By Jay Hancock, Senior Correspondent for Kaiser Health News. Originally published at Kaiser Health News.
Three years ago, pharma giant Pfizer paid $24 million to settle federal allegations that it was paying kickbacks and inflating sales by reimbursing Medicare patients for out-of-pocket medication costs.
By making prohibitively expensive medicine essentially free for patients, the company induced them to use Pfizer drugs even as the price of one of those medicines, covered by Medicare and Medicaid, soared 44% to $225,000 a year, the Justice Department alleged.
Now Pfizer is suing Uncle Sam to legalize essentially the same practice it was accused of three years ago — a fighting response to a federal crackdown that has resulted in a dozen drug companies being accused of similar practices.
A Pfizer win could cost taxpayers billions of dollars and erase an important control on pharma marketing after decades of regulatory erosion and soaring drug prices, say health policy analysts. A federal judge’s ruling is expected any day.
“If this is legal for Pfizer, Pfizer will not be the only pharmaceutical company to use this, and there will effectively be a gold rush,” government lawyer Jacob Lillywhite said in oral arguments last month.
Pfizer’s legal argument “is aggressive,” said Chris Robertson, a professor of health law at Boston University. “But I think they’ve got such a political tailwind behind them” because of pocketbook pain over prescription medicine — even though it’s caused by pharma manufacturers. Pfizer’s message, “‘We’re just trying to help people afford their drugs,’ is pretty attractive,” he said.
That’s not all that’s working in Pfizer’s favor. Courts and regulations have been moving pharma’s way since the Food and Drug Administration allowed limited TV drug ads in the 1980s. Other companies of all kinds also have gained free speech rights allowing aggressive marketing and political influence that would have been unthinkable decades ago, legal scholars say.
Among other court arguments, Pfizer initially claimed that current regulation violates its speech protections under the First Amendment, essentially saying it should be allowed to communicate freely with third-party charities to direct patient assistance.
“It’s infuriating to realize that, as outlandish as they seem, these types of claims are finding a good deal of traction before many courts,” said Michelle Mello, a professor of law and medicine at Stanford University. “Drug companies are surely aware that the judicial trend has been toward more expansive recognition of commercial speech rights.”
Pfizer’s lawsuit, in the Southern District of New York, seeks a judge’s permission to directly reimburse patient expenses for two of its heart-failure drugs each costing $225,000 a year. An outside administrator would use Pfizer contributions to cover Medicare copays, deductibles and coinsurance for those drugs, which otherwise would cost patients about $13,000 a year.
Letting pharma companies put money directly into patients’ pockets to pay for their own expensive medicines “does induce people to get a specific product” instead of shopping for a cheaper or more effective alternative, said Stacie Dusetzina, an associate professor of health policy at Vanderbilt University. “It’s kind of the definition of a kickback.”
Government rule-makers have warned against such payments since the launch of Medicare’s Part D drug benefit in 2006. Drug companies routinely help privately insured patients with cost sharing through coupons and other means, but private carriers can negotiate the overall price.
Because Congress gave Medicare no control over prescription drug prices, having patients share at least part of the cost is the only economic force guarding against unlimited price hikes and industry profits at taxpayer expense.
At the same time, however, regulators have allowed the industry to help patients with copays by routing money through outside charities — but only as long as the charities are “bona fide, independent” organizations that don’t match drugmaker money with specific drugs.
Several charities have blatantly violated that rule in recent years by colluding with pharma companies to subsidize particular drugs, the Justice Department has alleged. A dozen companies have paid more than $1 billion to settle allegations of kickback violations.
Pfizer set up an internal fund at one of the charities, the Patient Access Network Foundation, to cover patient costs for a heart arrhythmia drug at exactly the same time it was raising the wholesale cost from $220 to $317 for a package of 40 capsules, the Justice Department said. Pfizer referred Medicare patients who needed the drug to the PAN Foundation, the government said.
Under such arrangements, every $1 million channeled through a charity “has the potential to generate up to $21 m[illion] for the sponsor company, funded by the U.S. government,” Andrew Baum, a Citi pharma stock analyst, wrote in 2017.
Pfizer settled the case, saying it was not an admission of wrongdoing but resulted from its “desire to put this legal matter behind us.”
The PAN Foundation and three other charities also made deals to resolve allegations that they functioned as disallowed conduits for patient assistance for multiple pharma companies. One organization, the Virginia-based Caring Voice Coalition, shut down after government scrutiny.
PAN’s settlement did not mention the alleged Pfizer transactions. Those were described in the separate government deal with Pfizer.
The 2019 PAN agreement related to “legacy matters” and “did not involve any of PAN’s current operations or disease funds,” organization CEO Dan Klein said via a spokesperson. “Nonprofit patient assistance programs like PAN are necessary to help people access the critical medications they need to stay healthy.”
But legal troubles have hardly slowed the pharma-funded patient assistance business.
Four penalized nonprofits agreed to stop directing money to specific drugs, but they continue to accept hundreds of millions of dollars in pharma donations to indirectly cover copays and other patient drug costs, organization reports and IRS filings show. HHS regulators allow the practice because the drug companies are not involved in deciding which patients and which drugs are subsidized.
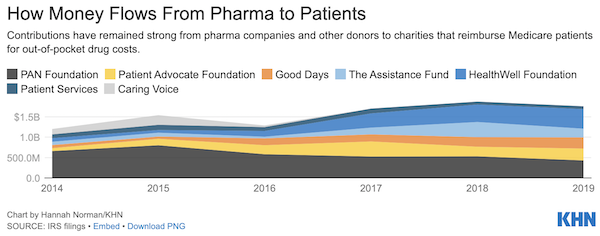
Donations to six pharma-funded patient assistance charities reached $1.8 billion in 2019, only slightly less than the year before, a KHN analysis of their IRS filings shows. That was nearly 50% higher than the amount from five years previously, before the Justice Department started cracking down.
Last year Pfizer donated $39.7 million to PAN and five other charities helping patients with out-of-pocket drug costs, company disclosures show.
If Pfizer’s lawsuit seeking to earmark such donations for its tafamidis heart-failure drugs opens the way for similar practices industrywide, it would drive up Medicare costs through rising prices and numbers of prescriptions, said Gerard Anderson, an economist and health policy professor at Johns Hopkins University’s Bloomberg School of Public Health. Such a program for tafamidis alone would increase Medicare costs by $30 billion, the Health and Human Services Department’s inspector general estimated.
Pharma companies can “learn which patients are using the drug, and they can market [and offer financial assistance] directly to that patient,” Anderson said. “You get a huge return.”
Pfizer argues that its proposal, which the HHS inspector general called “highly suspect” in an advisory opinion before the company filed its lawsuit, is legal and sensible.
“Providing copay assistance to middle-income patients who have been prescribed tafamidis is an efficient and equitable way to lower their out-of-pocket costs,” company spokesperson Steven Danehy said.
But the real affordability problem for patients is that tafamidis is too expensive, federal attorney Lillywhite said in court arguments last month. (HHS’ Office of Inspector General declined to comment.)
Pfizer has “priced itself out of the market,” he said. The company is seeking to “do something that’s unprecedented, to upend decades of settled law and agency guidance” to boost sales of “what is the most expensive cardiovascular drug ever launched in the United States.”
After the oral arguments, Pfizer dropped claims that HHS rules violate its free speech rights. Judge Mary Kay Vyskocil is considering only the company’s contention that a dedicated fund for tafamidis would not violate kickback prohibitions because, among other arguments, it is the doctor who decides to prescribe the drug and create revenue for Pfizer, not the patient getting the financial assistance.
But legal analysts still see the case as part of a broad movement toward deregulation and corporate rights.
A 1970s Supreme Court case, viewed as paving the way for an explosion of drug, lawyer and liquor ads as well as corporate campaign donations, was about speech rights for prescription drug sellers in Virginia. In 2011 the court found that the First Amendment allows data miners to buy and sell prescription records from pharmacies, provided the patients aren’t identified.
A year later, a federal appeals court cited speech protections when it overturned the conviction of a pharma sales rep who had been promoting a drug for uses not approved by the FDA.
Even if Pfizer loses its case, the climate may be ripe for similar challenges by other drugmakers, especially after the appointment of more than 200 federal judges by business-friendly President Donald Trump, legal scholars said.
The federal kickback law doesn’t mention copay assistance charities “and wasn’t designed with these programs in mind,” said Mello, of Stanford. Pfizer’s lawsuit “should be a loud, clanging call to Congress” to explicitly define drug assistance subsidies as illegal kickbacks, she said.


Predators are always on the lookout for a kill. Why should drug pushers be any different.
Seldom have governments mandate that their citizenry submit to experimental therapies.
The hundreds of billions of dollars at stake are more than enough to for any ration person to distrust every assertion and all data.
How could the Covid pharma pipeline even be shut off at this point without crashing the equities markets and pensions vested in pharma stocks that have gone from $13 to $350 in two years generating billionaires and covering vast public and private funding shortfalls?
The mandates and enormous hundreds of millions of doses a pop government purchases orders are now an effective mechanism to contrive otherwise impossible fiscal policies. Even getting funding for bridges and power distribution is presently taking a backseat to mandated pharma.
And NO liability.
Pfizer is just getting started….
https://twitter.com/ChrstnBnano/status/1421828905531449353?s=20
Corporations/Businesses are mandating that citizenry submit to experimental therapies.
And all the risk in on the subject of the experiment.
No liabilty.
To top that off: The cost of getting sick is all on you ….for the sake of the economy.
Trump greenlighted importing Rx from Canada in the summer of 2020. Looks like that is stalled under Biden
https://www.cov.com/-/media/files/corporate/publications/2020/10/hhs-and-fda-actions-on-importation-of-prescription-drugs-from-canada-and-other-countries.pdf
http://www.msn.com/en-us/news/politics/four-senators-call-on-becerra-to-back-importation-of-prescription-drugs-from-canada/ar-AAMBCdt
The Feds should say ‘Right. We are going to do a tax audit of you and teams of our investigators are right now going through your corporate headquarters seizing every record and computer that they can find. And we are also seizing all records of your Covid Pfizer drug as well so that we can determine how you judged the safety of your vaccine.’ And tell them that they will no longer have any access to any government research whatsoever and from now on, they can do their own basic research. It’s the Chicago way as you are essentially dealing with mobsters-
https://www.youtube.com/watch?v=cjOPLTTjnwc (44 secs)
” It’s a racket. Those stock market guys are crooked ” said Al Capone & of course there were those other guys called the Chicago Boys who introduced the Neoliberal racket to Chile.
A piece of footage in some wildlife film I saw many years ago featuring a caribou reminds me of these people in the sense that it was slowly being drained of it’s blood by thousands of mosquitoes or midges so effectively killing it. I suppose that the only difference with our rent seeking parasites is that for them & us, there is no Caribou B.
Quote “A Pfizer win could cost taxpayers billions of dollars and…”
Uh… You may be forgetting a one small thing. At the federal level, taxes in no way, shape or form fund federal spending. All federal spending is the creation of new money (all tax payments to the federal govt are destroyed from an accounting perspective). This is an accounting fact that you can verify. Please read “The Deficit Myth” to gain a correct understanding of federal monetary operations. You can also read the various books by Warren Mosler (free on his website). The federal govt has no fiscal constraints, only real constraints in the real economy.
This was also explicitly confirmed by Alan Greenspan in his famous response to Paul Ryan. It’s on youtube.
advait
August 1, 2021 at 12:03 pm
Yep.
So if we are to make a dent in the messaging fairy’s narrative, how would you rewrite the quote? What will break the federal tax payer “pay for” mythos? Or the federal budget is like a family’s, we all have to tighten our belts with shared sacrifice, etc.?
So so many ways that they, and “we” ourselves inadvertently, invoke the cultural messaging / whispers even.
Your reply is thoughtful and on target. One way to make a dent is to learn about MMT and spread the word. Also I recommend reading “A People’s History of the United States” by Howard Zinn. Pfizer’s antics to legalize corruption is simply what happens when Americans allow the wealthy to use their power to craft laws in their favor.
Taxes are to make something more difficult to do – so – Pfizer wining will make it more difficult for taxpayers to get healthcare and medications and easier for Pfizer to rip off the public.
The billions of dollars could be much better spent directing effort towards lessening a real constraint on the economy (say by insulating houses or building an eco-insulation factory) instead of giving even more money to the wealthy owners of pharma companies to inflate asset prices, bribe legislators and innovate.
The money is fiat but the displaced and misplaced investments are actual as is the increased concentration of wealth.
In the absence of single payer and a national formulary and pricing, or at least one for all Medicare and Medicaid beneficiaries, these pharma funded “charities” are a necessary evil for some.
Our disabled son requires expensive medications most of which are covered by Medicare part D. However the plans only cover generics with a hefty copay. But generics, while usually a good thing, have caused him problems. As I understand, generics are allowed to deviate +/- 20% for the active compound. Each manufacturer uses different fillers. While this usually doesn’t matter in most cases, sometimes it makes a huge difference. In his case brand versus generics was significant. Brand, of course is very expensive even though the medication is off patent and was developed in the 1960s.
As a consequence, he uses one of these drug plan schemes to get the name brand drug. It is not cheap and was a huge effort to get him accepted. Even with the drug charity, it remains very expensive.
He attended university in Ontario and was required to purchase a private health insurance plan that mirrors OHIP, Ontario’s single payer. The university had a drug plan. Needless to say, his medical care and medications were seamless and frictionless. And cost was a small fraction of Medicare part A, B and D and the supplement.
We needs single payer now. Euthanize private health insurance corporations and cram down pricing of drugs and services.
NOTE: other comments here are focused on vaccines; this is not what the KHN article is explaining.
Corporate Free Speech has always irked me – How can a corporation have any free speech with so many inside the corporation having different views on myriad topics…the best that could be expected is incoherent babble – a corporation with free speech is only a thin veneer to those who’s message is brought forward through the corporation, messaging through the corporation is only a way to give certain individuals an unequal advantage or more rights-to-rights and the law than others. All this is legislated and made law by the congress critters – so of course, corporate campaign funding – for decades – has favored scams and scammers into office to gain special permissions and laws the rest of us citizens can’t use – in effect, it gives certain individuals extra free speech, extra legal privileges, extra legal protections, extra support, extra tax payer dollars and most everyone else less of all the above. So – really – I do not get how the Supreme Court can be so deluded into thinking that a man-made and enabled on paper – a fiction the “corporation” should come to have free speech – particularly since the history of corporations and combines is so checkered and spotted with indifference and opposition to this Republic and the constituents herein. What eva happened to equal protections.
What was the law that was repealed – that in effect limited pricing on medicine that had its research funded by the public??? who brought that legislation forward? who signed it in??? – Same thing with the restrictions on discharging student loans??? — Just like an alcoholic – the first step to correcting the problem is to admit the problem. Just like the best way to fix a mistake is to identify the mistake first.
Maybe we need a Democrats Anonymous (DA) and a Republicans Anonymous (RA) and an Economics Anonymous (EA)
Looking at all the alternatives we might consider something like the British National Health Service. The issues they do have generally relate to underfunding. That would not be so much of a problem in the US. If we are to consider health care a human right for all people resident in the US both legal and illegal doctors need to be on salary. Pharma needs to be subject to control. Firefighter paramedics do the most critical medical care we have on salary so why are doctors not? And if medical care is a human right and an obligation of the government how does the government not have the power to regulate prices and utilization? Think how many drugs and surgeries and implants and treatments are of no or minimal efficacy. At least the British have 70 years of mistakes that we can learn from.
I get it…..this is a money grab by the Congressmen representing poorer communities often in the south or cities (who have been consistently against campaign finance reform on the grounds that their constituents are poor and cannot fund them) and their allies, who are the major beneficiaries of pharma cash, before something does change because they are fully aware that nothing can continue to grow at 10% per year for ever. The lawyer/health insurance/medical and pharma party paid for a resounding win in November and now we can pay for it. Of course, the Real Estate/Religion/finance party’s candidate was no better. It will be a race to see if global warming driving massive migration and mortality or health care will trigger a revolution in the US. I urge all readers to watch Gore Vidal’s 1991 speech to the national press club on You Tube. Nothing new here.