken over so when something does need to be fixed they have no idea and nowhere to turn.
Particularly in the US, there is a desperate need for the ‘courtiers’ to at least listen to the ‘engineers’ if not surrender control of public policy-making decisions to them entirely. The ‘courtiers’ have already proven they are willing to throw future generations and a habitable planet under the bus to preserve their privileges and power. Now it appears they are willing to throw the elderly and just about anyone in less than perfect health under that same bus as well.
The take-away here seems to be focusing on efforts to educate the public about the costs of continuing to listen to the promises of the ‘courtiers’ to bring back the good old days. For the purposes of this post a focus on the numbers of dead was appropriate. I suspect however it ignores the long-term costs to those who to some degree or other ‘recovered’. Have there been any studies of the physiological damage to those infected but not appearing to have seriously experienced any symptoms?
(Thorstein Veblen discussed this issue in a different context more than a century ago. See The Engineers and the Price System. )
I very much agree. I think that technocratic governments as per your definition, obssesed with the mechanics and procedures, including with these an obssesion with timing, (electoral timing etc) where also probably shocked to see an event coming whose timing couldn’t be controlled and was, as in the case of the municipal elections in France, interfering with their carefully thougth movements.
A Canadian friend commented that his neighbor worked in Wuhan. His neighbor returned with his family in November last year because of unease caused by mysterious rise in illness. This anecdote supports Ignacio’s belief that the populace reacted ahead of government lock downs, reducing the infamous R0.
Compliments, Ignacio. You have explained this clearly and thoroughly–and this isn’t the first enlightening article that you have given to us.
There is some good information out there–I find the Italian press to be dealing very well with explaining the pandemic–but what you have done here is generally well above the quality of reporting and synthesis of lines of information found in the Anglo-American sphere. I am glad that you bothered to learn English so perfectly.
Kudos to Yves, who helped with my not so perfect English!
Muchas gracias, Ignacio!
For HK, the leadership was toeing the mainland party line. Action was taken by the population, including the threat of strikes by the medical workers to force border closures.
Taiwan e-mailed the WHO on December 31st, then immediately implemented measures assuming human-to-human transmission, which included enhanced border control and isolation. After sending a fact finding party on Jan. 13-15, Taiwan activated its Central Epidemic Command Center.
Time line: https://time.com/5826025/taiwan-who-trump-coronavirus-covid19/
Official Taiwan CDC: https://www.cdc.gov.tw/En/Bulletin/Detail/PAD-lbwDHeN_bLa-viBOuw?typeid=158
I would point to past experience with SARS, and to the fact that it was right before the Lunar New Year. Taiwan was very vulnerable, as hundreds of thousands of Taiwanese live and work in the mainland, and were set to flock back home.
Taiwan leadership did very well indeed. Thank you for these comments with complementary info. Seems that nothing like being too close to, to avoid the hard consequences those faraway suffered.
I extend my gratefulness to all commenters, I wish I could answer all!
Thank you, Ignacio for this post.
Regarding conclusion 4, no travel from China by Jan 15, what would have been the basis for that at that date, if the 2002, 2003 SARS was also spread human to human (the current one not confirmed till Jan 20, though strongly suggested by early data) and the world was not much impacted outside Asia 18 or so years ago?
That is, would would have been there to conclude this was and would be worse than the one in 2002? I don’t remember travel restrictions back then, whether imppsed by nearby countries, or Europe/America.
Thanks.
Would more information from China in those early days (for example, the quoted Jan 10 report above) help with the decision?
Because early data showed very easy human-to-human spread, much easier than SARS and the Chinese HC system had probably noticed that difference well before Jan 15th. Many here at NC could “notice” it being some thousand miles away simply by the speed of upcoming news.
Muchas gracias, Ignacio.
Anecdotal evidence from Luxembourg, because we suffer small country bias: massive number of infections (4k in population of 625k), but fairly low fatality rate and NO excess deaths.
Government wants to test entire population, but whether valid conclusions can be drawn due to aforesaid bias is questionable.
Never closed borders, but everyone closed them on us, so stuck here for two months. Necessary, but mentally weird for someone who hardly remembers pre-Schengen times when passports were required and for a population used to going shopping in Germany/Belgium/France, all of tops 30 minutes away.
Experts vying for narrative control…
It’s naziville out here in Caly, subject to discipline and termination. Better to collect the extra 600…
Businesses going out left and right. Older owners packing it in.
And that Barron’s article was spot on.
With social distancing to create more space for tech control and the elimination of commercial recourse, why would either side want offices?
A big factor is very simple. China was not really connected to the world until the past 10-20 years. Now people go back and forth from China similar to going to and from Europe.
Prior to the past couple of decades, flus etc. had to get to Hong Kong or Singapore from China and then they could roam free. Now they can get on a plane for any major city in China and be on another continent within hours.
The 1957 flu was first identified in Singapore. The 1968 flu is named “Hong Kong Flu”. These flus could have origninated in those countries as all it takes is people living in close proximity to farm anaimals (e.g. Mid-West US and start of 1918 flu).
SARS and MERS were close runs. If those bugs had an extra couple of days of asymptomatic incubation then they could have roamed free and caused a pandemic. However, they had relatively short incubation periods and then were very debilitating and fatal quickly, so they could be identified and quarantined quickly.
The relatively long incubation period and large number of asymptomatic or pre-symptomatic spreaders for the current bug is a key to it spreading widely.
So in the past 20 years, we have had two near-misses and one direct hit from potential pandemic bugs that escaped China. At this point, we need to assume that China has the potential for producing another one of these every 5-10 years. that is what our systems need to be prepared to address. There are other countries that can also produce them, but the sheer number of people in China, especially in agricultural ares, means that they are likely to be a dominant source for a long time.
Excellent article. Good scientists like to stick to the facts. But we must not fail to look at the political aspect of the human reaction to the pandemic. There was a shortage of PPE outside of China because there are basically no manufacturing plants elsewhere. The one face mask plant in the USA in Texas never got a government contract and did not increase its production. This was directly due to the Donald Trump Administration and the company not being connected to the right families. Due to the shortage of masks officals downplayed the importance of wearing them in public.
Spain and Italy are the “sick men” of Europe. The European Union was worse than useless during the pandemic. The USA, UK and Sweden are infected with the neoliberal ideology that decimated their governments so the rich could get richer. The aristocratic heads of the Atlantic Alliance decided the deaths of its citizens were off no consequence. Today, there still is no old fashion, proven effective, national public health campaign to test, trace and isolated the ill in the USA. Clearly, pharmaceutical profits from a future patentable vaccine are more important than American lives.
My mutterings from Germany…
The author is missing Australia: they where on the sunny side of the planet – that helped them avoid the first run of the pandemic, because of white skin, vitamin D and summer on their part of the blue marble we are so fond of…
Germany had the sheer luck of having some competent men at the right places: virologists and epidemiologists like Mr. Drosten or Mr. Lauterbach, a member of the parliament.
The next important factor is how to manage infected people: in Germany they stay in the hospital until they are cured or dead. That’s a very simple fact. And reopening the closed floors in the “we have to save money” hospitals was one of the first steps when the pandemic went rampant in Italy. Then the Italians and Spaniards made one big mistake: they send people with “mild” symptoms into caring & nursing homes but there was no isolation protocol for those and not enough protective gear like masks, shields gloves and desinfectants. Going low on the sun and not enough vitamin D in your body, especially if you are old seems to be the way of euthanasia nowadays – and no, there is no plan behind this, just normal incompetence and ignorance.
Next: Italians and Spaniards tend to avoid the sun whenever possible – not only in the summer but in a caring and nursing home over the whole year. Together with the failure of sending infected patients to these homes, this was – in hindsight – one of the factors which boosted the number of sick and dying people.
In Germany we have had the luck of the enormous public news sector – we’ve had our ‘Hugenberg’ in the 1920ies – now we don’t need someone like Rupert Murdoch any more – and we had actual news snippets every evening in the ‘tagesschau’ – the news show on television, which resembles the modern version of a campfire, but for the whole nation.
As a sidemark: if you want to become friends with a German, never – never – phone him between 8 p.m. and 8:15 p.m. That’s the airing time of the tagesschau…
The failure of sending infected people with ‘mild’ symptoms into nursing & caring homes was repeated in New York. We now know the outcomes of such a policy.
Again: having the possibility of diagnosing Covid-19 from the 16th of January on together with a constant stream of informations from Wuhan first and Bergamo later on made the general public aware of “something’ is coming over us’. So the public reduced their activities way before any lockdown measures had been taken by the federal and local authorities.
Oh, I missed lots of countries and focused mainly on those that saw disease spiralling out of control and for which I had data to analyse. What about Iran, for instance? I think your comment on what happened in Germany might be pushed forward about 3 weeks after the 16th of January you mention. Anyway it points to the same conclusions noted in the post.
Thank you, Ignacio.
There is a good piece on Ft Alphaville about the nonsensical UK strategy.
https://ftalphaville.ft.com/2020/06/01/1591001732000/Making-sense-of-nonsensical-Covid-19-strategy/
That is really a good piece. A mistake is identified early in the article: Treating SARS CoV 2 as if it was a new flu strain instead of a completely new virus.
This is a good article , Thanks for sharing
https://mariamalonzo2020.wixsite.com/fva1
The analysis in the article is dishonest:
First, there is a clearly defined difference between limited H2H transmission and sustained H2H transmission in epidemiology.
Sustained transmission is H2H transmission that is easily and continuously transmitted from person to person.
Limited H2H transmission is when a virus dies out or stops transmitting after infecting a few people in clusters.
At that early point in China there was not enough testing or information to ascertain sustained transmission. Lethality was unknown, as there were no deaths until Jan 9th, and that was a senior with serious co-morbidity.
https://www.statnews.com/2020/01/21/who-raises-possibility-of-sustained-human-to-human-transmission-of-new-virus-in-china/
H2H transmission is unsurprising between family members–they live, breathe, eat, and often sleep together. That means there are multiple possibilities for transmission–airborne (including droplet), direct physical contact (including sexual, and/or body fluids), fomite, fecal-oral. Because the mechanism of transmission was clearly unclear at that point–as well as virulence–it’s quite legitimate for the officials to move cautiously and investigate further before making an announcement that could 1) impact the operations, business, and livelihood of an entire city 2) cause unnecessary panic 3) necessitate strong NPI measures.
For example, AIDS is clearly H2H transmissible, but it wouldn’t warrant a quarantine on a city or even individuals.
Also, the issue of asymptomatic transmission was totally unclear at this point (unlike SARS) which also affects policy and measures.
***********************
See below for WHO timeline. Note the specificity of the language.
14 January 2020
WHO’s technical lead for the response noted in a press briefing there may have been limited human-to-human transmission of the coronavirus (in the 41 confirmed cases), mainly through family members, and that there was a risk of a possible wider outbreak. The lead also said that human-to-human transmission would not be surprising given our experience with SARS, MERS and other respiratory pathogens.
https://www.who.int/news-room/detail/27-04-2020-who-timeline—covid-19
Data collected through detailed epidemiological investigation and through the deployment of the new test kit nationally suggests that human-to-human transmission is taking place in Wuhan. More analysis of the epidemiological data is needed to understand the full extent of human-to-human transmission. WHO stands ready to provide support to China to conduct further detailed analysis.
https://www.who.int/china/news/detail/22-01-2020-field-visit-wuhan-china-jan-2020
See here for phases of alert, based on probability of transmission:
https://www.cidrap.umn.edu/news-perspective/2009/04/what-do-who-pandemic-alert-phase-changes-mean-you
Here are some more examples from the CDC of H2H transmission that is limited, non-sustained.
https://www.cdc.gov/flu/avianflu/h5n1-human-infections.htm
“It is possible for human-to-human transmission of other non-human (animal-origin) influenza A viruses to range along a continuum; from occasional, limited, non-sustained human-to-human transmission of one or more generations without further spread (“dead-end transmission”), to efficient and sustained human-to-human transmission. Efficient and sustained (ongoing) transmission..among people in the community is needed for [an influenza] pandemic to begin.
Inept apologetics don’t go down well here, particularly when they don’t look organic either.
And that’s before getting to the fact that you are utterly out of line in making baseless personal attacks.
Plus you attack is pure projection. Anyone who compares an STD like AIDS to an airborne, highly contagious disease in terms of transmissibility is either a fool or a fabricator. Take your pick. And my gay friend like to point out that AIDS is actually not easily contracted (the risk is to the sperm recipient and for anal sex, requires over 1000 penetrations on average).
And your argument is not accepted by anyone credible. Start with the AP story I cited, which is an analysis of Covid-19 widely accepted among epidemiologists and scientists.
It is nonsensical trying to divert the attention to the reality with the use of qualifiers like “sustained” or “easy” that I carefully tried to avoid in the article.
Early data suggested clearly that person to person transmissión was not only occurring but very frequent among December patients being asked. If you need to wait, as the WHO did, nearly a month to say this was “sustained” when it was obvious that many were already infected in Wuhan and cases were appearing at an explosive rate, why we need epidemiological vigilance?. This was an obvious failure.
I have lived a similar experience in Madrid and in a single week, even in a couple of days many normal citizens passed from purposedly ignoring Covid-19 to very alarmed. I guess that epidemiologists in China, knowledgeable about previous zoonotic outbreaks like SARS, noticed this quite soon. The alarms sounded by the end of December all around the world and news came at a speed that soon indicated something big. A
ll the speculations about family members and routes of transmission are bad excuses that cannot hide the fact that this disease, from the very beginning, was seen to spread at an explosive rate. This info was withheld for a critical period probably for the reasons explained in the AP link you cited.
I wonder if a certain relaxed complacency on the part of organizations, officials, politicians, and the general public was encouraged by the way we managed to ‘dodge the bullet’ for both SARS-1 and MERS.