Nobel Prize winner Angus Deaton and his wife Anne Case put the spotlight on a health care crisis that had managed to go almost entirely unnoticed: that of what they called an “AIDS-level” rise in deaths among whites with high school educations or less, aged 45-54. The top causes were a rise in substance abuse, most of all opioids and alcohol, and suicides.
As we’ll discuss shortly, a new story in the Washington Post today discusses another symptom of distress in rural communities: a sharp rise in hepatitis C and B cases. These are second-order effects of the sharp increase in opioid use. What is particularly distressing about this development is that the rise in hepatitis C cases is high among the young, those in their 20s and 30s.
As a reminder, from our of the original Case Deaton study, released in 2015:
One of the long standing patterns in economies showing economic growth is longer life spans, and falls are see the result of severe distress and dislocation, as took place in the period right after the fall of the Soviet Union, when the expectancies of adult men fell by over seven years.
The US has just become the first country to approach this appalling record. A stark warning about the level of distress in America comes from an important study by Angus Deaton, the 2015 Nobel prize winner in economics, and his wife Anne Case. We’ve embedded their short and readable article at the end of this post. The authors found that from 1999 to 2013, the death rate among non-Hispanic whites aged 45 to 54 with a high school education or less rose, while it fell in other age and ethnic groups. This is an HIV-level silent epidemic: AIDS killed an estimated 650,000 from the mid-1980s to present, while an estimated close to half-million died in half that time period who would have lived had their mortality rates fallen in line with the rest of the population. It is hard to overstate the significance of these findings.
And here are the key charts. This cross-country comparison shows how extreme an outlier these middle aged whites are:
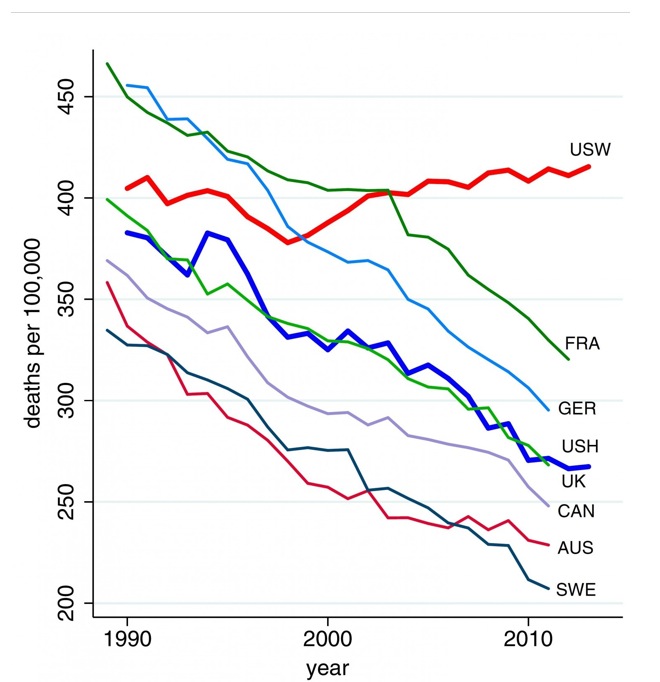
The authors linked the big culprits to despair, namely “poisoning” which is opioid abuse first and alcoholism second, and suicides.
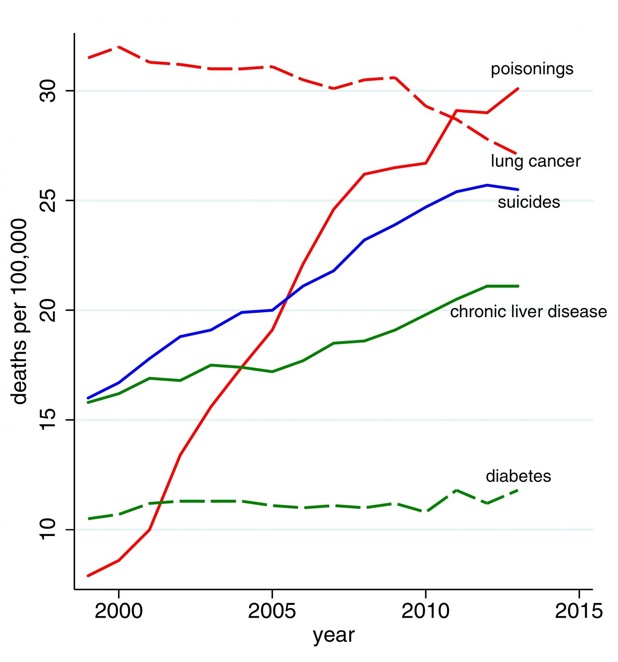
Case and Deaton published a new study earlier this year, with two more years of data. It showed that the patterns they found earlier were persisting. Their thesis (emphasis original):
We propose a preliminary but plausible story in which cumulative disadvantage from one birth cohort to the next—in the labor market, in marriage and child outcomes, and in health—is triggered by progressively worsening labor market opportunities at the time of entry for whites with low levels of education. This account, which fits much of the data, has the profoundly negative implication that policies—even ones that successfully improve earnings and jobs, or redistribute income—will take many years to reverse the increase in mortality and morbidity, and that those in midlife now are likely to do worse in old age than the current elderly.
The Washington Post story discusses the predictable and deadly knock-on effect of the sharp rise in opioid abuse in rural communities: that of a spike in level of hepatitis C. 80% to 85% of those who are infected with hepatitis C wind up with chronic hepatitis. The main vectors of transmission are sharing needles, unprotected sex, kidney dialysis, and handling blood in your line of work. In Australia, tattooing was a major hepatitis C transmission mechanism; I’m not sure if that is still true. Similarly, in the US, blood transfusions once accounted for a significant portion of hepatitis C infections; more stringent screening has cut that way down.
Because hepatitis C is, famously, a “silent killer,” where victims are often symptom-free for many years or experience only mild and intermittent loss of appetite and fatigue. From Epidemic.org:
A mild inflammatory response in which the infected individual is virtually asymptomatic but with potentially a high level of virus in the blood, may continue for years, even decades, before progressing significantly. More than 50-85% of infected individuals develop chronicity. In some 20-30% of patients, this may eventually result in cirrhosis (scarring of the liver tissue), and clinically in end-stage symptomatic liver disease. This appears to take, on average, about 20-30 years to develop. However, up to 1/3 may not develop significant liver damage at all, even after years..
Some patients with cirrhosis (scarring and nodule formation) may clinically do well for years, while others may deteriorate. The risk of liver cell cancer (hepatocellular carcinoma, HCC) increases over time.
Because alcohol is processed in the liver, excessive alcohol consumption can hasten liver damage. Damage progresses faster in people who are also HIV-positive.
In people who also have hepatitis B, the risk of developing liver cancer is increased. When it comes to cirrhosis, men tend to progress faster than women. Additionally, people over 40 with cirrhosis progress at a faster rate than younger people.
Epidemic.org lists some additional factors that often increase the speed of progression:
Importantly, the disease outcome is strongly influenced by co-morbid problems such as alcohol abuse, poorly controlled diabetes, iron accumulation in the liver and severe obesity.
Now to the Washington Post story:
The nation’s opioid epidemic has unleashed a secondary outbreak: the rampant spread of hepatitis C.
New cases of the liver disease have nearly tripled nationwide in just a few years, driven largely by the use of needles among drug users in their 20s and 30s, spawning a new generation of hepatitis C patients. Because a treatment that cures the disease costs tens of thousands of dollars, is limited by insurance and Medicaid, and is mostly unavailable to people who are still using illicit drugs, there probably will be financial and public health ramifications for decades to come….
“If we don’t cure a significant number of the people who are injecting, in 20 years from now, the hospitals in this part of the world will be flooded with these people with end-stage liver disease, which has no cure,” said Judith Feinberg, a professor of behavioral medicine and psychiatry at the West Virginia University School of Medicine. “I can see it coming at me like the headlights of a train. Just coming, coming, coming, and I’m thinking, ‘Doesn’t anybody want to jump out of the way?’”
The article later states that a six-month course of medication can run to over $100,000.
Not only is the treatment costly, but it is also debilitating. A friend of mine got hepatitis C, and has no idea how, since he was not an IV drug user, but since he was also HIV positive, I would assume his cause was unprotected sex. His course of treatment lasted six months and the side effects were comparable to chemotherapy. He was unable to work during this time. So even working class people who can manage to get treated face a second cost: loss of income and probable loss of employment.
Again from the Post:
According to the CDC, 34,000 people were estimated to have contracted hepatitis C in 2015, a number public health officials believe is low. In Massachusetts, officials estimate 300,000 people have the disease — and just half have received a formal diagnosis. Testing for the disease is not widespread, and because it’s possible to not display any symptoms, hepatitis C often goes undetected for decades until manifesting in severe, life-threatening liver disease.
“It’s the unidentified that scare me,” said Rahul Gupta, West Virginia’s health commissioner. “What I’m afraid of is that there are people out there not in the medical health care system and they’re spreading the disease.”
This data point explains why Feinberg and Gupta are so worried:
Thousands of people each year stream into West Virginia Health Right’s free clinic for clean needles, medication and, staffers hope, a hepatitis C test.
About half of the clinic’s clients have hepatitis C, chief executive Angie Settle said, discovered through a rapid-results test the clinic offers. The clinic, which sends mobile dental units around the state to offer free dental care, has started sending staff along to test people for hepatitis C.
West Virginia offers free treatments for those who are at an advanced stage of the drug and are sober. And here we see a how notions of fairness and morality can be at odds with public health goals. From a fairness perspective, those most deserving of help are the ones who are sickest and most deserving in the eyes of society. But from a public health perspective, you’d want to identify people most likely to be disease vectors, which would include young people, particularly ones who are very sexually active, since those early in the disease progression could conceivably be infecting others for decades.
As this slide show by Robert Greenwald, professor at Harvard Law School, and Ryan Clary, Executive Director of the National Viral Hepatitis Roundtable shows, sobriety requirements for Medicaid treatment vary by state as well as to how stringently they define “sobriety” and that, generally speaking, those restrictions are easing, but not all that much.
So here we see yet another cost of neoliberalism and the refusal of its adherents to see creating an adequate level of decently paid work and social safety nets as a requirement for a functioning society. America is on its way to being a country with more and more chronic illnesses. And the folks who have produced this result tout national competitiveness as a major goal. Instead, save for the medical industrial complex, America is becoming a less attractiveness on multiple fronts.


Judging from the government’s policy on dealing with this pandemic; I’d say everything is going according to plan.
Cynical? Not nearly enough so…
Wash post is wrong about hcv sexual transmission which is uncommon. Hepatitis B is sometimes caught through sex and just much more contagious. A spoonful of hbv positive blood would cause a swimming pool to be emptied and scrubbed with bleach. I used to teach blood borne illnesses to staff and that was an example we used. Doctors seem not to notice if treatments bankrupt or cause permanent disabiliies which the interferon sometimes does with only a small chance of curing HCV 1A the most common genotype. The new DAA tx is supposed to work much better but costs more unless you buy it in India.
It wasn’t the Washington Post that said unprotected sex with an infected person could lead to getting Hep C, it was HealthLine:
You can become infected with hepatitis C through contact with the blood of an infected person. You’re at risk of contracting the virus if you:
https://www.healthline.com/health/hepatitis-c/stages-progression#1
I think you are forgetting that anal sex can result in mild rectal bleeding of the “bottom” and blood is the vector of transmission. The person I know who got Hep C without ever using IV drugs or getting blood transfusions was gay. And there are straight women who like anal sex too.
I have a gay friend who got diagnosed with Hep about a year ago. He is a total straight edge though, so he didn’t have any clue how he got it. What really scares me about this is that most people don’t get tested for it and will think they are clean as they start a relationship… That is problematic regardless of sexual orientation.
I used to receive and follow up on communicable disease reports as a public health nurse. A 12 year old girl with no known risk factors came up positive, for B I think.
The only thing we could figure is that she got it from sharing a hair brush with a hepatitis positive relative who was staying in the home.
Early on, in the 90’s, I was told that the HIV virus would die in seconds on a counter top
but that hep B could live there a week. Not sure what the latest is on that but I think the comparison still holds.
I don’t know recent data either but I recall being told that if a spill of hbv blood on a window sill, for instance, had been cleaned up but not disinfected we could get it from leaning a bare arm on it even two weeks later! I wore long sleeves after hearing that. The swimming pool analogy used for HIV was they could just add more chlorine. I don’t know where infection control got their examples. As for HCV and boomers, I can’t help but think of the country docs of my childhood who gave me the job of boiling the syringe when they made house calls to us and wanted to give an injection. I was around five. Not very sterile and our dentists probably never heard of an autoclave.
Test$ + Diagno$i$ + Treatment$$$ = Luxurious Overpass Cardboard Box .. uh .. ‘Living’ ….
So I’m supposed to waltz over to Mr. BIG MEDICAL for an ‘intervention’ because … ?
Go ahead .. Pull the other distal !
Did your friend with Hep C get the new treatments? (I thought they were not supposed to be debilitating.) Interferon used to be debilitating for sure.
Their price is ridiculous:
https://www.statnews.com/2016/03/08/harvoni-hepatitisc-ads/
https://www.alternet.org/personal-health/84000-hep-c-drug-only-1500
It’s not necessarily urgent that someone asymptomatic get these drugs immediately and there may be some downsides, but yes hep C is serious and definitely a disease of despair.
Yes, the new treatments take three rather than six months and are much less debilitating. The cost, however, is a scandal. Gilead could massively treat the disease and still make a tidy profit, but they prefer to keep the epidemic alive and milk the desperate sufferers, govt, insurance companies, etc., forever. I have met people whose full-time job is to counsel people through the endless appeal process to try to get a single patient authorized for the treatment, which lists at $1,000 a day X 84 days. However, there are competing drugs now, and New York State made a deal with the others since Gilead wouldn’t negotiate a discount. It’s a terrible dilemma for advocates because you have to fight for people to have access to the cures while knowing all the time that you are lining these pharma creeps’ pockets.
–“AIDS-level” rise in deaths among whites with high school educations or less, aged 45-5—
It’s a bloody shame that mainstream media/entertainment elites are non-plussed about this. Great to see that our “progressive” elites are just as non-empathetic or value-judgemental as stereotypical 17th century Puritans.
How cares about ‘those people’—they deserved to get it.
California is also experiencing a cluster of deadly Hepatitis A outbreaks among homeless IV drug users. It’s spreading due to the extreme lack of sanitary toileting facilities. For example, my friend’s business backs up on an alley, and she has to call to have the accumulation of human excrement removed on a frequent basis. When she finally demanded a police response, the “urban outdoorsmen” simply upped the ante and began directing their defecations against the side of her building! Neoliberalism in action…
I have a family member who was diagnosed with hep-c, as well as liver cancer … She goes through the whole regime of chemo treatment for the hep, then later, then removal of several liver tumors, then a liver transplant, and is now doing well, courtesy of the anti-rejection drugs prescribed thereafter …. all covered by an insurance policy courtesy of a state employment pension .
I, on the other hand, have absolutely NO way to receive even a fraction of the kind of medical intervention she has at her disposal, without facing bankrupcy, or our feeble assets stolen that would otherwise go to my progeny, because, well, I didn’t have the foresight to work for a government entity, being recompenced through other, not so fortunate Taxpayers, such as yours truly.
This is but one example, of why I hold public employees, AND their respective union representation, with contempt. For me it’s up close, and in my face !
Why don’t you wish that everyone had the same benefits that your family member has? Why is holding her in contempt the default option?
I DO wish that everyone could receive the kind of care my family member received, but in responce to my complaint, all I get is (1.) Well there’s the Emergency Room .. or, alternatively, (2.) “I wish you had what I have” …
Well, if wishes were fishes, and all that ..
I also have a friend, who was diagnosed with hep-c, going through a similar drug regime .. but not needing a liver transplant, and when I bring up the fact of his pension ( he took early retirement from the county he worked for, knowing the score regarding the unsustainable actuarials in funding ) he takes it as a dish on him personally, instead of seeing this as a problem for the larger public, and I believe this is representitive of public employees, through their unions, nation-wide, because they are not seriously threatening their reps. and senators to make the changes neccessary to allow All of society’s members to have an in in what they themselves receive. It’s the same rational a dept. head of my little town used not too long ago when asked why our city needed to raise rates on utilities and road maint … because
THEIR healthcare rates were raising, irregardless of what us locals are having to deal with, with ever higher annual fees, assessments, and taxes, at least 1/4 of residents here needing assistance in paying their monthly utlilty bills, in an environment of doggedly high unemployment, and low-wage jobs for anyone NOT in city, county gov, medical, or military perveiw. THEY GOT THEIR’S ! … well, ain’t that grand !!
SIGNED, A Deplorable west of Seattle
Do other readers have experience that bears on this one way or the other?
Personally, I’d be curious to hear whether, in your opinion, this is also true of other unions. Also, do you feel like this is an attitude that has arisen over time, and was less prevalent among public employees in the past?
My daughter-in-law, who is extremely compassionate and voted for Sanders, was angered when her public employer started charging a higher premium for family insurance than for insurance for one person. I pointed out that I’d always paid a higher premium for insuring a whole family; that, after all, a family could be expected to use more medical care than one person; and that she was getting a huge bargain relative to what I paid. She was still unhappy, because it made a tight budget tighter.
OTOH, she’s very much in favor of Medicare for all. She thinks everyone should get the same deal she does.
Instead of complaining “not fair- you shouldn’t get that!”, you should lament “not fair- we all should get that!”
Don’t put words in my mouth ! .. that isn’t what I said, and frankly .. at this point .. with all the hinky $h!t that’$ being played, by both lessor, and greater mortals that I’ve been exposed to these last twenty or so years, ‘I can’t … to use what has now become a common cliche`… be cynical enough !!’
I’m not putting anything in your mouth, mate.
You got a raw deal. Instead of fulminating over how someone got a better deal than you did, I’m suggesting that you and everyone else demand a better deal.
Constructive criticism.
I am curious about the contempt in which you hold government employees AND their respective union representation – the union reps perhaps themselves being government employees elected to bargain for various benefits.
Some people argue against meaningful wages and health benefits ideologically, diehard against any socialist or government aid whatsoever. Others argue against help granted to known individuals considered unworthy of help, variously, because of gender or age or even personal relations with family members or former spouses or friends.
Others are envious.
What with single payor healthcare proposed as the best solution to your predicament (in the future, as I understand it, and with the poor luck that strikes many) please explain how any actions other than a collective response to cost would be effective.
Obviously, a broad engagement is needed with the deplorables to help them cope with their new normals. Didn’t the US do something like that for the native americans when they were put on reservations? That said, I seem to remember alcohol being used as a coping mechanism there. /sarc
There is more hepatitis out there than hep C
Outbreak of Hep A in San Diego
http://www.slate.com/blogs/the_slatest/2017/10/18/california_is_experiencing_the_second_worst_hepatitis_a_outbreak_in_the.html
15 years ago, an outbreak of Hep A in Pennsylvania
http://www.npr.org/templates/story/story.php?storyId=1510561
http://www.nytimes.com/2003/11/17/us/community-is-reeling-from-hepatitis-outbreak.html
There are vaccines against Hepatitis A & B (not C through E, that I know of) and one of the very nice things that a good county public health department will do is offer a period ‘vaccine day’ where (for a fee) everyone can stand in line & get a vaccine. When I say ‘pay a fee’ it varies if you are a kid, on Medicaid, or have insurance, but the prices look affordable. Here is a price sheet local to me.
http://www.ewashtenaw.org/government/departments/public_health/disease_control/vaccines-fees/immunization-fees-may-1
I am throwing this into comments as the commentariat enjoys talking about ‘Medicare for All’ which is great & I support, but we should also not forget the ‘we are all in it together’ public health type projects, and the local institutions that make public health possible. Americans can have great loyalty to local institutions even when we are pissed at “the gov’ment” and if we could deliver some important, basic health care through county government, that could promote citizen loyalty & attentiveness to a health care system that so often seems very remote
I didn’t have time to read this post yet. I was sitting in the doctor’s office this morning — and one of the drug company folks was sitting across from me waiting to talk to the doctor. Then it hit me and I asked him: “If Harvoni …
… [Gileads 99% cure of Hepatitis C which it sells in the US for $100,000 an 84 pill treatment] …
… is worth so much why don’t they knock off a truckload? They must keep it somewhere. Isn’t the Mafia interested?”
Later a whole gamut of criminal enterprises opened up for me. You could get a prescription and you could hit the pharmacy when you knew they had it (burglary or robbery). Harvoni could be the smuggling enterprise dream.
You are not going to get life imprison for smuggling kilos of prescription drugs (I don’t think). It is worth many time more per kilo than dangerous drugs. 84 pills weighs, what, about four ounces? Almost a million dollars per kilo (at US pharmacy prices). Cost to manufacture: maybe $2,000 — going by $150 a treatment for Sovaldi (I saw somewhere), the main ingredient. No raids, no payoffs — and no guilty conscience: you’re saving lives! :-)
Anti pharmaceutical TV ad:
I keep thinking of a scene I used to see on Seventh Avenue outside Madison Square Garden in the 70s. Two money trucks would park, one at the curb, one catercorner in the next lane, four guards would come out of the building, one with two boxes (presumably money) on a hand truck, one just behind him to one side, another ten feet behind him to the other side and one trailing thirty feet behind on the other, all guns drawn.
Well, you’d just need a little box with a dozen pill bottles to go way over a million smackolas with Harvoni. You could film it being delivered to a drug fortress. Once knowledge of extreme profit knocking over prescription drugs, all super expensive drugs,not just Harvoni, becomes widespread you’re going to have to protect them much more than, say, check cashing dollars — they are worth incomparably more.
* * * * * *
Another anti-big pharma medical murder angle:
Put up a countdown billboard showing how many years and days before Hepatitis C can be wiped out in this country — simultaneous with Gilead’s patent for Harvoni running down.
It is crazy to have a cure or Hepatitis C and to have to wait twenty years to use it. Especially ironic since it was VA research that got the cure going — until the VA researchers smelled money and took it over for themselves (took it to Ireland actually for lower intellectual property taxes) — the lead endocrinologist making a cool $446 million for himself (almost enough to manufacture enough to cure three million patients).
You want to go Breaking Bad on prescription drugs? (the medicinal kind, not opioids) — say by smuggling in from Canada? It would not work (sadly) Patients need to see a doctor to get the right drug & dosage (which is darn precise) and the likelihood that your local dealer has just the right drug & dosage is low. Sell your smuggled drugs to pharmacists / doctors? Nope, they need a paper trail & regulated supply chain for legal & liability reasons. For a few highly fungible drugs this might work, like how people sometimes use pet antibiotics on humans, but that isn’t enough to base a criminal syndicate around.
Although if you want to write a screenplay & turn it into a TV series I would watch the hell out of that. Good luck at the doctor’s office ! :-)
Mmm. Thanks for the heads up. Hep C patients (and others) can get accurate prescriptions even now. Just cannot pay for drug. I envision a high quality underground network — however much quality it takes to dole out the (Indian, Chinese, whomever) prescriptions rightk.
You doctor knows what you are really going to do but is not responsible as long as does not discuss it. Why wouldn’t she want to save your life?
Come to think — in the bad old days in the Bronx (60s, 70s) — there was widely known to be diet pill doctors deep south (149th street) who would put skinny patient son a scale and prescribe the drugs. My network (er, my idea — that’s all) would all be sub rosa — no visible median personnel — and ethical. And profitable as long as it maintained a reputation for quality and accuracy.
Cops might look the other way. They know people who need the drug(s) too. Could become like prohibition. Juries might not convict!
God help should any one of our favored government representitives be in need of Harvoni, or any other life-saving medication … not !
“So here we see yet another cost of neoliberalism and the refusal of its adherents to see creating an adequate level of decently paid work and social safety nets as a requirement for a functioning society.”
This is an important post. Thanks for the article.
adding: Neoliberals could care about creating the right economic conditions for a functioning society. Or, they could care about getting it all for themselves. Those two goals are mutually exclusive.
Morphine turns on NFKB, a master regulator of inflammation which worsens infection. The link with hepatitis and liver fibrosis is well known. Why is this surprising to coroners?
Morphine is also angiogenic in end-stage metastatic cancer, reducing expected lifespan.
Shades of AIDS. How fucking fabulous. Living in the Bay Area was nicely depressing back then.
I don’t know anything about Hepatitis, but I do know getting infected with HIV is not that easy; the more people infected however, the more opportunities, or chances, for new infections to occur. It’s simple numbers. So the most vulnerable tend to get it first, but increasing numbers like with HIV, or Hepatitis means the ever less likely get infected too.
One of the biggest reasons AIDS spread so far was not only the still serious stigma of being gay, which meant hiding that you had AIDS, or that anyone has died of it (obituary pages just full of people “dying after a brief illness.”) let alone HIV, but also the belief that it was earned because of “the lifestyle” or God’s Judgment for being a homosexual. So it got more chances to spread. Even after old ladies, children, and hemophiliacs started dying it still took far too long and people still kept trying to blame the dying. They must have done something to earn being sick. As if God would have people rotting to death as some divinely just punishment.
I’m guessing that like with the Reagan Administration, Congress and state governments not taking the epidemic seriously because it was “those people”‘dying, hepatitis might be getting the same dismissal for the same reason. More sick people who then add more chances to spread with more people needlessly dying. Maybe it’s time for another version of ACT UP. That organization was full of asses, but they did help finally getting serious attention paid to the epidemic.